Joint pain affects millions of Americans each year, often signaling underlying conditions that range from temporary inflammation to chronic autoimmune diseases. While imaging studies and physical examinations provide valuable diagnostic information, laboratory testing remains essential for identifying the specific cause of joint discomfort. Understanding which lab tests for joint pain your healthcare provider might order can help you prepare for evaluation and interpret your results more effectively.
Understanding the Role of Laboratory Testing in Joint Pain Diagnosis
Laboratory tests serve as critical tools for distinguishing between mechanical joint problems and systemic inflammatory conditions. When you experience persistent joint pain, swelling, or stiffness, blood work can reveal inflammatory processes, autoimmune activity, or metabolic imbalances that aren't visible through imaging alone.
Blood tests complement clinical assessment by:
- Measuring inflammation levels throughout your body
- Detecting specific antibodies associated with autoimmune conditions
- Identifying metabolic disorders like gout
- Monitoring disease progression over time
- Guiding treatment decisions
The comprehensive approach to diagnosing joint problems typically combines patient history, physical examination, imaging studies, and targeted laboratory testing. Each component provides unique insights that create a complete diagnostic picture.
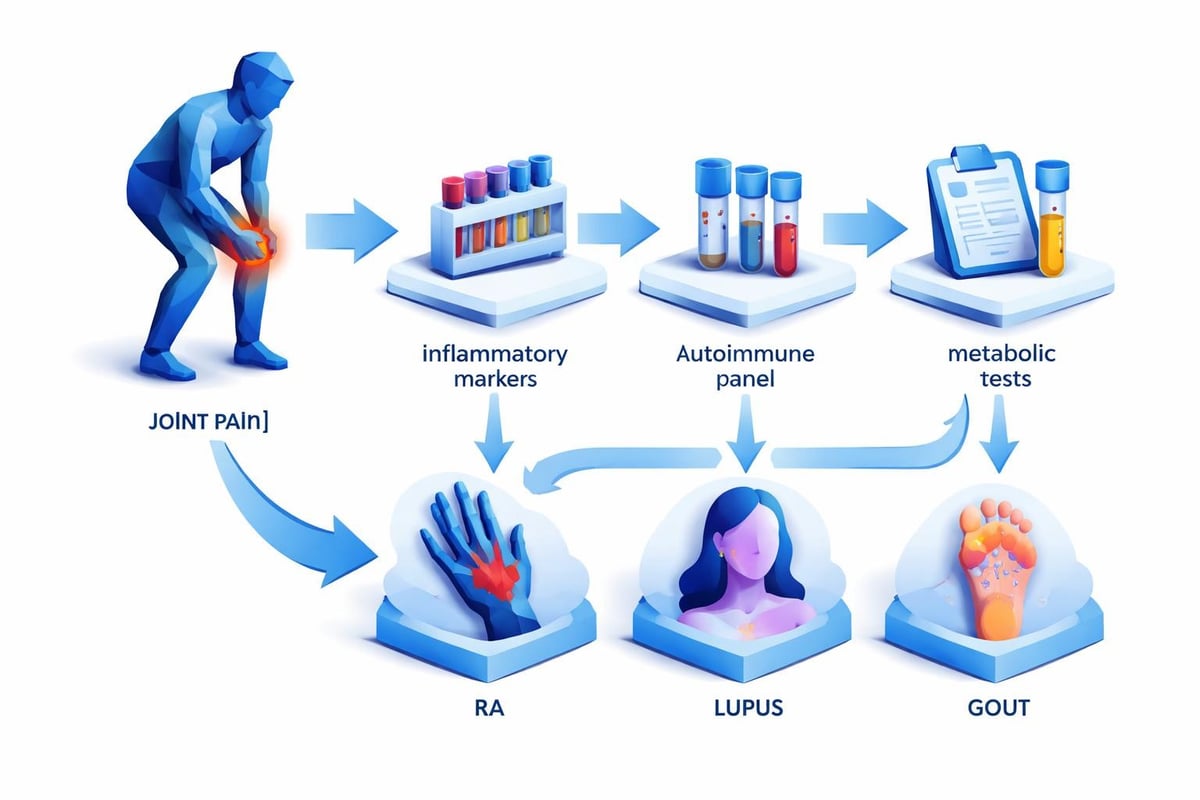
Essential Blood Tests for Inflammatory Joint Conditions
Complete Blood Count (CBC)
A complete blood count serves as a foundational screening test when evaluating joint pain. This test measures red blood cells, white blood cells, and platelets, providing information about overall health and potential inflammatory processes.
