Managing lupus effectively requires consistent monitoring between rheumatology appointments. While your initial diagnosis may have involved comprehensive testing, ongoing lupus blood tests serve a different purpose: tracking disease activity, catching flare-ups early, and ensuring your treatment plan remains effective. Understanding what your rheumatologist checks and why these tests matter empowers you to take an active role in your care and make informed decisions about when to seek additional testing or medical attention.
Understanding the Role of Routine Lupus Blood Tests
Regular blood work provides your rheumatologist with objective data about your body's inflammatory response and organ function. Unlike symptoms that can be subjective or vary day to day, laboratory values offer measurable insights into what's happening at a cellular level. This information helps your doctor distinguish between normal fluctuations and genuine disease progression.
Between scheduled appointments, your lupus may change significantly. New autoantibodies can develop, inflammation levels may rise, or medications might affect your blood counts. The Lupus Foundation of America outlines common laboratory tests that help track these changes before they become symptomatic.
Why Monitoring Frequency Matters
The timing of your blood tests depends on several factors:
- Current disease activity level
- Medications you're taking (especially immunosuppressants)
- Recent changes to your treatment plan
- Pregnancy or plans to become pregnant
- New or worsening symptoms
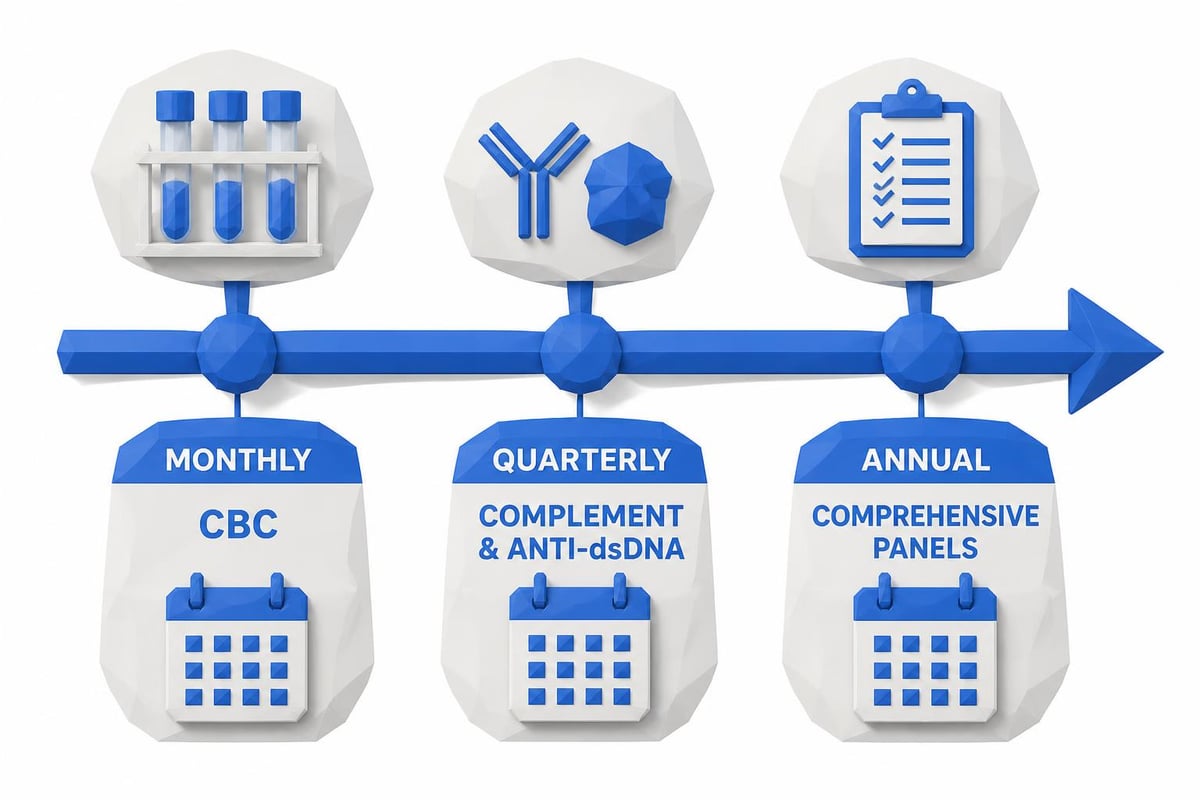
Most rheumatologists recommend testing every three to six months for stable patients. Those experiencing active disease or medication adjustments may need monthly monitoring.
