Understanding the difference between temporary stress responses and chronic high cortisol levels can be challenging. While everyone experiences elevated cortisol during stressful situations, persistent elevation may indicate serious underlying conditions like Cushing's syndrome that require medical attention. Recognizing when your body's stress hormone has crossed from normal adaptation to medical concern is essential for maintaining long-term health.
Understanding Cortisol and Its Role in Your Body
Cortisol is a steroid hormone produced by your adrenal glands that plays a crucial role in numerous bodily functions. Often called the "stress hormone," it helps regulate metabolism, immune response, blood pressure, and blood sugar levels.
Your body naturally produces varying amounts of cortisol throughout the day, with levels typically peaking in the early morning and declining as evening approaches. This circadian rhythm ensures you have energy to start your day and can relax at night.
Normal cortisol functions include:
- Regulating glucose metabolism and blood sugar
- Controlling blood pressure
- Reducing inflammation
- Supporting memory formation
- Managing salt and water balance
When faced with stress, your adrenal glands release extra cortisol as part of the fight-or-flight response. This temporary elevation is completely normal and beneficial. Problems arise when cortisol levels remain elevated for extended periods, potentially causing serious health complications.
Common High Cortisol Symptoms from Everyday Stress
Temporary stress-related cortisol elevation produces symptoms that most people experience occasionally. These symptoms typically resolve once the stressful situation passes or you implement effective stress management techniques.
Physical Manifestations of Stress
Sleep disturbances represent one of the most common effects of elevated cortisol from stress. You may find it difficult to fall asleep, wake frequently during the night, or feel unrested despite adequate sleep time.
Energy fluctuations often accompany stress-related cortisol changes. Many people experience an initial surge of energy followed by afternoon crashes or persistent fatigue that differs from normal tiredness.
- Tension headaches or migraines
- Muscle tension, particularly in neck and shoulders
- Digestive issues including upset stomach or changes in appetite
- Minor weight fluctuations
- Increased heart rate or palpitations
Cognitive and Emotional Effects
Mental fog and concentration difficulties frequently occur when stress keeps cortisol elevated. You might struggle to focus on tasks that normally come easily or find yourself forgetting details.
Mood changes ranging from irritability to anxiety are hallmark signs of stress-induced cortisol elevation. These emotional shifts typically correspond directly with stressful events and improve when stress decreases.
According to experts who study cortisol patterns, daily hormone fluctuations become more pronounced during stressful periods, potentially amplifying normal ups and downs in energy and mood.
Medical Conditions: Cushing's Syndrome and Chronic Hypercortisolism
Unlike temporary stress responses, certain medical conditions cause persistently high cortisol symptoms that require professional diagnosis and treatment. Cushing's syndrome represents the most well-known condition characterized by chronic cortisol excess.
What is Cushing's Syndrome?
Cushing's syndrome occurs when your body is exposed to high levels of cortisol for extended periods. This can result from various causes including pituitary tumors, adrenal gland tumors, or long-term use of corticosteroid medications.
The condition affects approximately 10 to 15 people per million annually, making it relatively rare compared to stress-related cortisol fluctuations. However, its effects can be severe and progressive without proper treatment.
| Cause | Prevalence | Primary Mechanism |
|---|---|---|
| Pituitary adenomas (Cushing's disease) | 70% of cases | Tumor causes excess ACTH production |
| Adrenal tumors | 15-20% of cases | Tumor directly produces cortisol |
| Ectopic ACTH syndrome | 10-15% of cases | Non-pituitary tumors produce ACTH |
| Exogenous steroids | Variable | Long-term medication use |
Distinguishing Medical Symptoms
High cortisol symptoms from medical conditions manifest differently than stress-related effects. These signs develop gradually and persist regardless of lifestyle changes or stress reduction efforts.