Anemia frequently accompanies chronic inflammatory arthritis, while elevated white blood cell counts may indicate infection or active inflammation. Platelet levels also rise during inflammatory episodes, offering another marker of disease activity.
Erythrocyte Sedimentation Rate (ESR)
The erythrocyte sedimentation rate measures how quickly red blood cells settle in a test tube over one hour. Higher sedimentation rates indicate increased inflammation somewhere in the body, though this test lacks specificity for any particular condition.
ESR values help clinicians:
- Establish baseline inflammation levels
- Monitor treatment effectiveness
- Detect disease flares
- Differentiate inflammatory from non-inflammatory arthritis
Values above 20 mm/hr for men and 30 mm/hr for women typically warrant further investigation, especially when accompanied by joint symptoms.
Recommended Panel
Inflammation Panel
Save $2Chronic inflammation is the hidden driver of heart disease, cancer, and accelerated aging. This panel measures the key markers that reveal whether silent inflammation is damaging your body.
Includes 17 biomarkers
$52
Fasting required
C-Reactive Protein (CRP)
C-reactive protein rises rapidly in response to inflammation, making it more sensitive than ESR for detecting acute inflammatory processes. This protein, produced by the liver, increases within hours of inflammatory stimulus and decreases quickly when inflammation resolves.
High-sensitivity CRP (hs-CRP) testing provides even more precise measurements, though standard CRP testing suffices for most joint pain evaluations. According to research on blood tests for joint pain, combining CRP with ESR offers superior diagnostic value compared to either test alone.
Autoimmune Antibody Testing for Rheumatoid Arthritis
Rheumatoid Factor (RF)
Rheumatoid factor represents an antibody that targets other antibodies in the body, creating immune complexes that contribute to joint inflammation. Approximately 70-80% of rheumatoid arthritis patients test positive for RF, though this antibody also appears in other conditions and occasionally in healthy individuals.
| RF Level | Clinical Significance |
|---|---|
| Negative (<15 IU/mL) | Does not rule out RA; seronegative RA exists |
| Low Positive (15-30 IU/mL) | May indicate early RA or other conditions |
| Moderate Positive (30-100 IU/mL) | Supports RA diagnosis with symptoms |
| High Positive (>100 IU/mL) | Strong correlation with aggressive RA |
Anti-Cyclic Citrullinated Peptide (Anti-CCP)
Anti-CCP antibodies demonstrate higher specificity for rheumatoid arthritis than rheumatoid factor, meaning positive results more reliably indicate RA rather than other conditions. These antibodies can appear years before symptoms develop, allowing for earlier diagnosis and intervention.
The blood, fluid, and tissue tests for arthritis outlined by the Arthritis Foundation emphasize the importance of combining RF and anti-CCP testing for optimal diagnostic accuracy.
Recommended Test
Rheumatoid Factor
Rheumatoid Factor is an autoantibody commonly elevated in rheumatoid arthritis. This test helps diagnose RA and assess disease severity, though RF can also be elevated in other conditions.
Includes 1 biomarkers
$8
Key advantages of anti-CCP testing:
- Detects RA in early stages
- Predicts more aggressive disease courses
- Identifies patients who may develop erosive joint damage
- Helps differentiate RA from other inflammatory arthritis types

Lab Tests for Systemic Lupus Erythematosus
Antinuclear Antibody (ANA)
The antinuclear antibody test screens for autoimmune conditions by detecting antibodies that attack components within cell nuclei. While not specific to lupus, positive ANA results appear in over 95% of lupus patients, making this test an essential screening tool.
