When digestive symptoms persist and gluten seems to be the culprit, many people wonder if they can access screening tests without navigating the traditional healthcare system. A celiac disease blood test offers a first step in identifying this autoimmune condition, and understanding how these tests work empowers you to make informed decisions about your health. The landscape of lab testing has evolved significantly, with options now available for those seeking direct access to diagnostic tools without insurance requirements or mandatory physician referrals.
Understanding Celiac Disease Blood Testing
Celiac disease affects approximately 1% of the population, yet many cases remain undiagnosed for years. Blood tests serve as the primary screening tool because they detect specific antibodies that the immune system produces when someone with celiac disease consumes gluten. These antibodies indicate an autoimmune response rather than a simple food sensitivity or intolerance.
The diagnostic process for celiac disease typically begins with serological testing before moving to more invasive procedures. Blood screening offers a non-invasive, cost-effective way to determine whether further testing is warranted. For those exploring labs without insurance, understanding which tests provide the most reliable information becomes particularly important.
Primary Antibody Tests for Celiac Disease
Several antibody tests are used to screen for celiac disease, each measuring different immune responses:
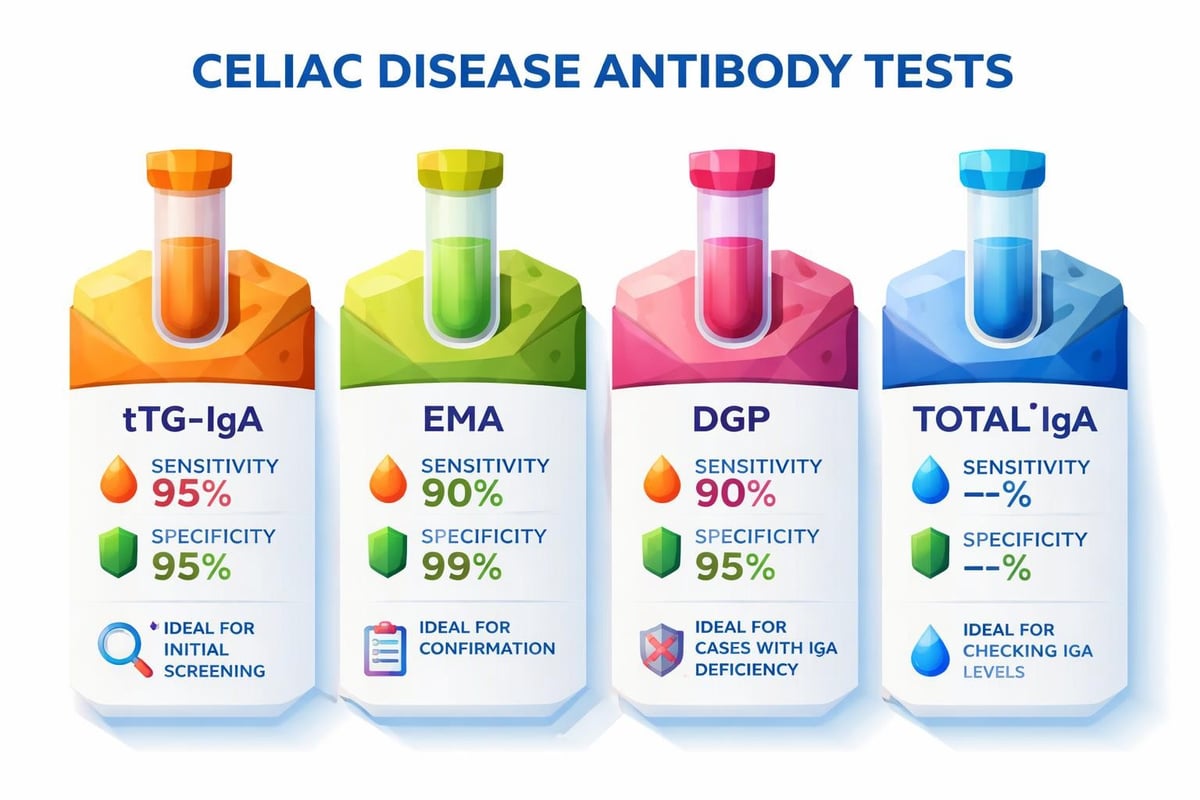
- Tissue Transglutaminase IgA (tTG-IgA): The most commonly ordered test and generally the most sensitive for detecting celiac disease
- Endomysial Antibody IgA (EMA): Highly specific test often used to confirm positive tTG-IgA results
- Deamidated Gliadin Peptide (DGP) IgA and IgG: Useful for patients under age 2 or those with IgA deficiency
- Total Serum IgA: Measures overall IgA levels to ensure accurate interpretation of IgA-based tests
The tTG-IgA test represents the gold standard for initial screening. According to the Celiac Disease Foundation's screening guidelines, this test demonstrates sensitivity rates exceeding 95% when patients are actively consuming gluten. However, a complete panel often includes multiple antibody tests to maximize accuracy and account for individual variations.