Characteristic physical changes include:
- Progressive central weight gain with fat accumulation around midsection and upper back ("buffalo hump")
- Moon-shaped face with redness
- Purple or pink stretch marks (striae) wider than 1 cm
- Easy bruising and thin, fragile skin
- Slow wound healing
- Severe fatigue that doesn't improve with rest
Women may experience irregular menstrual periods or cessation of menstruation entirely, while men often develop erectile dysfunction. Both sexes may notice decreased libido and fertility issues.
Bone density loss occurs rapidly with chronic hypercortisolism, leading to osteoporosis and increased fracture risk even in younger individuals. This differs significantly from age-related bone loss.

Metabolic and Cardiovascular Complications
Persistently elevated cortisol creates cascading effects throughout multiple body systems. Understanding these complications helps differentiate between temporary stress and medical concerns requiring intervention.
Blood Sugar and Diabetes Risk
Cortisol directly opposes insulin action, causing blood sugar to rise. While temporary stress-related increases pose minimal risk for healthy individuals, chronic elevation significantly increases type 2 diabetes risk.
People with undiagnosed Cushing's syndrome often develop insulin resistance and diabetes months or years before other symptoms become obvious. Monitoring glucose levels through accessible lab testing can identify these metabolic changes early.
Cardiovascular Strain
High blood pressure develops in approximately 80% of people with Cushing's syndrome. This hypertension often proves resistant to standard treatments and increases risks for:
- Heart attack
- Stroke
- Heart failure
- Arrhythmias
The cardiovascular effects stem from multiple mechanisms including increased blood volume, enhanced blood vessel sensitivity to constricting substances, and altered salt retention. Unlike stress-related temporary blood pressure spikes, these changes persist and worsen over time.
Mental Health Implications Beyond Normal Stress
While everyday stress causes temporary mood changes, chronic hypercortisolism produces profound psychiatric effects that don't respond to typical stress management approaches.
Depression affects 50-70% of individuals with Cushing's syndrome, often presenting as severe, treatment-resistant depression. The biochemical changes caused by excess cortisol alter neurotransmitter function in ways that differ fundamentally from stress-related mood changes.
Anxiety disorders, panic attacks, and cognitive impairment including memory problems occur frequently. Some individuals develop psychotic symptoms or severe mood swings resembling bipolar disorder.
These mental health manifestations often bring patients to psychiatrists or psychologists first, potentially delaying recognition of the underlying hormonal problem. Psychiatrists should consider hormonal evaluation when patients don't respond to standard treatments.
When to Suspect a Medical Problem vs Normal Stress
Determining whether your symptoms warrant medical investigation requires honest assessment of symptom patterns, severity, and response to stress reduction efforts.
Red Flags Requiring Evaluation
Certain symptom combinations strongly suggest underlying medical conditions rather than stress alone. Seek medical evaluation if you experience multiple symptoms from this list simultaneously:
- Unexplained weight gain concentrated in face, neck, and abdomen while arms and legs remain thin
- New stretch marks that are purple, pink, or red and wider than pencil width
- Muscle weakness making it difficult to rise from seated position or climb stairs
- Easy bruising with minimal trauma
- Bone fractures with minor injury
- Persistent high blood pressure uncontrolled by medication
- New diabetes diagnosis or worsening blood sugar control
The timing and progression of symptoms provide important clues. Stress-related symptoms fluctuate with life circumstances and improve during vacations or low-stress periods. Medical conditions cause steadily worsening symptoms regardless of stress levels.
Documentation and Tracking
Keeping detailed records helps both you and healthcare providers identify patterns. Note when symptoms occur, their severity, and any triggering events or relieving factors.
Taking photographs at regular intervals can document physical changes that develop too gradually to notice day-to-day. This visual record proves especially valuable for facial changes, weight distribution, and skin changes.
Diagnostic Approaches and Testing Options
Confirming high cortisol symptoms requires specific laboratory testing that measures hormone levels in various ways. Understanding available tests helps you work effectively with healthcare providers.
Initial Screening Tests
Three primary screening tests assess cortisol excess, each measuring different aspects of hormone production and regulation.
