Your body communicates through subtle signals that are easy to dismiss as normal stress or aging. When progesterone levels drop below optimal ranges, these signals become more persistent and can significantly impact your quality of life, fertility goals, and overall well-being. Understanding what your body is trying to tell you empowers you to take action and seek appropriate testing to identify hormonal imbalances that may be affecting your health.
Understanding Progesterone's Critical Role
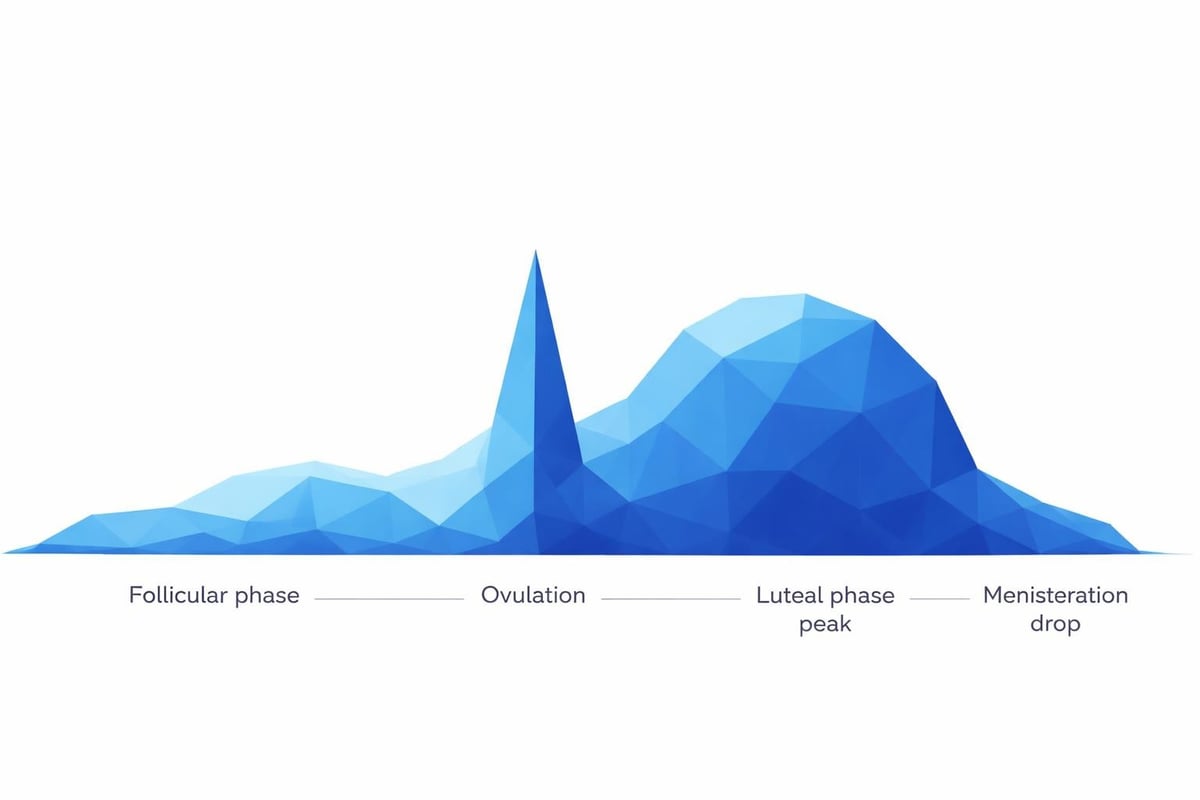
Progesterone serves as a cornerstone hormone in reproductive health, working in concert with estrogen to regulate menstrual cycles, support pregnancy, and maintain overall hormonal balance. This hormone rises after ovulation, preparing the uterine lining for potential implantation and supporting early pregnancy development.
Beyond reproduction, progesterone influences mood regulation, sleep quality, bone density, and metabolic function. When levels fall short, the ripple effects touch multiple body systems simultaneously.