Recommended Test
Celiac Disease Panel
This comprehensive panel screens for celiac disease using multiple antibody markers, providing thorough coverage for both standard and IgA-deficient patients.
Includes 5 biomarkers
$85
The Critical Role of Gluten Consumption
One of the most important factors affecting celiac disease blood test accuracy is gluten consumption before testing. The antibodies these tests detect only appear in the bloodstream when the immune system actively responds to gluten proteins. If you've already eliminated gluten from your diet, test results may return false negatives even if you have celiac disease.
Healthcare providers typically recommend consuming gluten-containing foods daily for at least several weeks before testing. The National Celiac Association emphasizes that patients should maintain their normal gluten-containing diet throughout the testing process. This requirement presents a significant challenge for individuals who have already noticed symptom improvement after reducing gluten intake.
Recent developments offer hope for those struggling with gluten consumption requirements. Research highlighted by the American Society for Clinical Pathology discusses emerging blood tests that may diagnose celiac disease without requiring patients to eat gluten. While these newer testing methods show promise, traditional antibody tests remain the current standard for initial screening.
Preparing for Your Blood Test
Proper preparation ensures the most accurate results:
- Continue eating gluten: Consume gluten equivalent to 1-2 slices of bread daily for at least 2-4 weeks before testing
- Schedule appropriately: Most tests don't require fasting, but confirm requirements with your testing facility
- Document symptoms: Keep a diary of digestive symptoms, their frequency, and their relationship to gluten consumption
- Review medications: Inform the lab of any immunosuppressant medications that might affect antibody production
- Consider timing: Schedule the blood draw when you've been consistently consuming gluten
Interpreting Your Test Results
Understanding what your celiac disease blood test results mean requires knowing how laboratories report findings. Most results appear as numerical values with reference ranges, indicating whether antibody levels fall within normal limits or suggest potential celiac disease.
