Understanding your body's stress response starts with measuring cortisol, often called the stress hormone. Whether you're experiencing chronic fatigue, unexplained weight changes, or persistent anxiety, a cortisol test can provide valuable insights into how your adrenal glands function and how your body manages stress. This diagnostic tool has become increasingly accessible as more people seek direct answers about their hormone health without the traditional barriers of scheduling doctor appointments and navigating insurance complexities.
What Cortisol Does in Your Body
Cortisol serves as one of your body's most critical hormones, produced by the adrenal glands that sit atop each kidney. This steroid hormone regulates numerous essential functions including metabolism, blood sugar levels, immune response, and blood pressure.
Your cortisol levels naturally fluctuate throughout the day in a pattern called the diurnal rhythm. Typically, cortisol levels peak in the early morning hours, usually around 6-8 AM, helping you wake up and feel alert. As the day progresses, levels gradually decline, reaching their lowest point around midnight when your body prepares for sleep.

The Stress Connection
When you encounter a stressful situation, your brain signals the adrenal glands to release cortisol. This response provides energy and focus to handle immediate challenges. However, chronic stress can disrupt this delicate balance.
Key functions of cortisol include:
- Converting proteins and fats into usable energy
- Reducing inflammation throughout the body
- Regulating blood pressure and cardiovascular function
- Controlling sleep-wake cycles
- Managing how your body uses carbohydrates, fats, and proteins
Problems arise when cortisol levels remain consistently elevated or drop too low. Both scenarios can trigger a cascade of health issues that significantly impact your quality of life.
Recommended Test
Cortisol, Total
Cortisol is your body's primary stress hormone, produced by the adrenal glands. This test measures total cortisol levels to assess adrenal function and stress response.
Includes 1 biomarkers
$15
Why You Might Need Cortisol Testing
Healthcare providers recommend cortisol testing for various symptoms and conditions. Recognizing when testing becomes necessary helps you address potential hormone imbalances before they escalate.
Common Symptoms of High Cortisol
People with elevated cortisol levels often experience distinct physical changes. Weight gain, particularly around the midsection and face, ranks among the most visible indicators. You might also notice:
- Purple or pink stretch marks on the abdomen, thighs, or arms
- Thinning skin that bruises easily
- Muscle weakness, especially in the upper arms and thighs
- High blood pressure resistant to standard treatments
- Elevated blood sugar or type 2 diabetes
- Mood changes including anxiety, depression, or irritability
These symptoms may indicate Cushing's syndrome, a condition characterized by prolonged exposure to high cortisol levels.
Signs of Low Cortisol
Insufficient cortisol production presents a different set of challenges. Understanding low cortisol symptoms helps identify potential adrenal insufficiency or Addison's disease.
| Symptom Category | Specific Indicators |
|---|---|
| Energy Levels | Chronic fatigue, weakness, decreased stamina |
| Physical Changes | Unexplained weight loss, low blood pressure, dizziness |
| Skin Changes | Darkening of skin (hyperpigmentation), especially in scars and skin folds |
| Digestive Issues | Loss of appetite, nausea, abdominal pain, salt cravings |
| Mental Health | Depression, mood instability, reduced motivation |
Types of Cortisol Tests Available
Medical testing offers several methods to measure cortisol levels, each serving specific diagnostic purposes. The choice depends on your symptoms, suspected condition, and what your healthcare provider needs to evaluate.
Blood Cortisol Test
The blood test represents the most common approach. A healthcare professional draws blood from a vein, typically in your arm, during the morning when cortisol naturally peaks. Blood cortisol testing provides a snapshot of your hormone levels at a specific moment.
Some situations require two blood draws: one in the morning and another in late afternoon or evening. This comparison reveals whether your cortisol follows the expected diurnal pattern.
Urine Cortisol Test
A 24-hour urine collection measures your total cortisol output over a full day. The urine cortisol test captures fluctuations throughout the day, offering a comprehensive view of your adrenal function.
Collection process involves:
- Discarding the first morning urine
- Collecting all urine for the next 24 hours in a provided container
- Storing the container in a refrigerator during collection
- Returning the complete sample to the laboratory
This method proves particularly useful for diagnosing Cushing's syndrome, as it shows average cortisol production rather than a single point in time.