The Menstrual Cycle Connection
During a typical cycle, progesterone production surges during the luteal phase (the two weeks following ovulation). This rise triggers specific changes in your body:
- Slight body temperature increase
- Thickening of the uterine lining
- Reduction in estrogen's stimulating effects
- Preparation for either pregnancy or menstruation
When progesterone production falters, this delicate timing mechanism breaks down. The result often manifests as irregular bleeding, unpredictable cycles, or difficulty conceiving.
Common Low Progesterone Symptoms You Shouldn't Ignore
Recognizing low progesterone symptoms requires attention to patterns rather than isolated incidents. These symptoms often cluster together, creating a constellation of signs that point toward hormonal imbalance.
Menstrual Irregularities and Bleeding Patterns
Abnormal bleeding stands among the most noticeable indicators of insufficient progesterone production. Without adequate progesterone to balance estrogen, the uterine lining may develop unevenly.
Common bleeding-related symptoms include:
- Spotting between periods
- Heavy menstrual flow lasting more than seven days
- Shortened cycles (less than 24 days)
- Prolonged light bleeding or spotting
- Missed periods despite not being pregnant
These patterns occur because progesterone normally stabilizes the endometrial lining. When levels drop, the lining may shed irregularly or excessively.
Fertility Challenges and Reproductive Health
For women trying to conceive, low progesterone symptoms can directly interfere with pregnancy achievement and maintenance. Progesterone creates the optimal environment for embryo implantation and early development.
| Fertility Impact | How Low Progesterone Affects It |
|---|---|
| Implantation | Inadequate uterine lining development prevents embryo attachment |
| Early Pregnancy | Insufficient support increases miscarriage risk in first trimester |
| Ovulation Quality | Weak ovulation produces less progesterone during luteal phase |
| Cycle Predictability | Irregular cycles make timing conception attempts difficult |
Women experiencing recurrent miscarriages should consider progesterone testing as part of their fertility evaluation. Medical News Today discusses how low levels contribute to pregnancy loss and other reproductive challenges.
Mood Changes and Mental Health Symptoms
Progesterone acts as a natural mood stabilizer by influencing neurotransmitter production in the brain. Declining levels often trigger psychological symptoms that many women attribute to stress or other factors.
Anxiety and irritability frequently intensify during the second half of the menstrual cycle when progesterone should naturally rise. Instead of the calming effect adequate progesterone provides, deficiency creates heightened emotional reactivity.
Depression symptoms may worsen or emerge, particularly during perimenopause when progesterone production begins its natural decline. Lesser-known symptoms like depression are often overlooked by healthcare providers who focus primarily on physical manifestations.
Sleep Disturbances and Fatigue
Progesterone promotes restful sleep by increasing the production of GABA, a calming neurotransmitter. When progesterone drops, sleep quality suffers in several ways:
- Difficulty falling asleep despite feeling tired
- Frequent nighttime wakings
- Non-restorative sleep leaving you exhausted upon waking
- Heightened sensitivity to environmental disruptions
This sleep disruption creates a cascade effect. Poor sleep worsens mood symptoms, reduces stress tolerance, and impairs the body's ability to regulate other hormones properly.