| Test Type | Normal Range | Positive Indicator | Next Steps |
|---|---|---|---|
| tTG-IgA | <4 U/mL | ≥4 U/mL | Consult gastroenterologist |
| EMA | Negative | Positive | Consider endoscopy |
| DGP IgA/IgG | <20 U/mL | ≥20 U/mL | Additional testing needed |
| Total IgA | 70-400 mg/dL | <70 mg/dL | Use IgG-based tests |
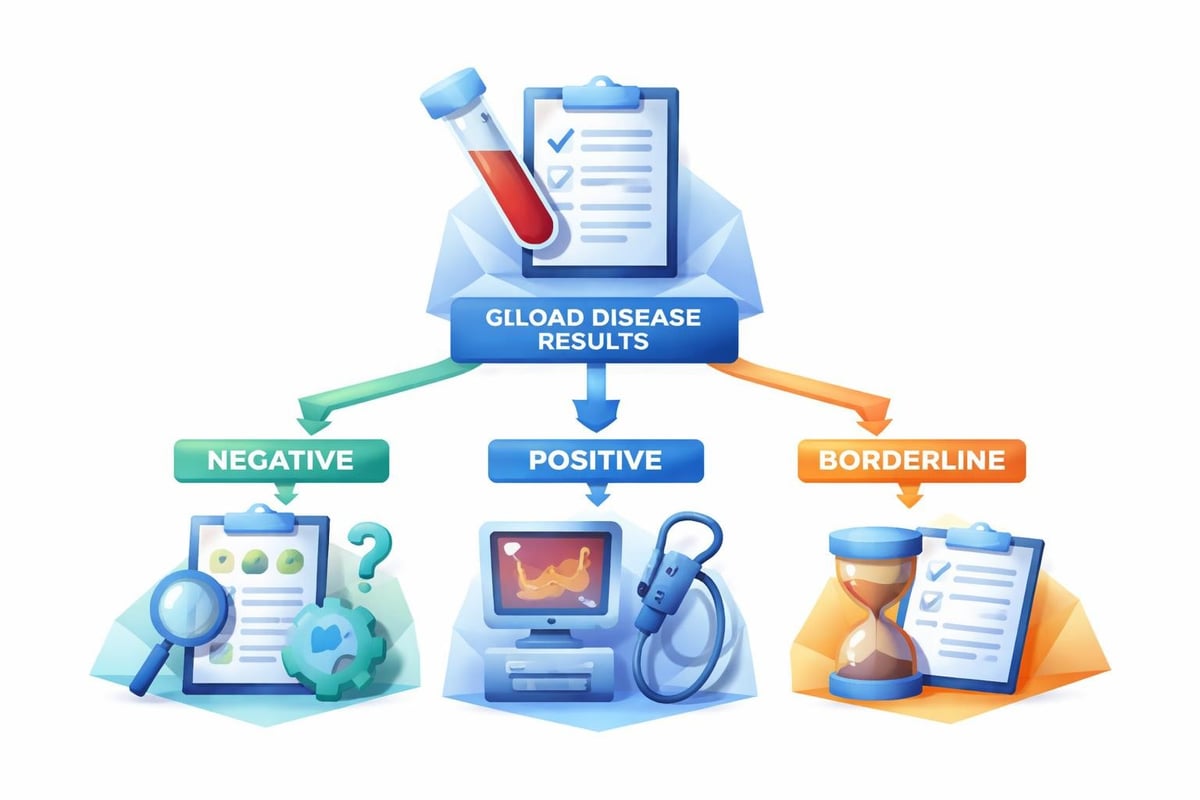
Positive results indicate elevated antibody levels consistent with celiac disease. However, a positive celiac disease blood test doesn't provide a definitive diagnosis on its own. Most gastroenterologists recommend endoscopic biopsy to confirm intestinal damage before starting a lifelong gluten-free diet.
Negative results suggest celiac disease is unlikely, particularly when multiple antibody tests return normal values. However, false negatives can occur with IgA deficiency, minimal gluten consumption, or early-stage disease. If symptoms persist despite negative results, discuss additional testing options with a healthcare provider.
Borderline results fall in a gray area where values are elevated but don't clearly indicate celiac disease. These situations often require repeat testing after a few months or additional diagnostic procedures.
Accessing Tests Without Traditional Doctor Visits
The traditional model for obtaining a celiac disease blood test involves scheduling a doctor's appointment, discussing symptoms, receiving a test order, visiting a lab, and then following up for results. This process can take weeks and involves multiple appointments, copays, and insurance authorizations. For many people, these barriers delay necessary screening.
Self-pay lab testing services have transformed access to diagnostic tools. When you order labs without a doctor, you can initiate screening based on your own health concerns and timeline. This approach offers several advantages for celiac disease testing:
- Immediate access: Order tests online without waiting for appointments
- Transparent pricing: Know exact costs upfront without insurance billing surprises
- Convenience: Choose from thousands of lab locations nationwide
- Quick results: Receive findings within 1-3 days in most cases
- Privacy: Maintain control over your health information
However, self-directed testing also carries responsibilities. Understanding which tests to order, how to interpret results, and when to seek medical consultation becomes your responsibility. The comprehensive FAQ resources provided by testing services can help you make informed decisions about your screening journey.