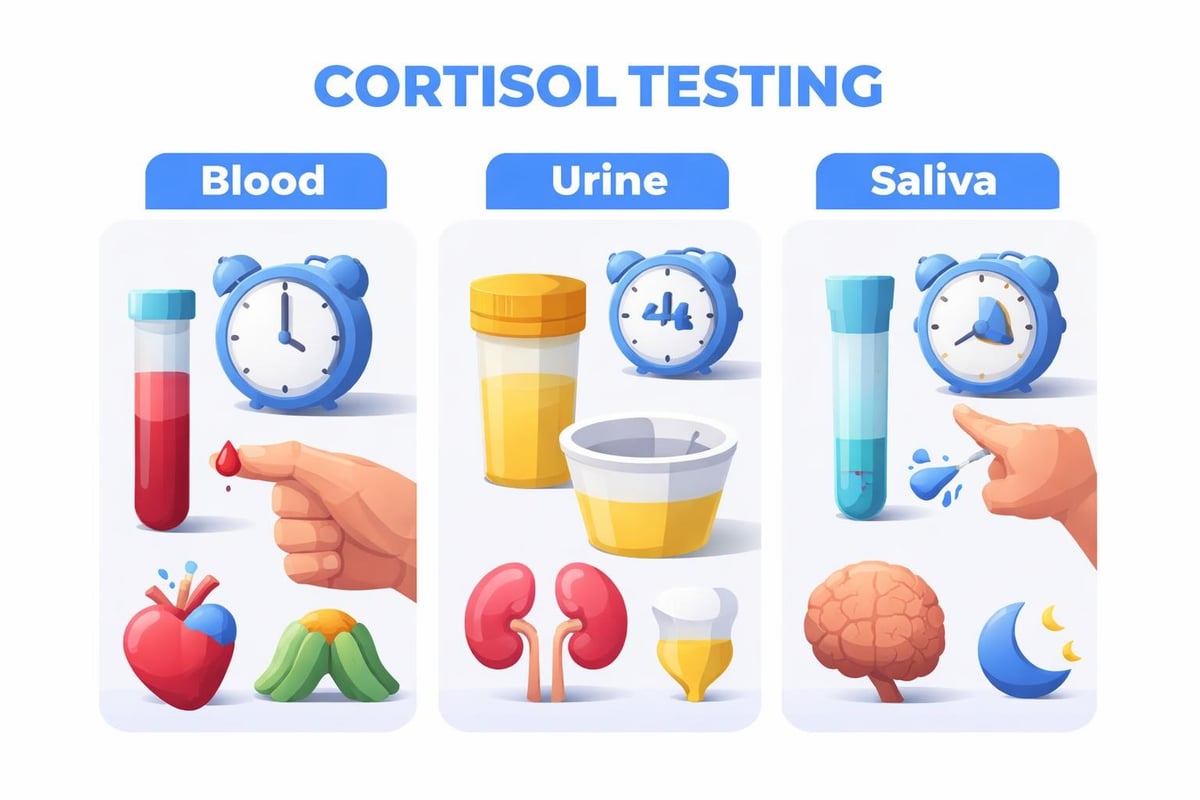
Saliva Cortisol Test
Saliva testing has gained popularity for its convenience and ability to measure free, biologically active cortisol. You collect saliva samples at specific times, often late at night when cortisol should be at its lowest.
This non-invasive method works well for detecting conditions like Cushing's syndrome, where nighttime cortisol remains elevated when it should naturally decline.
Stimulation and Suppression Tests
Beyond basic measurements, specialized tests challenge your adrenal glands to assess their responsiveness. The ACTH stimulation test involves injecting synthetic ACTH (adrenocorticotropic hormone) and measuring how cortisol levels respond.
Conversely, dexamethasone suppression tests use synthetic cortisol to evaluate whether your body appropriately decreases natural cortisol production. These advanced tests help pinpoint specific adrenal disorders.
Preparing for Your Cortisol Test
Proper preparation ensures accurate results. Several factors can influence cortisol levels, and understanding these helps you avoid false readings.
Medication Considerations
Certain medications affect cortisol production or measurement. Inform your testing provider about all medications, particularly:
- Oral contraceptives or hormone replacement therapy
- Corticosteroids like prednisone or hydrocortisone
- Anti-seizure medications
- Synthetic thyroid hormones
- Psychiatric medications
Your provider may recommend temporarily stopping specific medications before testing, but never discontinue prescriptions without professional guidance.
Lifestyle Factors
Physical and emotional stress directly impact cortisol levels. Research on cortisol testing reliability demonstrates how various factors influence results.
Before your test:
- Avoid vigorous exercise for 24 hours
- Get adequate sleep the night before
- Minimize stress and anxiety when possible
- Fast if instructed (usually for morning blood tests)
- Avoid alcohol for 24 hours prior
Timing matters significantly. Morning blood tests typically occur between 7-9 AM when cortisol peaks naturally. Late-night saliva tests should happen between 11 PM and midnight.
Understanding Your Test Results
Cortisol test interpretation requires context. Normal ranges vary based on testing method, time of day, and the laboratory performing the analysis.
