When your thyroid-stimulating hormone (TSH) levels drop below the normal range, it raises important questions about your thyroid health. A low TSH reading on a lab test often leaves patients wondering whether they're dealing with an overactive thyroid gland, taking too much thyroid medication, or facing another underlying condition. Understanding what drives TSH levels down and how to interpret these results is essential for managing your thyroid health effectively and making informed decisions about testing and treatment.
Understanding TSH and Its Role in Thyroid Function
Thyroid-stimulating hormone serves as the primary messenger between your pituitary gland and your thyroid gland. The pituitary produces TSH to signal your thyroid to release thyroid hormones, specifically triiodothyronine (T3) and thyroxine (T4). This communication system operates on a negative feedback loop: when thyroid hormone levels rise, TSH production decreases, and when thyroid hormones drop, TSH increases.
The Normal TSH Range
The typical reference range for TSH falls between 0.4 and 4.0 mIU/L, though some laboratories use slightly different parameters. When your TSH drops below 0.4 mIU/L, medical professionals consider it suppressed or low. However, the severity of low TSH matters significantly for diagnosis and treatment decisions.
TSH levels can be categorized as:
- Mildly suppressed: 0.1-0.4 mIU/L
- Moderately suppressed: 0.01-0.1 mIU/L
- Severely suppressed: Below 0.01 mIU/L
The degree of suppression often correlates with the severity of the underlying condition and helps guide treatment approaches.
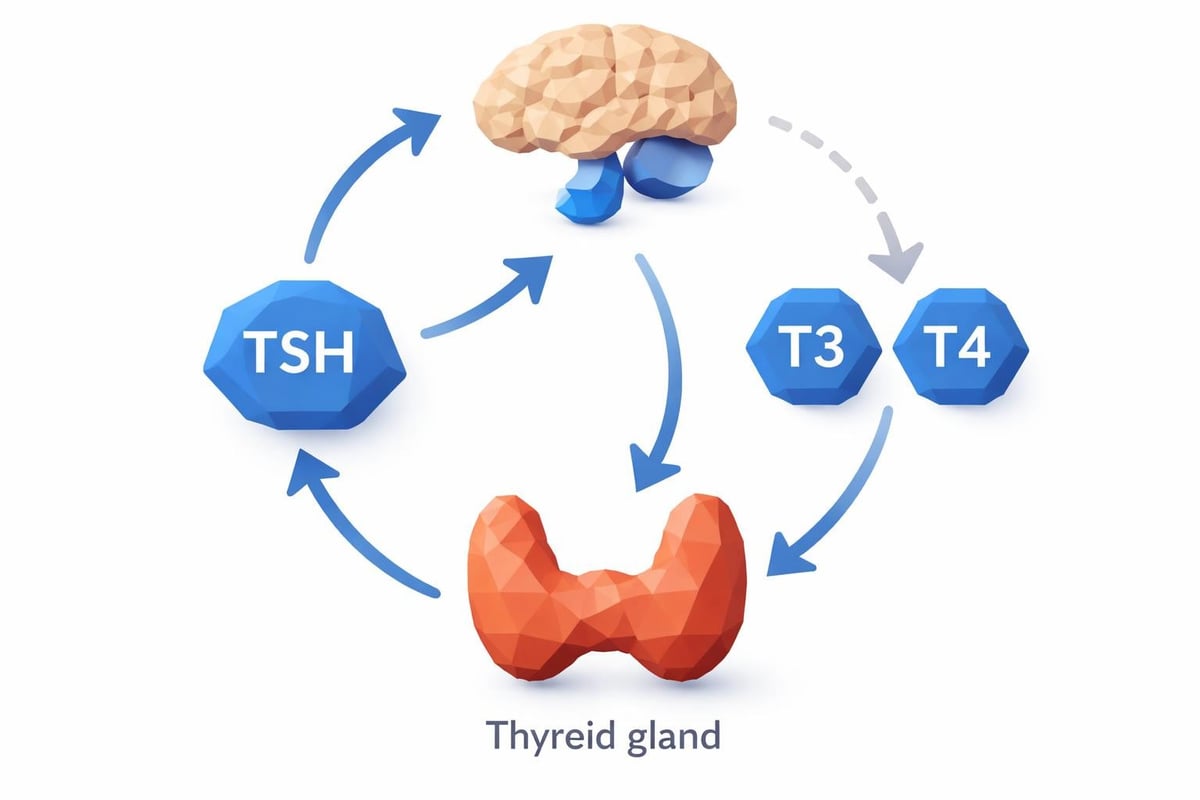
Primary Causes of Low TSH Levels
Several distinct conditions can push TSH levels below the normal threshold. Identifying the specific cause requires additional testing beyond the initial TSH measurement.