Who Should Consider Celiac Disease Screening
Not everyone needs a celiac disease blood test, but certain symptoms and risk factors warrant consideration. The condition manifests differently across individuals, making it challenging to identify without testing.
Common Symptoms Suggesting Testing
Digestive symptoms represent the most recognized indicators:
- Chronic diarrhea or constipation
- Abdominal bloating and pain
- Gas and cramping after eating
- Unexplained weight loss
- Fatty, pale, or foul-smelling stools
Non-digestive symptoms often surprise people but can signal celiac disease:
- Skin issues: Itchy, blistery rash (dermatitis herpetiformis)
- Neurological problems: Headaches, numbness, balance issues
- Fatigue: Persistent tiredness unrelieved by rest
- Bone or joint pain: Unexplained osteoporosis or arthritis
- Mood changes: Depression, anxiety, or brain fog
High-Risk Groups
Certain populations face elevated celiac disease risk and may benefit from screening even without obvious symptoms:
| Risk Factor | Increased Risk Level | Screening Recommendation |
|---|---|---|
| First-degree relative with celiac disease | 10-20% | Test regardless of symptoms |
| Type 1 diabetes | 5-10% | Regular screening advised |
| Autoimmune thyroid disease | 2-5% | Consider testing with symptoms |
| Down syndrome | 5-12% | Periodic screening recommended |
| Turner syndrome | 4-8% | Regular monitoring suggested |
Medical guidelines from UCLA Health's celiac resources suggest that individuals with autoimmune conditions or family history should discuss screening with healthcare providers. However, you don't need to wait for a referral to begin the testing process.
Cost Considerations and Insurance Alternatives
Traditional insurance-based testing can result in unexpected bills due to deductibles, copays, and out-of-network charges. Many people assume insurance always reduces costs, but this isn't necessarily true for basic screening tests. Insurance claims generate administrative overhead that self-pay models eliminate entirely.
When you explore how self-pay lab testing works, pricing transparency becomes immediately apparent. You see the exact cost before ordering, and that price includes the blood draw, laboratory analysis, and results delivery. No surprise bills arrive months later.
Self-pay celiac disease blood test panels typically range from $70 to $200 depending on which antibodies are included. A comprehensive panel testing multiple antibodies costs less than many insurance copays for specialist visits. For uninsured individuals or those with high-deductible plans, self-pay testing often represents the most economical option.
Beyond the Initial Blood Test
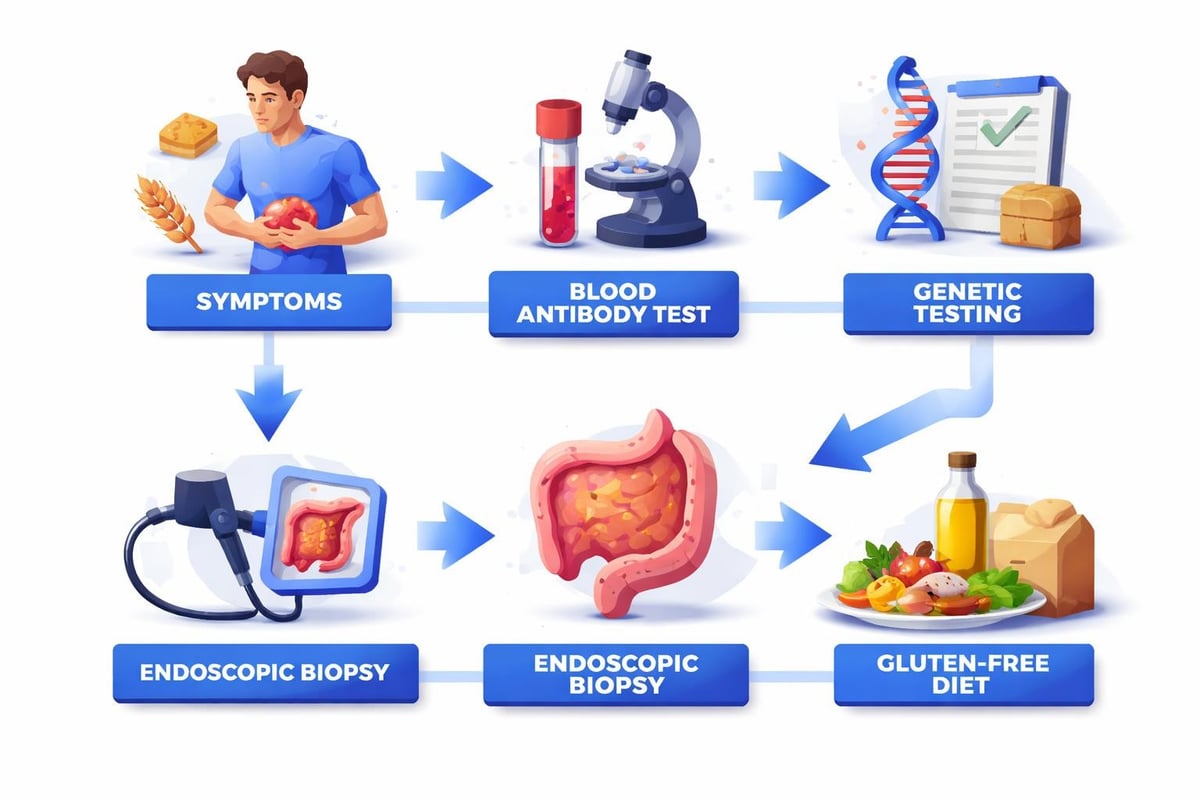