Essential Lupus Blood Tests Your Doctor Orders
Your rheumatologist relies on a panel of specific tests to create a complete picture of your lupus activity. Each test provides unique information about different aspects of the disease.
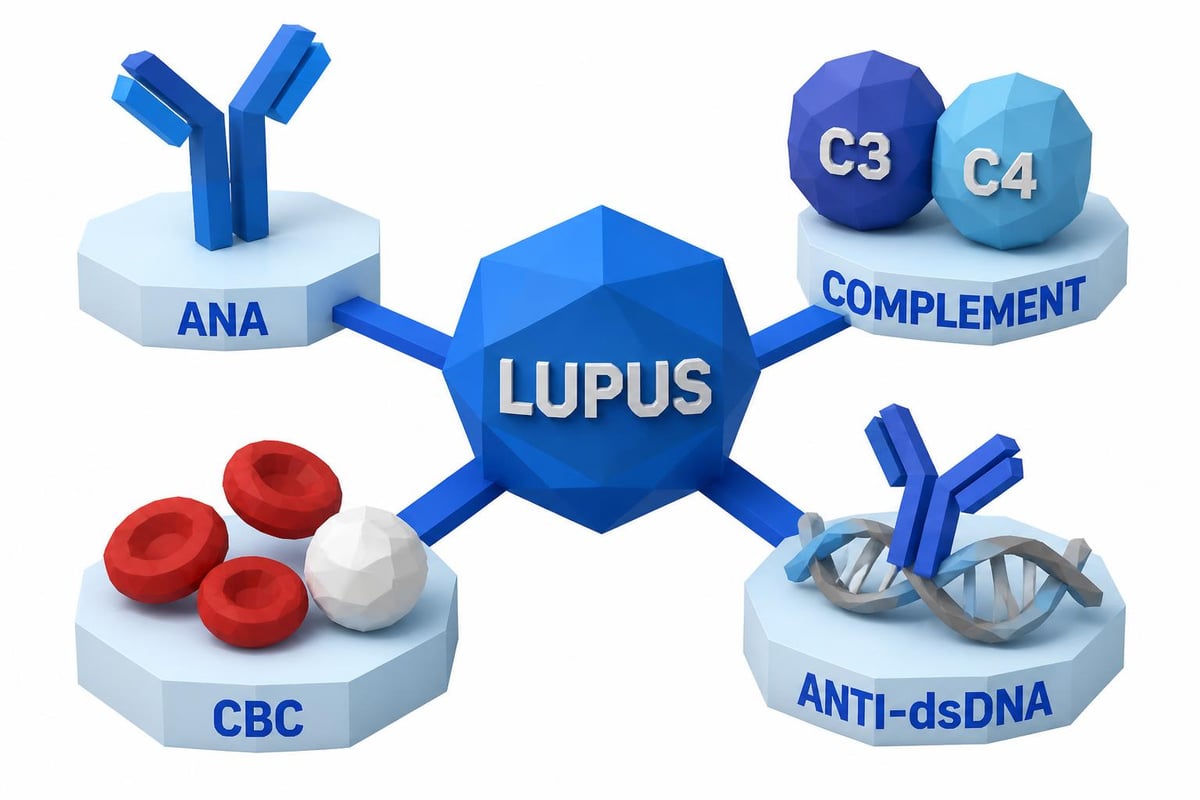
Antinuclear Antibody (ANA) Test
The ANA test remains foundational in lupus monitoring, though its role differs from diagnosis. While Johns Hopkins Lupus Center explains the role of specific blood tests in initial diagnosis, ongoing ANA monitoring helps track antibody levels over time. A rising ANA titer sometimes precedes clinical flare-ups, though this pattern varies significantly among patients.