ANA testing reports both titer (concentration) and pattern. Higher titers generally indicate stronger autoimmune activity, though some healthy individuals test positive at low titers. The pattern observed under microscopy provides clues about specific autoimmune conditions.
Anti-Double-Stranded DNA (Anti-dsDNA)
Anti-dsDNA antibodies demonstrate high specificity for systemic lupus erythematosus, appearing in approximately 70% of patients with active disease. These antibody levels often correlate with disease activity, rising during flares and declining during remission.
Testing for anti-dsDNA becomes particularly important when evaluating joint pain accompanied by skin rashes, fatigue, or kidney symptoms. This marker helps distinguish lupus from other autoimmune conditions that may present with similar joint manifestations.
Complement Levels (C3 and C4)
Complement proteins participate in immune system function, and their levels decrease when consumed during active lupus inflammation. Low C3 and C4 levels, especially combined with positive anti-dsDNA antibodies, strongly suggest active lupus with potential organ involvement.
Monitoring complement levels over time helps assess disease activity and treatment response, providing objective data beyond symptom reporting.
Metabolic Testing for Crystal-Induced Arthropathies
Serum Uric Acid
Elevated uric acid levels characterize gout, though not all individuals with high uric acid develop gout, and some gout patients maintain normal uric acid during acute attacks. Serum uric acid testing works best for monitoring treatment effectiveness rather than diagnosing acute gout episodes.
Normal uric acid ranges:
- Men: 3.4-7.0 mg/dL
- Women: 2.4-6.0 mg/dL
- Gout risk increases significantly above 7.0 mg/dL
Levels above 9.0 mg/dL carry substantially higher risk for gout attacks and urate crystal deposition in joints and soft tissues.
Recommended Test
Uric Acid
Uric acid is a waste product from purine breakdown. Elevated levels can cause gout (painful joint inflammation) and may indicate kidney problems or increased cardiovascular risk.
Includes 1 biomarkers
$5
Synovial Fluid Analysis
While technically not a blood test, synovial fluid analysis provides definitive diagnosis for crystal-induced arthropathies through direct examination of joint fluid. This procedure, called arthrocentesis, involves extracting fluid from affected joints for laboratory evaluation.
The fluid undergoes several analyses:
- Visual inspection for clarity, color, and viscosity
- Microscopy to identify uric acid or calcium pyrophosphate crystals
- Cell count to assess inflammation severity
- Culture to rule out infectious arthritis
- Glucose and protein measurements
Needle-shaped uric acid crystals confirm gout, while rhomboid-shaped calcium pyrophosphate crystals indicate pseudogout. These fluid and tissue tests for arthritis offer diagnostic certainty that blood tests alone cannot provide.
Additional Specialized Testing
HLA-B27 Genetic Marker
The HLA-B27 gene associates strongly with spondyloarthropathies, a group of inflammatory conditions affecting the spine and other joints. Approximately 90% of ankylosing spondylitis patients carry this genetic marker, compared to 6-8% of the general population.
Testing for HLA-B27 becomes relevant when evaluating lower back pain with inflammatory characteristics, peripheral joint pain accompanied by enthesitis (inflammation where tendons attach to bone), or family history of spondyloarthropathies.
Lyme Disease Serology
In regions where Lyme disease is endemic, testing for Borrelia burgdorferi antibodies helps identify this tick-borne infection that frequently causes joint pain, particularly in large joints like knees. Two-tiered testing using ELISA followed by Western blot confirmation provides optimal diagnostic accuracy.
Parvovirus B19 Antibodies
Parvovirus B19 infection can trigger acute polyarticular arthritis, especially in adults. Testing for IgM and IgG antibodies distinguishes recent infection from past exposure, helping identify viral arthritis that may mimic rheumatoid arthritis.