A celiac disease blood test serves as a screening tool, not a final diagnosis. Understanding the complete diagnostic pathway helps you anticipate next steps based on your results. Positive antibody tests typically lead to endoscopy with small intestine biopsies, which remain the gold standard for confirming celiac disease.
The endoscopic procedure allows gastroenterologists to visually examine the small intestine and collect tissue samples. Under a microscope, these samples reveal characteristic damage patterns: flattened villi, increased inflammatory cells, and other structural changes caused by immune responses to gluten.
Genetic Testing for HLA-DQ2 and HLA-DQ8
Genetic testing offers additional information, though it works differently than antibody screening. Approximately 95% of people with celiac disease carry either the HLA-DQ2 or HLA-DQ8 gene variant. However, about 30-40% of the general population carries these genes without developing celiac disease.
Genetic testing proves most useful for ruling out celiac disease rather than confirming it. A negative genetic test effectively eliminates celiac disease as a diagnosis, since the condition rarely occurs without these gene variants. This makes genetic testing valuable when antibody results are unclear or when someone has already started a gluten-free diet before testing.
Common Testing Mistakes to Avoid
Several missteps can compromise celiac disease blood test accuracy or create unnecessary complications:
Starting a gluten-free diet before testing represents the most common error. Many people experiment with gluten elimination when they suspect sensitivity. While this may improve symptoms temporarily, it interferes with antibody production and leads to false-negative results. If you've already removed gluten, discuss gluten challenge protocols with a healthcare provider before testing.
Ordering incomplete panels sometimes occurs when people try to minimize costs by selecting only one antibody test. While the tTG-IgA test is highly sensitive, combining it with total IgA measurement and potentially other antibodies increases diagnostic accuracy. IgA deficiency affects 2-3% of people with celiac disease, making IgG-based tests necessary for these individuals.
Ignoring positive results poses serious health risks. Some people receive positive screening results but delay follow-up because they feel relatively well. Untreated celiac disease causes long-term complications including nutrient deficiencies, osteoporosis, infertility, and increased cancer risk. Positive antibody tests warrant prompt gastroenterology consultation regardless of symptom severity.
Self-diagnosing based on negative results can miss other important conditions. Negative celiac antibody tests don't exclude non-celiac gluten sensitivity, wheat allergy, inflammatory bowel disease, or other digestive disorders. Persistent symptoms after negative screening deserve medical evaluation to identify the underlying cause.