Hyperthyroidism
Hyperthyroidism and low TSH levels are closely connected, as an overactive thyroid produces excessive amounts of thyroid hormones. When T3 and T4 levels surge, the pituitary gland responds by dramatically reducing TSH production. This represents the body's attempt to slow down thyroid hormone production, though the effort proves unsuccessful in true hyperthyroidism.
Common causes of hyperthyroidism include:
- Graves' disease: An autoimmune condition where antibodies stimulate excessive thyroid hormone production
- Toxic multinodular goiter: Multiple thyroid nodules independently produce thyroid hormones
- Toxic adenoma: A single overactive nodule in the thyroid gland
- Thyroiditis: Inflammation causing temporary thyroid hormone release
Thyroid Medication Overmedication
Patients taking levothyroxine or other thyroid replacement medications can develop low TSH if their dosage exceeds their body's needs. This scenario is particularly common after dosage adjustments, weight changes, or when switching between different thyroid medication brands. The excessive thyroid hormone from medication suppresses TSH production just as hyperthyroidism does.
Subclinical Hyperthyroidism
Subclinical hyperthyroidism presents as low TSH with normal free T3 and free T4 levels. This condition occupies a gray area in thyroid disorders, often requiring careful monitoring rather than immediate treatment. However, it can progress to overt hyperthyroidism and carries cardiovascular risks in some patients, particularly older adults.
| Condition | TSH Level | Free T4 | Free T3 | Symptoms |
|---|---|---|---|---|
| Overt Hyperthyroidism | Low/Suppressed | High | High | Present |
| Subclinical Hyperthyroidism | Low/Suppressed | Normal | Normal | Minimal/Absent |
| Medication Overtreatment | Low/Suppressed | High | Normal/High | Variable |
| Central Hypothyroidism | Low/Normal | Low | Low | Present |
Recognizing Symptoms Associated with Low TSH
The symptoms you experience with low TSH depend heavily on whether your thyroid hormone levels are elevated. When low TSH occurs alongside high thyroid hormones, symptoms can be quite pronounced.
Physical Symptoms
Excess thyroid hormone accelerates your metabolism, creating a cascade of physical effects. Patients frequently report unexplained weight loss despite maintaining or increasing their caloric intake. Heart palpitations and rapid heartbeat are particularly concerning symptoms that warrant immediate medical attention.
Additional physical manifestations include:
- Tremors in the hands
- Increased sweating and heat intolerance
- Frequent bowel movements or diarrhea
- Muscle weakness, particularly in the upper arms and thighs
- Thinning hair or hair loss
- Changes in menstrual patterns for women
Neurological and Emotional Symptoms
The nervous system responds strongly to elevated thyroid hormones. Anxiety and nervousness often intensify, even in individuals without previous anxiety disorders. Sleep disturbances become common as the body remains in an elevated metabolic state. Difficulty concentrating and racing thoughts can interfere with work and daily activities.
Some patients with low TSH levels experience minimal symptoms, especially in cases of subclinical hyperthyroidism. This underscores the importance of regular testing rather than relying solely on symptom awareness.
Diagnostic Approach for Low TSH
When a TSH test reveals low levels, medical professionals follow a systematic approach to determine the underlying cause and appropriate treatment strategy.
Initial Follow-Up Testing
A single low TSH reading rarely provides enough information for definitive diagnosis. Healthcare providers typically order comprehensive thyroid panels that include:
- Free T4 (thyroxine): Measures the active, unbound form of T4
- Free T3 (triiodothyronine): Assesses the most metabolically active thyroid hormone
- TSH repeat measurement: Confirms the initial finding
- Thyroid antibodies: Identifies autoimmune thyroid conditions
These tests help distinguish between different causes of low TSH and guide treatment decisions. For individuals seeking convenient access to thyroid testing, lab testing without insurance provides an affordable option for obtaining comprehensive thyroid panels.
Recommended Test
TSH (Thyroid Stimulating Hormone)
The TSH test is the gold standard for evaluating thyroid function. It's the first test doctors order when thyroid problems are suspected.
Includes 1 biomarkers
$9
Advanced Diagnostic Testing
Depending on initial results, additional testing may include thyroid ultrasound to visualize the gland's structure, radioactive iodine uptake scans to assess thyroid activity, or thyroid receptor antibody tests specific to Graves' disease. These specialized tests help pinpoint the exact mechanism causing thyroid dysfunction.