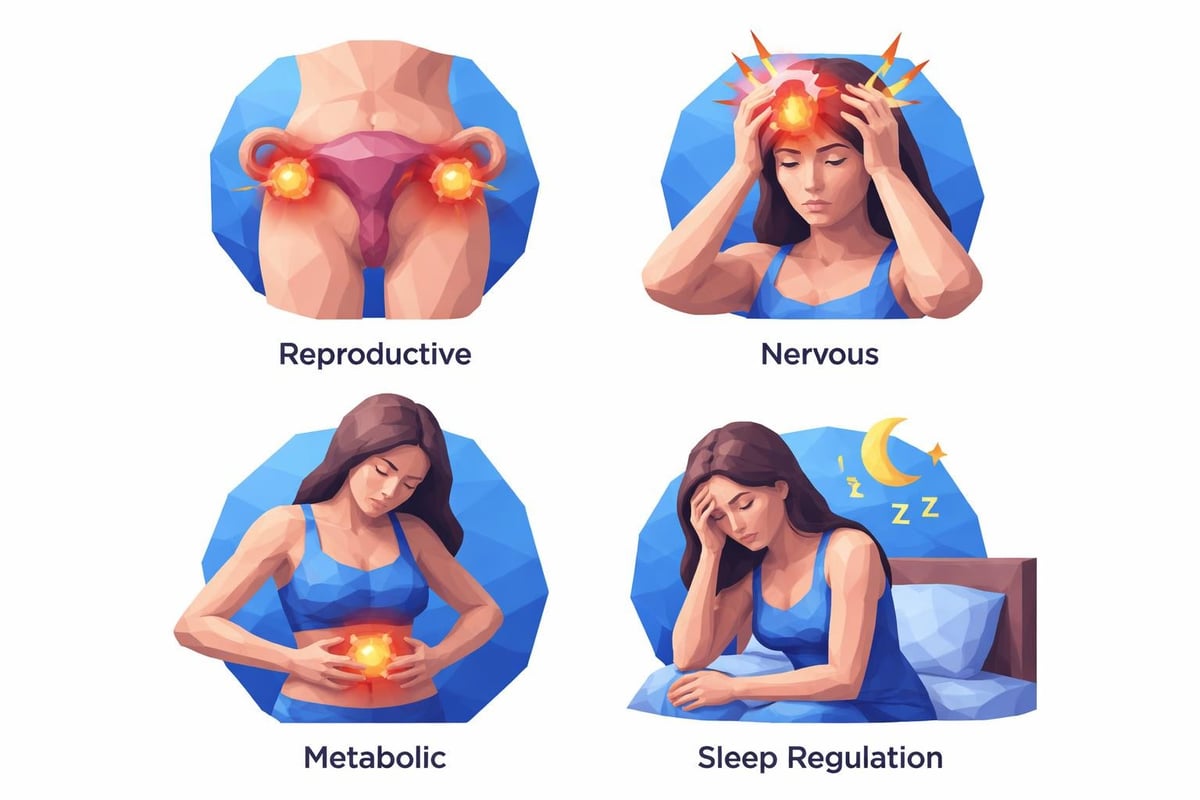
Physical Symptoms and Body Changes
Beyond reproductive and emotional effects, low progesterone symptoms manifest physically throughout the body. These changes often develop gradually, making them easy to dismiss initially.
Physical indicators include:
- Breast tenderness or fibrocystic changes
- Bloating and water retention
- Headaches or migraines, especially before menstruation
- Weight gain, particularly around the midsection
- Reduced libido
- Vaginal dryness
- Hot flashes or night sweats (especially during perimenopause)
Who Experiences Low Progesterone and Why
Understanding risk factors helps identify when testing becomes particularly important. Low progesterone symptoms don't affect all women equally, and certain life stages or conditions increase vulnerability.
Age-Related Progesterone Decline
Perimenopause represents the most common time for progesterone levels to drop. This transitional phase typically begins in the early to mid-40s, though some women experience changes earlier.
During perimenopause, ovulation becomes less consistent. Since ovulation triggers progesterone production, skipped ovulations mean missed opportunities for adequate progesterone synthesis. This creates months where estrogen acts unopposed, leading to estrogen dominance relative to progesterone.
Younger women may also experience low progesterone, particularly those with specific underlying conditions affecting ovarian function or hormone production.
Medical Conditions Affecting Progesterone Levels
Several health conditions directly impact the body's ability to produce or maintain adequate progesterone:
- Polycystic Ovary Syndrome (PCOS): Irregular ovulation reduces progesterone production
- Thyroid disorders: Both hypothyroidism and hyperthyroidism disrupt reproductive hormones
- Hypothalamic amenorrhea: Stress, excessive exercise, or low body weight suppress ovulation
- Premature ovarian insufficiency: Early decline in ovarian function before age 40
- Luteal phase defect: Shortened luteal phase with inadequate progesterone production
These conditions require targeted treatment addressing the root cause rather than just symptom management. Identifying underlying issues through comprehensive lab testing provides the foundation for effective treatment strategies.