Your ANA pattern also matters. Homogeneous and peripheral patterns associate more strongly with lupus, while speckled patterns may indicate other autoimmune conditions developing concurrently.
Complete Blood Count (CBC)
The CBC measures three critical components:
Red blood cells: Lupus can cause anemia through multiple mechanisms, including chronic inflammation, kidney disease, or medication side effects. Tracking hemoglobin and hematocrit helps identify when anemia develops.
White blood cells: Leukopenia (low white blood cell count) occurs in approximately 50% of lupus patients. Lymphopenia specifically correlates with disease activity and may signal an impending flare.
Platelets: Thrombocytopenia (low platelet count) can result from lupus itself or antiphospholipid antibodies. This condition increases bleeding risk and requires close monitoring.
Complement Levels (C3 and C4)
Complement proteins play a crucial role in your immune system. During active lupus, your body consumes these proteins faster than it produces them, causing levels to drop. Low C3 and C4 levels often indicate:
- Active systemic inflammation
- Potential kidney involvement
- Increased risk of flare-up
| Complement Test | Normal Range | Low Level Significance |
|---|---|---|
| C3 | 90-180 mg/dL | Active disease, possible kidney involvement |
| C4 | 10-40 mg/dL | Immune complex formation, inflammation |
| CH50 | 30-75 U/mL | Overall complement system function |
Rising complement levels during treatment suggest your therapy is working effectively.
Advanced Antibody Testing for Disease Monitoring
Beyond basic panels, specific antibody tests provide detailed information about lupus activity and organ involvement.
Anti-Double Stranded DNA (Anti-dsDNA)
This highly specific lupus marker strongly correlates with kidney disease. Medical News Today details the types of blood tests doctors order for lupus diagnosis, but anti-dsDNA proves particularly valuable for ongoing monitoring. Rising levels often precede lupus nephritis by weeks or months, allowing preventive intervention.
Approximately 70% of lupus patients test positive for anti-dsDNA at some point. Regular testing helps identify when kidney-protective treatments should begin.
Anti-Smith (Anti-Sm) Antibodies
While anti-Sm antibodies rarely change once positive, they're highly specific to lupus. Finding these antibodies confirms your diagnosis definitively and can guide treatment decisions. Unlike anti-dsDNA, anti-Sm levels don't typically fluctuate with disease activity.
Antiphospholipid Antibodies
These antibodies increase blood clotting risk and require separate monitoring:
- Lupus anticoagulant
- Anticardiolipin antibodies (IgG and IgM)
- Anti-beta-2 glycoprotein I antibodies
Testing occurs periodically because these antibodies can develop years after initial diagnosis. Their presence may necessitate anticoagulation therapy to prevent dangerous blood clots.
Inflammatory Markers and Disease Activity
General inflammation indicators supplement lupus-specific tests, providing context for your overall disease state.
Erythrocyte Sedimentation Rate (ESR)
The Arthritis Foundation provides information on tests including ESR for assessing inflammation. This test measures how quickly red blood cells settle in a tube over one hour. Faster settling indicates higher inflammation levels.
ESR elevations may signal:
- Active lupus flare
- Infection requiring treatment
- Other inflammatory conditions
- Medication effectiveness
However, ESR lacks specificity. Many conditions raise ESR, requiring your doctor to interpret results alongside other findings.
C-Reactive Protein (CRP)
CRP rises rapidly during inflammation and returns to normal quickly once inflammation resolves. Interestingly, lupus often causes only modest CRP elevations compared to other inflammatory diseases. Significantly elevated CRP in a lupus patient often suggests infection rather than lupus activity itself.
This distinction proves clinically valuable when you develop new symptoms. High CRP with stable lupus markers points toward infection, while normal CRP with changing lupus-specific tests suggests a flare.