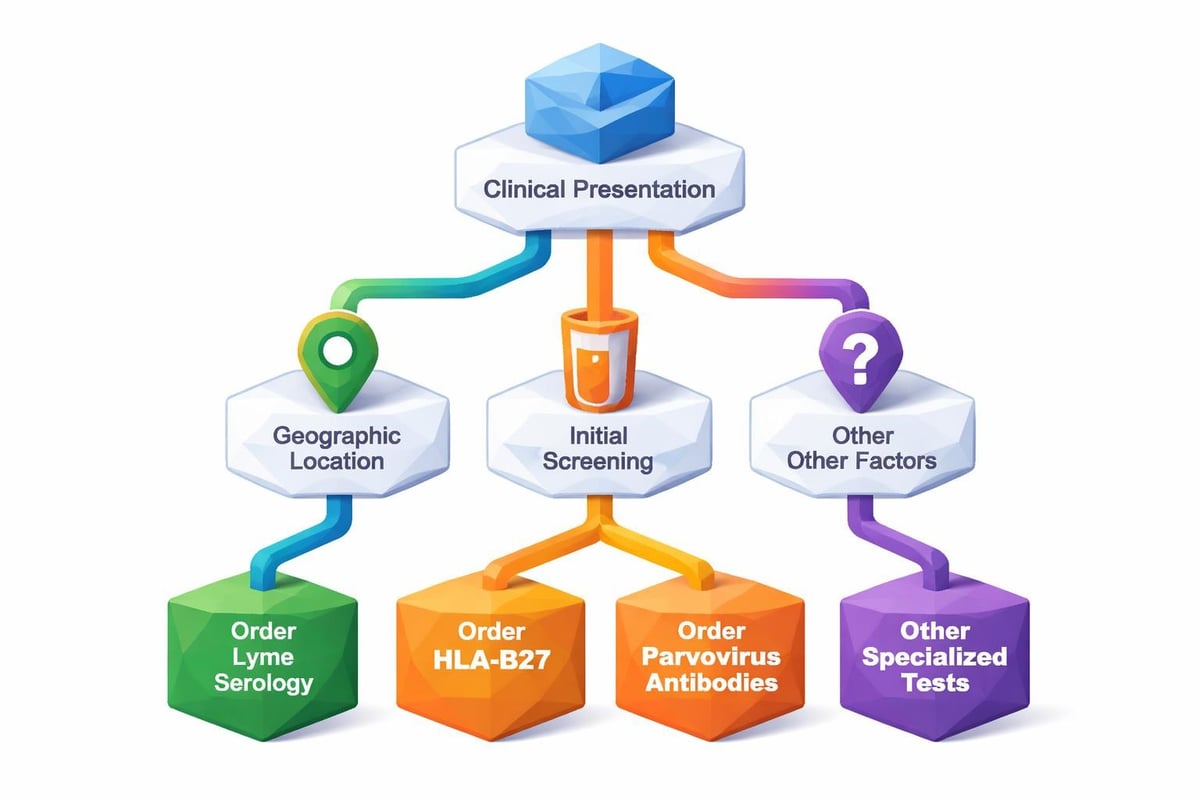
Interpreting Lab Test Results
Understanding lab tests for joint pain requires recognizing that no single test provides absolute diagnostic certainty. Results must be interpreted within clinical context, considering symptoms, physical findings, and imaging studies.
Important interpretation principles:
- False positives occur: Healthy individuals occasionally test positive for autoimmune markers
- False negatives happen: Early disease may not yet produce detectable antibodies
- Timing matters: Some tests perform better during active flares versus remission
- Trends outweigh single values: Serial testing reveals disease progression more reliably than isolated results
Many patients benefit from understanding their results through resources like understanding lab results, which explains common testing terminology and reference ranges.
Accessing Lab Tests for Joint Pain Without Traditional Barriers
Traditional pathways to laboratory testing often require insurance authorization and multiple healthcare appointments, creating delays when you need answers about persistent joint pain. The ability to order labs without a doctor provides faster access to diagnostic information.