Recommended Panel
Female Hormone Panel
Save $10This comprehensive panel measures all major female hormones: estrogen, progesterone, reproductive hormones (FSH/LH), and androgens (testosterone/DHEA-S) - essential for understanding hormonal balance.
Includes 7 biomarkers
$89
Lifestyle Factors and Stress
Chronic stress elevates cortisol, which can interfere with progesterone production. The body prioritizes cortisol synthesis when under prolonged stress, sometimes at the expense of reproductive hormones.
Additional lifestyle factors influencing progesterone include:
- High-intensity exercise without adequate recovery
- Restrictive dieting or caloric deficits
- Inadequate sleep over extended periods
- Exposure to endocrine-disrupting chemicals
- Significant body weight fluctuations
Testing for Progesterone Levels
Confirming low progesterone symptoms through testing eliminates guesswork and enables targeted treatment. Timing matters significantly when testing progesterone, as levels fluctuate dramatically throughout the menstrual cycle.
When to Test
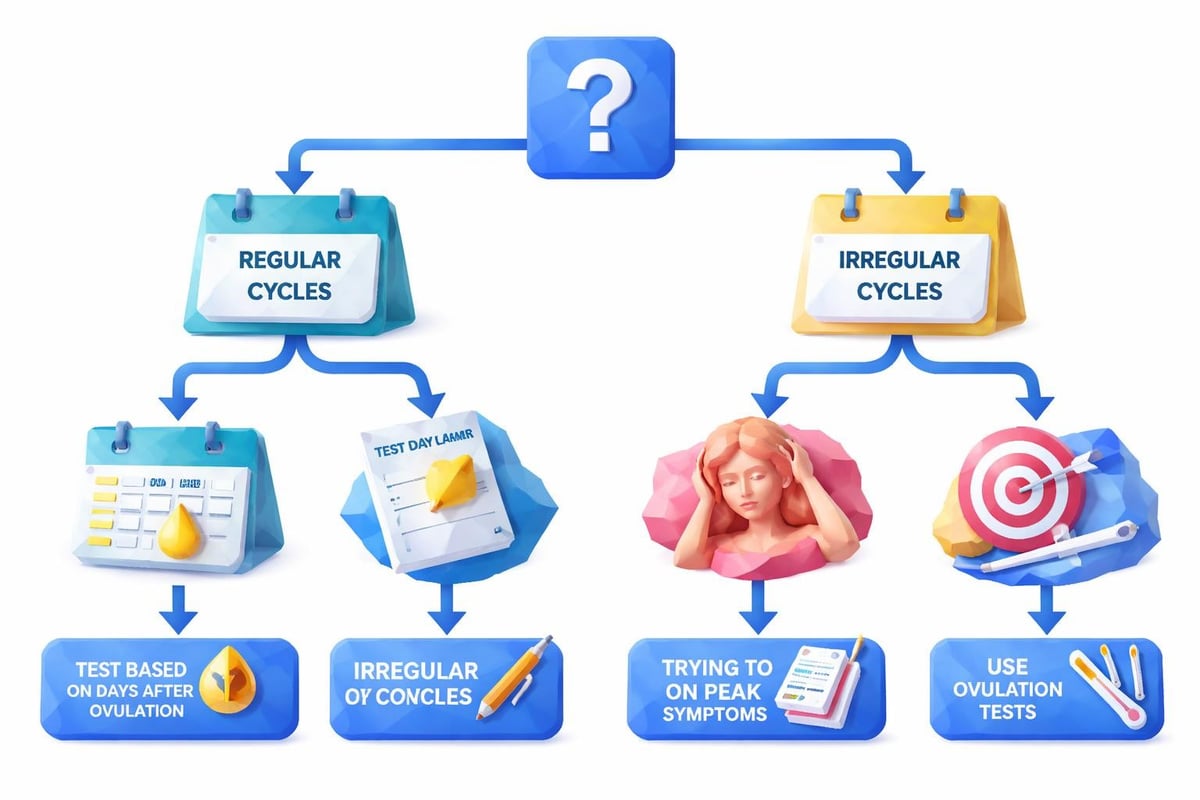
For women with regular cycles, progesterone testing should occur during the mid-luteal phase, approximately 7 days after suspected ovulation (typically day 21 of a 28-day cycle). This timing captures progesterone at its natural peak.