Organ Function Tests Critical for Lupus Monitoring
Lupus can affect virtually any organ system. Regular monitoring helps detect problems before permanent damage occurs.
Kidney Function Tests
Lupus nephritis develops in approximately 40% of patients and represents a major cause of morbidity. Early detection through blood work allows aggressive treatment that can preserve kidney function.
| Test | Purpose | Frequency |
|---|---|---|
| Creatinine | Measures kidney filtration | Every 3-6 months |
| Blood Urea Nitrogen (BUN) | Assesses waste removal | Every 3-6 months |
| Estimated GFR | Calculates overall kidney function | Every 3-6 months |
| Urinalysis | Detects protein and blood in urine | Every 3-6 months |
Rising creatinine or declining GFR indicates deteriorating kidney function requiring immediate intervention. Many patients also need periodic urine protein measurements to quantify kidney damage.
Liver Function Tests
Immunosuppressive medications commonly used in lupus can stress the liver. Regular monitoring of liver enzymes (ALT, AST, alkaline phosphatase) ensures these medications remain safe. Additionally, autoimmune hepatitis occasionally develops in lupus patients, requiring separate treatment.
Metabolic Panel
A comprehensive metabolic panel evaluates:
- Electrolyte balance (sodium, potassium, chloride)
- Blood glucose levels
- Calcium and mineral status
- Protein and albumin levels
Lupus and its treatments can affect all these values. Corticosteroids, for instance, commonly raise blood glucose, potentially causing diabetes with long-term use.
Accessing Lupus Blood Tests Between Appointments
Traditional healthcare scheduling can delay important testing when you notice concerning symptoms. Waiting weeks for an appointment, then additional days for results, potentially allows disease progression.

Modern lab testing services address this gap. If you're experiencing new fatigue, joint pain, or other symptoms between scheduled visits, you can order lab tests without a doctor appointment. This approach provides several advantages:
Faster results: Most comprehensive panels return within one to three business days, allowing you to share current data with your rheumatologist promptly.
Cost transparency: Lab testing without insurance through self-pay services often costs less than insurance copays and deductibles, with prices clearly stated upfront.
Convenience: Understanding how the testing process works helps you complete testing at nearby facilities without scheduling delays.
Self-directed testing doesn't replace your rheumatologist's expertise. Instead, it empowers you to gather timely information when symptoms change, supporting better-informed conversations with your doctor.
Interpreting Your Lupus Blood Test Results
Understanding your results requires context. Numbers outside reference ranges don't automatically indicate problems, and normal results don't always mean your lupus is inactive.
Individual Baseline Matters
Every patient establishes their own baseline values. Your "normal" ANA titer might be 1:320, while another patient's baseline sits at 1:80. What matters most is tracking changes from your personal baseline rather than fixating on reference ranges.
Keep copies of all blood work to identify trends over time. A complement level dropping from your baseline of 110 mg/dL to 85 mg/dL might signal increasing activity, even though 85 remains within the technical normal range.
Multiple Tests Tell the Story
No single test result defines your lupus status. Your rheumatologist considers the complete picture:
- Are inflammatory markers rising together?
- Do antibody levels correlate with symptoms?
- Has kidney function changed?
- Do trends suggest improvement or worsening?
This comprehensive approach prevents overreacting to isolated abnormal values while catching genuine problems early.
When to Contact Your Doctor
Certain findings warrant immediate communication with your rheumatologist:
- Significantly elevated creatinine or declining kidney function
- New thrombocytopenia or severe anemia
- Dramatically rising anti-dsDNA levels
- Persistent fever with normal or low white blood cell count
- Abnormal liver enzymes, especially if taking immunosuppressants
Healthline discusses the process of diagnosing lupus, but monitoring differs from diagnosis. Your established relationship with your rheumatologist allows nuanced interpretation of changing values.
Medication Monitoring Through Blood Work
Lupus treatments require their own specific monitoring protocols beyond tracking disease activity itself.