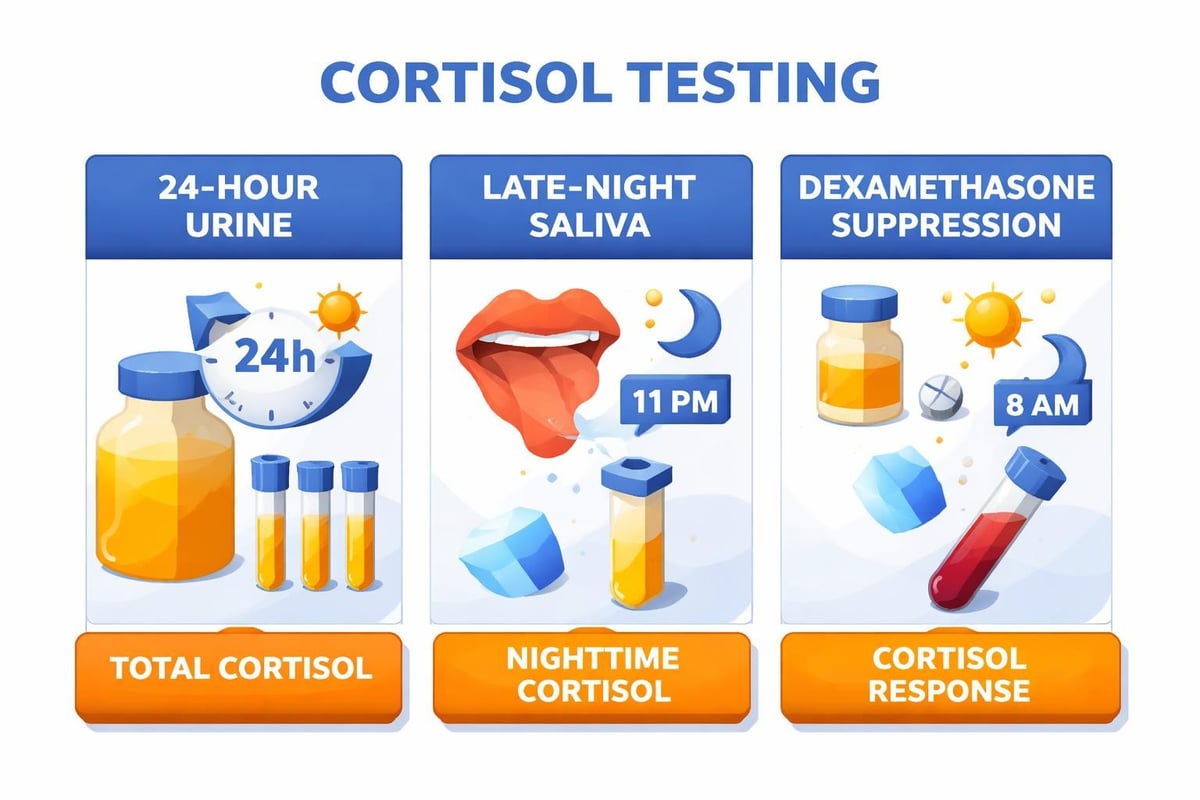
| Test Type | Collection Method | What It Measures | Advantages |
|---|---|---|---|
| 24-hour urine free cortisol | Urine collection over 24 hours | Total cortisol excreted daily | Reflects average production |
| Late-night salivary cortisol | Saliva sample at 11 PM-midnight | Cortisol at time it should be lowest | Convenient, non-invasive |
| Low-dose dexamethasone suppression | Blood draw after taking medication | Whether cortisol production can be suppressed | Tests regulation mechanism |
Many people find ordering labs without requiring a doctor's visit provides faster access to initial screening, especially when symptoms are concerning but not severe enough for emergency care.
Confirmatory and Specialized Testing
If screening tests suggest hypercortisolism, additional testing determines the underlying cause. ACTH levels help distinguish between pituitary-driven disease, adrenal tumors, and other causes.