Women with irregular cycles face more complexity. Testing may need to occur multiple times to capture the luteal phase, or alternative testing methods like salivary hormone panels may provide better insights into patterns over time.
Testing Options and Accessibility
Modern lab testing has become increasingly accessible, removing barriers that previously prevented women from investigating hormonal concerns. Rather than waiting weeks for doctor appointments, you can now order lab tests without a doctor and receive results quickly.
| Testing Method | Advantages | Considerations |
|---|---|---|
| Serum Blood Test | Gold standard for accuracy; single time-point measurement | Requires precise cycle timing; one snapshot only |
| Saliva Testing | Multiple samples track daily fluctuations; convenient at-home collection | Less standardized reference ranges; some debate about accuracy |
| DUTCH Test | Comprehensive hormone metabolite analysis; includes cortisol patterns | Higher cost; requires specialized interpretation |
For many women, the convenience of labs without insurance through direct-to-consumer testing services provides both affordability and speed. Results typically arrive within 1-3 days, enabling faster decision-making about treatment approaches.
Recommended Test
Progesterone
Progesterone is a key reproductive hormone that prepares the uterus for pregnancy and supports early pregnancy. This test helps evaluate ovulation, fertility, and hormonal balance.
Includes 1 biomarkers
$14
Interpreting Your Progesterone Results
Numbers without context provide limited value. Understanding what progesterone levels mean requires consideration of several factors beyond the reference range printed on your lab report.
Normal Ranges and Context
Progesterone levels are measured in nanograms per milliliter (ng/mL). Reference ranges vary based on menstrual cycle phase:
- Follicular phase: 0.1-0.7 ng/mL
- Luteal phase: 2-25 ng/mL (optimal typically above 10 ng/mL)
- First trimester pregnancy: 10-44 ng/mL
- Postmenopausal: Below 1 ng/mL
These ranges represent population averages. Your optimal level might differ based on individual factors, symptoms, and health goals. Some practitioners consider levels below 10 ng/mL during the luteal phase inadequate for supporting pregnancy, even if technically within the reference range.
What Low Results Mean
When test results confirm low progesterone symptoms, the next step involves identifying why levels have dropped. A single low reading doesn't necessarily indicate a chronic problem, particularly if testing timing was off or an anovulatory cycle occurred.
Consistently low results across multiple properly-timed tests suggest either inadequate production (often from weak ovulation or luteal phase defect) or accelerated metabolism of progesterone.
Working with healthcare providers to interpret results within your complete health picture ensures appropriate next steps. Sometimes understanding lab results requires professional guidance to connect the numbers to your specific symptoms and health goals.
Treatment Approaches for Low Progesterone
Addressing low progesterone symptoms requires individualized approaches based on severity, underlying causes, age, and whether pregnancy is desired. Treatment strategies range from lifestyle modifications to bioidentical hormone supplementation.
Natural Support Strategies
Before considering pharmaceutical interventions, many women benefit from foundational lifestyle adjustments that support healthy progesterone production:
- Stress management: Meditation, yoga, or counseling to reduce chronic cortisol elevation
- Sleep optimization: Maintaining consistent sleep schedules and improving sleep hygiene
- Nutritional support: Adequate healthy fats, B vitamins, magnesium, and zinc
- Exercise balance: Moderate activity without excessive high-intensity training
- Weight optimization: Maintaining healthy body composition supports hormone balance
Certain supplements and foods may support progesterone production, though evidence varies. Vitex (chasteberry) has some research supporting its use for luteal phase support, though individual responses vary considerably.