Immunosuppressant Monitoring
Common lupus medications need regular surveillance:
Methotrexate: Requires monthly CBC and liver function tests initially, then every three months once stable. This medication can suppress bone marrow and affect liver health.
Azathioprine: Needs regular CBC monitoring for cytopenias and liver function assessment. Some doctors also check thiopurine methyltransferase (TPMT) enzyme levels before starting treatment.
Mycophenolate: Requires CBC monitoring, particularly for white blood cells and platelets. Gastrointestinal side effects are common but don't require specific blood monitoring.
Cyclophosphamide: Demands close monitoring of blood counts due to significant bone marrow suppression risk.
Biologic Therapy Monitoring
Newer biologic medications like belimumab still require baseline and periodic blood work, though monitoring intensity varies. Your doctor tracks infection markers, kidney function, and general blood counts to ensure these therapies remain safe.
Hydroxychloroquine Considerations
While hydroxychloroquine (Plaquenil) doesn't require routine blood monitoring, baseline testing helps establish your status before starting. Some doctors periodically check G6PD enzyme levels, as deficiency can cause hemolysis with this medication.
Cost Considerations for Ongoing Lupus Blood Tests
Lupus monitoring requires lifelong testing, making costs a practical concern for many patients. Understanding your options helps maintain consistent monitoring without financial strain.
Insurance coverage varies dramatically. Some plans require substantial copays for each test, while others impose deductibles before coverage begins. Transparent lab test pricing through self-pay services sometimes provides better value than insurance-based testing.
Additionally, many monitoring tests qualify as FSA or HSA eligible, allowing you to use pre-tax dollars for testing expenses. This option can reduce effective costs by 20-30% depending on your tax bracket.
Planning Your Testing Budget
Creating an annual testing budget helps maintain consistent monitoring:
- Calculate expected testing frequency based on your current disease state
- Price your typical panel through both insurance and self-pay options
- Factor in convenience costs like copays, time off work, or travel
- Set aside monthly amounts in an HSA or FSA if available
- Discuss financial constraints with your rheumatologist to prioritize essential tests
Consistent monitoring proves more valuable than comprehensive testing done sporadically due to cost concerns.
The Future of Lupus Blood Testing
Research continues advancing lupus monitoring capabilities. Innovative approaches to discovering lupus heterogeneity from electronic health records may soon enable more personalized testing protocols based on your specific lupus subtype.
Additionally, natural language processing to identify lupus nephritis patterns shows promise for earlier kidney disease detection. These technologies may eventually allow doctors to predict flares weeks in advance, enabling preventive treatment adjustments.
Point-of-care testing development might eventually allow some lupus monitoring from home, similar to diabetes glucose monitoring. While not yet available, these advances could revolutionize how patients track disease activity between formal laboratory testing.
Building Your Testing Schedule
Work with your rheumatologist to establish a monitoring schedule appropriate for your situation. A typical stable patient might follow this pattern:
Every 3-6 months:
- Complete blood count
- Comprehensive metabolic panel
- Complement levels (C3, C4)
- Urinalysis
- Anti-dsDNA antibodies
Every 6-12 months:
- Complete antibody panel
- Antiphospholipid antibodies
- Inflammatory markers (ESR, CRP)
- Vitamin D levels
- Thyroid function
As needed:
- Medication-specific monitoring
- Testing prompted by new symptoms
- Pre-conception or pregnancy monitoring
- Infection workups
This schedule adjusts based on symptoms, treatment changes, or concerning trends in your results. Finding convenient locations for testing helps maintain adherence to your monitoring plan.
Regular lupus blood tests provide essential insights into disease activity, medication safety, and organ function between rheumatology appointments. Understanding what your doctor monitors and why these tests matter enables you to participate actively in your care and recognize when additional testing might be needed. Whether you need routine monitoring panels or want to investigate new symptoms promptly, Justlabs offers convenient access to comprehensive testing with transparent pricing and results delivered within days, helping you stay informed about your lupus without insurance delays or scheduling barriers.