Treatment Strategies for Different Causes
The appropriate treatment for low TSH varies dramatically based on the underlying cause. A personalized approach ensures optimal outcomes while minimizing treatment risks.
Managing Medication-Induced Low TSH
When thyroid medication overtreatment causes low TSH, the solution typically involves dosage adjustment. Healthcare providers usually reduce the medication dose by small increments, then retest TSH levels after 6-8 weeks to assess the response. This gradual approach prevents overcorrection that could lead to hypothyroidism.
Dosage adjustment considerations:
- Never adjust thyroid medication without medical supervision
- Take medication consistently at the same time daily
- Avoid taking thyroid medication with supplements or foods that interfere with absorption
- Report any new medications to your healthcare provider, as drug interactions can affect thyroid hormone levels
Treating Hyperthyroidism
Hyperthyroidism requires more intensive intervention. Treatment options include antithyroid medications that block thyroid hormone production, radioactive iodine therapy that permanently reduces thyroid function, or surgical removal of part or all of the thyroid gland. The choice depends on the specific cause, severity, patient age, and individual preferences.
Monitoring Subclinical Hyperthyroidism
Understanding low TSH causes and symptoms helps patients recognize when subclinical hyperthyroidism requires intervention versus observation. Many cases resolve spontaneously, but regular monitoring every 6-12 months remains essential to catch progression to overt hyperthyroidism.
Treatment may be recommended for subclinical hyperthyroidism when:
- TSH remains below 0.1 mIU/L persistently
- Patients develop symptoms
- Bone density decreases
- Cardiac arrhythmias develop
- Patients are over 65 years old
Special Populations and Low TSH Considerations
Certain groups face unique challenges and risks when dealing with low TSH levels.
Pregnancy and Low TSH
During pregnancy, TSH levels naturally decrease slightly in the first trimester due to hormonal changes. However, significantly suppressed TSH can increase risks for both mother and baby. Pregnant women require careful monitoring and often need medication adjustments to maintain optimal thyroid function throughout pregnancy.
Older Adults
Elderly patients with low TSH face increased risks of atrial fibrillation, heart failure, and accelerated bone loss. These cardiovascular and skeletal risks often warrant treatment even for subclinical hyperthyroidism in this age group. Conservative treatment approaches balance symptom relief against potential medication side effects.
Athletes and Active Individuals
Low TSH can significantly impact physical performance and recovery. The increased metabolic rate may initially seem beneficial but often leads to muscle wasting, decreased endurance, and prolonged recovery times. Athletes experiencing unexplained performance changes should consider thyroid function testing.
The Importance of Regular Monitoring
Whether you're taking thyroid medication, have been diagnosed with hyperthyroidism, or are monitoring subclinical thyroid dysfunction, consistent testing remains crucial for optimal health outcomes.
Testing Frequency Recommendations
The appropriate testing schedule depends on your specific situation:
| Clinical Scenario | Recommended Testing Frequency |
|---|---|
| New thyroid medication | 6-8 weeks after each dose change |
| Stable on medication | Every 6-12 months |
| Active hyperthyroidism treatment | Every 4-6 weeks initially |
| Subclinical hyperthyroidism | Every 6-12 months |
| Pregnancy with thyroid issues | Every 4 weeks |
These guidelines provide general frameworks, but individual circumstances may require more or less frequent monitoring based on symptom changes, medication adjustments, or other health factors.
Accessing Convenient Testing Options
Regular monitoring becomes more manageable when testing is accessible and affordable. Many patients appreciate the convenience of ordering their own tests without navigating insurance requirements or scheduling doctor appointments for routine monitoring. Ordering lab tests online streamlines the process, providing quick results that can be shared with healthcare providers.
Recommended Panel
Complete Thyroid Panel
Save $3Our most comprehensive thyroid panel includes all 5 essential markers: TSH, Free T4, Free T3, Reverse T3, and both thyroid antibodies. Get the complete picture of your thyroid health.
Includes 6 biomarkers
$84
Lifestyle Factors That Influence TSH Levels
While underlying medical conditions primarily drive low TSH, certain lifestyle factors can influence thyroid function and test results.
Medications and Supplements
Beyond thyroid replacement medications, several other drugs can affect TSH levels. Corticosteroids, dopamine agonists, and some antidepressants may suppress TSH. Biotin supplements, increasingly popular for hair and nail health, can interfere with thyroid test accuracy, causing falsely low TSH readings. Discontinuing biotin supplements at least 48 hours before thyroid testing ensures accurate results.