Bioidentical Progesterone Therapy
When natural approaches prove insufficient, bioidentical progesterone supplementation offers direct hormone replacement. Available forms include:
- Oral micronized progesterone: Taken daily, often in the evening due to sedative effects
- Topical creams: Applied to skin, though absorption varies between individuals
- Vaginal suppositories: Direct delivery to reproductive tissues; common for fertility support
- Injections: Typically reserved for pregnancy support in specific circumstances
Hormone therapy risks and benefits require careful consideration with healthcare providers. While bioidentical progesterone generally carries fewer risks than synthetic progestins, individual factors influence safety and appropriateness.
Fertility-Specific Treatments
Women trying to conceive with confirmed low progesterone often benefit from luteal phase support. This typically involves progesterone supplementation beginning after ovulation and continuing through early pregnancy if conception occurs.
Fertility specialists may recommend progesterone support alongside other treatments addressing ovulation quality, such as:
- Clomiphene citrate or letrozole to strengthen ovulation
- Lifestyle modifications targeting underlying PCOS or metabolic concerns
- Thyroid optimization if thyroid dysfunction contributes to progesterone issues
- Stress reduction and sleep improvement to support overall reproductive health
Success with progesterone supplementation varies. Some women experience immediate symptom relief, while others require dosage adjustments or combination approaches addressing multiple hormonal imbalances simultaneously.
Monitoring Progress and Long-Term Management
Addressing low progesterone symptoms represents an ongoing process rather than a one-time fix. Regular monitoring ensures treatment effectiveness and allows for adjustments as your body's needs change.
Tracking Symptoms and Responses
Keeping detailed records of symptoms before, during, and after treatment provides valuable feedback about what's working. Consider tracking:
- Menstrual cycle length and bleeding patterns
- Mood changes throughout the cycle
- Sleep quality and energy levels
- Physical symptoms like breast tenderness or bloating
- Basal body temperature patterns (if trying to conceive)
This information helps healthcare providers fine-tune treatment approaches and identify whether additional testing or alternative strategies might benefit you.
Follow-Up Testing Recommendations
After initiating treatment, repeat testing typically occurs after 1-3 months to assess response. Timing depends on the intervention and your specific situation.
For women on progesterone supplementation, testing while taking the medication confirms adequate dosing. For those pursuing natural approaches, testing tracks whether lifestyle changes have successfully improved production.
The convenience of affordable lab test pricing makes regular monitoring more accessible, removing cost as a barrier to informed health management.
Adjusting Treatment Over Time
Your progesterone needs change as you age, as health conditions evolve, and as life circumstances shift. What works during perimenopause may differ from what's needed in your 30s while trying to conceive.
Regular communication with healthcare providers ensures treatment remains aligned with your current needs. Some women eventually discontinue supplementation as underlying issues resolve, while others require ongoing support, particularly through perimenopause and beyond.
Taking Control of Your Hormonal Health
Recognizing low progesterone symptoms empowers you to seek answers rather than accepting disruption as inevitable. Your body's signals deserve attention and investigation, especially when they interfere with quality of life, fertility goals, or overall well-being.
Modern testing accessibility removes traditional barriers to hormone evaluation. You no longer need to wait months for specialist appointments or navigate complex insurance approvals to understand what's happening in your body. Direct access to testing through services offering convenient lab locations puts hormone health information within reach quickly and affordably.
Whether you're navigating fertility challenges, perimenopause transitions, or unexplained symptoms affecting your daily life, understanding your progesterone status provides crucial information for targeted treatment. The combination of proper testing, informed interpretation, and appropriate intervention can transform how you feel and function.
Remember that hormonal balance rarely exists in isolation. Progesterone works within a complex network of other hormones, nutritional status, stress levels, and overall health. Comprehensive evaluation often reveals multiple factors contributing to symptoms, requiring multifaceted approaches for optimal results.
Understanding low progesterone symptoms and confirming them through testing represents the crucial first step toward hormonal balance and improved well-being. Whether you're concerned about fertility, managing perimenopause, or experiencing unexplained symptoms, accessible testing provides the answers you need to move forward with confidence. Justlabs makes hormone testing straightforward and affordable, delivering results in 1-3 days without requiring doctor visits or insurance approvals, so you can take control of your hormonal health on your timeline.