Normal Cortisol Ranges
Blood cortisol measurements in the morning typically fall between 10-20 micrograms per deciliter (mcg/dL), though ranges vary by laboratory. Afternoon levels should measure lower, around 3-10 mcg/dL.
For 24-hour urine tests, normal total cortisol excretion ranges from 10-100 micrograms per 24 hours. Saliva tests measured at midnight should show levels below 0.09 mcg/dL.
| Test Type | Sample Timing | Typical Normal Range |
|---|---|---|
| Blood | 7-9 AM | 10-20 mcg/dL |
| Blood | 4-6 PM | 3-10 mcg/dL |
| Urine | 24-hour collection | 10-100 mcg/24hr |
| Saliva | 11 PM - Midnight | < 0.09 mcg/dL |
Remember that these represent general guidelines. Your healthcare provider interprets results based on your specific situation, symptoms, and medical history.
What Elevated Results Mean
High cortisol levels warrant further investigation to identify the underlying cause. Cushing's syndrome remains the primary concern with consistently elevated readings.
Causes of high cortisol include:
- Pituitary tumors producing excess ACTH
- Adrenal gland tumors
- Ectopic tumors in other organs producing ACTH
- Chronic stress or severe depression
- Obesity
- Poorly controlled diabetes
Not all elevated results indicate serious disease. Temporary elevation can result from acute illness, pregnancy, or medications. Factors affecting cortisol assays include body composition and oral contraceptive use, which may necessitate adjusted reference ranges.
Interpreting Low Results
Insufficient cortisol production suggests adrenal insufficiency, either primary (Addison's disease) or secondary (pituitary dysfunction).
Primary adrenal insufficiency occurs when:
- Adrenal glands are damaged by autoimmune disease
- Infections like tuberculosis affect the adrenal glands
- Genetic disorders impair adrenal development
- Surgical removal of adrenal glands
Secondary adrenal insufficiency develops when the pituitary gland fails to produce adequate ACTH, often due to tumors, radiation therapy, or prolonged corticosteroid use that suppresses natural hormone production.
Follow-Up Testing and Diagnosis
A single abnormal result rarely provides definitive diagnosis. Most conditions require additional testing to confirm findings and identify root causes.
Additional Hormone Panels
Comprehensive evaluation often includes measuring ACTH levels alongside cortisol. This combination helps distinguish between different types of adrenal disorders.
High cortisol with high ACTH suggests pituitary-driven Cushing's disease or ectopic ACTH production. High cortisol with low ACTH points toward adrenal tumors producing cortisol independently.
Low cortisol with high ACTH indicates primary adrenal insufficiency, while low cortisol with low ACTH suggests pituitary or hypothalamic problems.
Imaging Studies
When hormone tests indicate adrenal or pituitary disorders, imaging helps locate structural abnormalities:
- MRI scans of the pituitary gland reveal tumors or abnormalities
- CT scans of the adrenal glands identify tumors, hyperplasia, or atrophy
- Specialized nuclear medicine scans sometimes trace hormone production sources
These studies complement hormone testing, creating a complete diagnostic picture.
Accessing Cortisol Testing Through Direct-to-Consumer Services
Traditional cortisol testing typically requires doctor referrals, insurance approvals, and multiple appointments. Modern direct-access laboratory services have transformed this process.
Platforms offering convenient lab testing allow you to order tests independently, often at transparent, affordable prices. This approach benefits people who:
- Lack health insurance or have high-deductible plans
- Want to monitor hormone levels proactively
- Experience symptoms but face long wait times for specialist appointments
- Prefer privacy and direct access to their health data
The Self-Pay Testing Process
Direct-access testing follows a streamlined workflow:
- Select your desired test from available options
- Complete your order and receive lab requisition
- Visit a nearby collection facility at your convenience
- Receive results electronically within 1-3 days
- Review findings and consult with healthcare providers as needed
This model eliminates many barriers while maintaining quality standards. Accredited laboratories perform the same tests using identical equipment and methodologies as traditional medical settings.
When to Consult Healthcare Professionals
While direct testing provides valuable information, certain situations require professional medical guidance. Abnormal results, particularly significantly elevated or low cortisol levels, warrant consultation with endocrinologists or primary care providers.
Healthcare professionals provide essential services including:
- Comprehensive interpretation within your full medical context
- Ordering specialized follow-up tests
- Diagnosing specific conditions
- Prescribing necessary treatments
- Monitoring therapy effectiveness
Direct-access testing complements rather than replaces medical care. Think of it as gathering important data that empowers informed conversations with your healthcare team.
Managing Cortisol Levels
Test results revealing imbalanced cortisol levels open pathways to targeted interventions. Treatment approaches depend on whether levels run too high or too low, and the underlying cause.