Self-pay laboratory testing eliminates insurance requirements while maintaining quality standards through CLIA-certified facilities. Results typically arrive within 1-3 days, allowing you to share findings with healthcare providers promptly.
| Traditional Testing | Direct-Access Testing |
|---|---|
| Requires doctor visit | Order online directly |
| Insurance approval needed | Transparent self-pay pricing |
| 1-2 weeks for results | 1-3 days for results |
| Unknown costs until billing | Upfront pricing available |
| Limited test selection | Comprehensive test menu |
For those managing costs independently, exploring labs without insurance options reveals affordable alternatives to traditional testing pathways.
When to Consider Laboratory Testing
Not all joint pain requires extensive laboratory workup. Mechanical issues like osteoarthritis often need only imaging studies, though the tests for osteoarthritis may include limited blood work to rule out inflammatory conditions.
Consider lab testing when experiencing:
- Joint pain persisting beyond 6 weeks despite conservative treatment
- Morning stiffness lasting over 30 minutes
- Multiple joint involvement, especially symmetrical patterns
- Systemic symptoms like fever, rash, or unexplained weight loss
- Family history of autoimmune disease
- Rapid onset of severe joint swelling
Early testing allows for prompt diagnosis and treatment initiation, potentially preventing irreversible joint damage in inflammatory conditions.
Cost Considerations and Financial Planning
Laboratory testing costs vary dramatically based on insurance coverage, facility choice, and negotiated rates. Understanding pricing beforehand enables better financial planning and informed healthcare decisions.
The comprehensive overview of laboratory tests for evaluating joint pain emphasizes selecting appropriate tests based on clinical suspicion rather than ordering extensive panels indiscriminately.
Cost-saving strategies include:
- Bundling related tests when ordering
- Choosing direct-access testing facilities
- Using FSA/HSA funds for eligible tests
- Comparing prices across different laboratories
- Requesting only clinically indicated tests
Many health savings account holders can apply their FSA/HSA eligible tests funds toward diagnostic workups, reducing out-of-pocket expenses significantly.
Creating Your Testing Plan
Developing an effective testing strategy requires balancing comprehensive evaluation with cost efficiency. Starting with screening tests and adding specialized testing based on initial results prevents unnecessary expenses while ensuring diagnostic thoroughness.
Suggested tiered approach:
First Tier: Basic Inflammatory Screening
- Complete blood count
- Erythrocyte sedimentation rate
- C-reactive protein
- Comprehensive metabolic panel
Second Tier: Autoimmune Evaluation
- Rheumatoid factor
- Anti-CCP antibodies
- Antinuclear antibodies
- Serum uric acid
Third Tier: Condition-Specific Testing
- Anti-dsDNA and complement levels for suspected lupus
- HLA-B27 for spondyloarthropathy concerns
- Lyme serology in endemic regions
- Synovial fluid analysis for definitive crystal identification
This approach, recommended by the primary care assessment guidelines, maximizes diagnostic yield while controlling costs.
Monitoring Disease Activity Over Time
Once diagnosed with inflammatory arthritis or autoimmune conditions, periodic laboratory testing tracks disease activity, guides treatment adjustments, and identifies potential complications.
Monitoring frequency depends on disease type, treatment intensity, and clinical stability. Active disease or new medication initiation typically requires more frequent testing than well-controlled conditions on stable treatment regimens.
Common monitoring intervals:
- Newly diagnosed or unstable disease: Every 4-8 weeks
- Stable disease on medication: Every 3-6 months
- Remission with minimal treatment: Every 6-12 months
Trending values over time provides more meaningful information than isolated test results, revealing whether interventions effectively control inflammation and prevent disease progression.
Laboratory testing provides essential diagnostic information when joint pain persists, helping distinguish inflammatory conditions like rheumatoid arthritis, lupus, and gout from mechanical joint problems. Understanding which tests offer the most value for your specific symptoms empowers you to work effectively with healthcare providers while managing costs. Justlabs offers convenient access to comprehensive lab testing with transparent pricing and quick results, allowing you to take control of your joint health evaluation without insurance delays or hidden fees.