Stress and Illness
Severe physical stress from illness, surgery, or significant injury can temporarily suppress TSH through a phenomenon called "non-thyroidal illness syndrome." This represents a physiological adaptation rather than true thyroid disease. TSH typically normalizes after recovery from the acute stressor.
Timing and Consistency
TSH levels fluctuate throughout the day, typically highest in the early morning and lowest in the afternoon. For consistent monitoring, schedule thyroid tests at the same time of day, preferably in the morning. If taking thyroid medication, consider testing before taking your daily dose for the most accurate assessment of your baseline thyroid function.
When to Seek Immediate Medical Attention
While many cases of low TSH require routine follow-up, certain symptoms demand urgent evaluation.
Seek immediate medical care if you experience:
- Severe chest pain or rapid, irregular heartbeat
- Difficulty breathing or shortness of breath
- Severe weakness or inability to stand
- Confusion or significant changes in mental status
- Fever combined with thyroid symptoms
These symptoms may indicate thyroid storm, a rare but life-threatening complication of severe hyperthyroidism, or other serious cardiac complications that require emergency treatment.
The Connection Between Low TSH and Long-Term Health
Understanding the broader health implications of untreated or poorly managed low TSH motivates consistent monitoring and appropriate treatment. Research on low TSH demonstrates connections to several long-term health concerns.
Cardiovascular Risks
Prolonged exposure to excess thyroid hormone or suppressed TSH increases the risk of atrial fibrillation, a heart rhythm disorder that raises stroke risk. Heart muscle changes can develop over time, potentially leading to heart failure in severe cases. Even subclinical hyperthyroidism carries cardiovascular risks, particularly in older adults.
Bone Health Concerns
Thyroid hormones influence bone metabolism. Excess thyroid hormone accelerates bone turnover, leading to decreased bone density and increased fracture risk. This effect is particularly concerning for postmenopausal women who already face elevated osteoporosis risk. Managing low TSH appropriately helps preserve bone health.
Metabolic Consequences
The hypermetabolic state from uncontrolled hyperthyroidism causes muscle wasting despite adequate protein intake. This can lead to significant functional impairment and reduced quality of life. Proper treatment restores normal metabolism and allows for muscle mass recovery.
Distinguishing Between Central and Primary Thyroid Disorders
While most cases of low TSH indicate excessive thyroid hormone, rare situations involve pituitary or hypothalamic dysfunction causing inappropriately low TSH despite low thyroid hormone levels.
Central Hypothyroidism
This uncommon condition occurs when the pituitary gland fails to produce adequate TSH, or the hypothalamus doesn't properly signal TSH release. Unlike primary hyperthyroidism, central hypothyroidism presents with low or inappropriately normal TSH alongside low thyroid hormones. This pattern requires specialized endocrine evaluation and different treatment approaches.
Diagnostic Clues
Healthcare providers consider central hypothyroidism when patients have symptoms of hypothyroidism with low or normal TSH. Additional pituitary hormone testing and brain imaging may be necessary to identify pituitary tumors, previous brain injury, or other causes of pituitary dysfunction.
Optimizing Your Thyroid Health Journey
Managing low TSH effectively requires partnership between patients and healthcare providers, informed decision-making, and consistent monitoring.
Keeping Accurate Records
Maintain a log of your thyroid test results, medication doses, and symptoms. This historical perspective helps identify patterns and guides treatment adjustments. Note the laboratory that performed each test, as reference ranges can vary between facilities.
Communicating with Healthcare Providers
Share all medications, supplements, and health changes with your medical team. Report new symptoms promptly rather than waiting for scheduled appointments. Ask questions about your test results and treatment plan to ensure you understand the rationale behind recommendations.
Empowering Yourself Through Knowledge
Understanding what low TSH means, what causes it, and how it affects your health enables you to participate actively in your care. While healthcare providers guide treatment decisions, your insights about symptoms and quality of life are invaluable for optimizing management strategies.
Understanding whether your low TSH stems from hyperthyroidism, medication overtreatment, or another cause is essential for receiving appropriate care and preventing long-term complications. Regular monitoring through accessible, affordable testing helps you stay informed about your thyroid health and make timely adjustments when needed. Justlabs makes thyroid testing convenient and transparent, with online ordering, competitive pricing, and results delivered in 1-3 days, empowering you to take control of your health without the hassle of insurance or unnecessary doctor visits for routine monitoring.