Addressing High Cortisol
Treatment for elevated cortisol targets the root cause. Cushing's syndrome from tumors often requires surgical removal of pituitary or adrenal tumors. Radiation therapy or medications that block cortisol production provide alternatives when surgery isn't feasible.
For stress-related elevation without underlying disease, lifestyle modifications prove effective:
- Stress management techniques including meditation, deep breathing, and mindfulness
- Regular moderate exercise rather than intense workouts that may temporarily spike cortisol
- Adequate sleep of 7-9 hours nightly
- Balanced nutrition emphasizing whole foods and limiting caffeine
- Social support and professional counseling when dealing with chronic stress
Treating Low Cortisol
Adrenal insufficiency requires hormone replacement therapy. Hydrocortisone or prednisone tablets replace missing cortisol, typically taken in divided doses that mimic natural production patterns.
Patients with primary adrenal insufficiency also need mineralocorticoid replacement (fludrocortisone) to maintain proper sodium and potassium balance. Dosing requires careful adjustment based on symptoms, blood pressure, and electrolyte levels.
Essential aspects of replacement therapy:
- Taking medications exactly as prescribed, never skipping doses
- Increasing doses during illness, injury, or major stress
- Wearing medical identification indicating adrenal insufficiency
- Carrying emergency hydrocortisone injection for crisis situations
- Regular monitoring through follow-up testing
Special Considerations for Different Populations
Cortisol testing interpretation varies across different groups. Understanding these nuances ensures accurate assessment.
Athletes and Active Individuals
Regular intense exercise temporarily elevates cortisol as part of the normal stress response. Athletes may show higher baseline levels without pathology. Timing tests during rest periods and avoiding testing shortly after competitions provides clearer pictures of true adrenal function.
Overtraining syndrome can chronically dysregulate cortisol patterns. Athletes experiencing persistent fatigue, declining performance, or frequent illness benefit from cortisol assessment to rule out hormonal contributions.
Recommended Panel
Energy & Fatigue Panel
Save $4.5Fatigue has many causes - this panel tests for the most common ones: thyroid dysfunction, iron deficiency, vitamin deficiencies, anemia, and metabolic issues. Stop guessing, start knowing.
Includes 36 biomarkers
$72
Fasting required
Pregnancy and Postpartum
Cortisol levels naturally increase during pregnancy, sometimes reaching two to three times normal levels. Standard reference ranges don't apply to pregnant individuals. Specialized interpretation accounts for trimester-specific changes.
Postpartum, levels gradually normalize over several weeks. Persistent elevation or very low levels after delivery warrant investigation, as they may indicate complications or pre-existing conditions masked by pregnancy.
Children and Adolescents
Pediatric cortisol testing uses age-specific reference ranges. Children's adrenal glands develop over time, and normal values differ significantly from adults. Growth patterns, puberty, and developmental stage all influence results.
Symptoms prompting pediatric testing include poor growth, excessive weight gain, early or delayed puberty, and unusual fatigue or weakness. Specialized pediatric endocrinologists interpret results and guide treatment when necessary.
Cost Considerations and Insurance Coverage
Understanding the financial aspects of cortisol testing helps you plan effectively. Traditional medical testing through insurance involves copays, deductibles, and potential balance billing. Costs vary tremendously based on your specific insurance plan.
Self-pay pricing through direct-access services often surprises people with its affordability and transparency. Without insurance markup and administrative overhead, tests frequently cost less than insurance deductibles. You know exact prices upfront, avoiding surprise bills.
For those seeking both English language services and Spanish language support, modern testing platforms accommodate diverse communities. Transparent pricing and multilingual resources make hormone testing accessible regardless of insurance status or language preference.
Maximizing Testing Value
Strategic testing approaches optimize your investment:
- Start with basic cortisol measurement rather than comprehensive panels unless symptoms suggest complex disorders
- Time tests appropriately to capture peak and trough levels with minimal samples
- Keep detailed symptom logs to correlate with test results
- Share results with healthcare providers to avoid redundant testing
- Consider periodic monitoring if treating hormone imbalances to track progress
Questions about specific tests, pricing, or processes find answers through resources like frequently asked questions provided by testing services.
Cortisol testing provides critical insights into your body's stress response and adrenal health, helping identify conditions ranging from chronic stress to serious hormone disorders. Understanding when to test, how different methods work, and what results mean empowers you to take charge of your hormone health. If you're experiencing unexplained fatigue, weight changes, or other symptoms that suggest cortisol imbalance, Justlabs offers convenient, affordable testing with results in 1-3 days, eliminating the need for insurance approvals or extended doctor appointment waits.