The Self-Testing Empowerment Movement
Healthcare is shifting toward patient empowerment and direct access to diagnostic information. The ability to order a celiac disease blood test without navigating insurance bureaucracy or scheduling multiple appointments represents this broader trend. You become an active participant in your health journey rather than a passive recipient of care.
This empowerment comes with responsibility for understanding test limitations, recognizing when professional medical guidance is essential, and making informed decisions about follow-up care. Self-pay testing services don't replace comprehensive medical care; they complement it by removing barriers to initial screening.
Consider the wide range of available tests that address various health concerns beyond celiac disease. Having convenient, affordable access to laboratory testing enables proactive health management and early detection of conditions that benefit from prompt intervention.
When Medical Consultation Becomes Essential
While you can initiate celiac disease screening independently, certain situations require physician involvement:
- Positive antibody test results need gastroenterology consultation for endoscopic confirmation
- Children under 18 should have medical supervision throughout the diagnostic process
- Pregnant women require specialized guidance about testing and dietary management
- Individuals with multiple autoimmune conditions need coordinated care
- Anyone experiencing severe symptoms like significant weight loss or malnutrition needs immediate medical attention
Think of self-directed blood testing as an entry point to the healthcare system rather than a complete substitute for medical care. You gain the advantage of starting the diagnostic process on your terms while maintaining the flexibility to engage physicians when their expertise becomes necessary.
The research on patient self-testing management emphasizes the importance of professional medical evaluation following home or self-directed testing. Positive results require confirmation and treatment planning, while persistent symptoms despite negative results warrant investigation for alternative diagnoses.
Testing in Special Populations
Celiac disease blood test interpretation varies across different age groups and health situations. Young children under age 2 may show different antibody patterns, making DGP tests more reliable than standard tTG-IgA screening. Pediatric testing requires careful consideration of age-appropriate reference ranges and test selections.
Elderly adults sometimes present with subtle or atypical symptoms, leading to underdiagnosis in this population. Testing remains accurate in older individuals, though they may have other health conditions complicating interpretation. Comprehensive panels that measure multiple antibodies help clarify results when single tests yield borderline findings.
People taking immunosuppressant medications for other autoimmune conditions may produce lower antibody levels even with active celiac disease. These situations require discussion with healthcare providers about medication timing relative to testing or consideration of endoscopic evaluation without elevated antibody markers.
Emerging Testing Technologies
The landscape of celiac disease diagnosis continues evolving with new technologies addressing current limitations. Point-of-care tests that provide results in minutes rather than days are entering the market, though they generally serve as preliminary screening tools requiring confirmatory laboratory testing.
Saliva-based testing represents another area of development, offering even less invasive sample collection than blood draws. While research shows promise, these methods haven't yet achieved the sensitivity and specificity of standard blood antibody testing for widespread clinical use.
The development of tests that don't require gluten consumption marks a significant advancement for patients who have already adopted gluten-free diets. These emerging methods measure different biomarkers that remain detectable regardless of current gluten intake. As these technologies mature and gain regulatory approval, they may transform the diagnostic landscape.
Taking Control of Your Digestive Health
Suspecting celiac disease creates anxiety and uncertainty, but taking proactive steps toward answers provides relief. A celiac disease blood test offers an accessible starting point for investigating whether your symptoms stem from this autoimmune condition or other digestive issues. The ability to initiate screening without insurance delays or mandatory physician appointments removes traditional barriers that postponed diagnosis for countless individuals.
Understanding test options, preparation requirements, and result interpretation equips you to make informed decisions about your health journey. Whether results indicate celiac disease requiring further investigation or rule out this condition and prompt exploration of alternative diagnoses, testing provides valuable information guiding your next steps.
Identifying celiac disease early prevents long-term complications and improves quality of life through appropriate dietary management. When you're ready to take the first step toward answers, Justlabs provides direct access to comprehensive celiac disease screening with transparent pricing, convenient locations nationwide, and results delivered within days. No insurance hassles, no doctor's appointment required-just straightforward testing that puts you in control of your health decisions.