Imaging studies including MRI of the pituitary gland and CT scans of the adrenal glands locate tumors or abnormalities. Specialized tests like the CRH stimulation test or bilateral inferior petrosal sinus sampling may be necessary for complex cases.
Getting test results quickly matters when you're concerned about your health. With rapid turnaround times of 1-3 days, you can move forward with appropriate next steps without extended waiting periods.
Recommended Test
Cortisol, Total
Cortisol is your body's primary stress hormone, produced by the adrenal glands. This test measures total cortisol levels to assess adrenal function and stress response.
Includes 1 biomarkers
$15
Recommended Test
DHEA-Sulfate
DHEA-S is the most abundant hormone in your body and serves as a precursor to testosterone and estrogen. Levels naturally decline with age, making this test useful for assessing adrenal function and hormonal aging.
Includes 1 biomarkers
$14
Managing Stress-Related Cortisol Elevation
When testing confirms your symptoms stem from stress rather than medical conditions, evidence-based lifestyle modifications can restore healthy cortisol patterns.
Immediate Stress Reduction Techniques
Mindfulness practices and meditation effectively lower cortisol levels with consistent practice. Even brief daily sessions of 10-15 minutes produce measurable benefits. Resources focused on stress management provide structured approaches for beginners.
Effective stress management strategies include:
- Regular exercise, particularly moderate-intensity activities like walking or swimming
- Adequate sleep with consistent schedule (7-9 hours nightly)
- Social connection and meaningful relationships
- Time in nature
- Limiting caffeine and alcohol
- Engaging in enjoyable hobbies
Nutritional Approaches
Diet influences cortisol production and stress response. Balanced nutrition with adequate protein, healthy fats, and complex carbohydrates supports stable blood sugar and hormone regulation.
Certain nutrients specifically support healthy stress response including vitamin C, magnesium, omega-3 fatty acids, and B vitamins. While supplements may help some individuals, focusing on nutrient-dense whole foods provides the most reliable benefits.
Avoiding prolonged fasting or severe calorie restriction prevents additional stress on your body. Eating regular meals maintains stable blood sugar and reduces cortisol spikes triggered by energy deficits.
Treatment Options for Medical Hypercortisolism
Medical conditions causing high cortisol symptoms require specific treatments targeting the underlying cause. Treatment approaches vary based on whether the problem originates in the pituitary gland, adrenal glands, or elsewhere.
Surgical Interventions
Transsphenoidal surgery to remove pituitary adenomas represents first-line treatment for Cushing's disease, with cure rates of 70-90% when performed by experienced surgeons. The procedure accesses the pituitary through the nose, avoiding brain surgery.
Adrenalectomy removes one or both adrenal glands when tumors cause excess cortisol production. Unilateral adrenalectomy for benign adenomas typically cures the condition without requiring lifelong hormone replacement.
Medical Management
When surgery isn't possible or doesn't achieve cure, medications can block cortisol production or action. Options include ketoconazole, metyrapone, mitotane, and mifepristone, each working through different mechanisms.
Radiation therapy treats pituitary tumors that can't be completely removed surgically or that recur after surgery. Effects develop gradually over months to years rather than providing immediate symptom relief.
Monitoring and Long-term Follow-up
Both stress management and medical treatment require ongoing monitoring to ensure effectiveness and catch any complications early.
What to Track
Regular assessment of symptoms helps gauge whether interventions are working. Keep records of weight, blood pressure, energy levels, mood, and any physical changes.
Periodic laboratory testing confirms cortisol levels remain in healthy ranges. After successful treatment for Cushing's syndrome, patients need lifelong monitoring since recurrence can occur years later.
Many individuals benefit from checking related metabolic markers including blood glucose, lipids, and thyroid function. Understanding your lab results empowers you to have informed discussions with healthcare providers about your health trends.
Addressing Complications
Even after successful treatment, some effects of prolonged hypercortisolism may persist. Bone density loss requires specific treatment with calcium, vitamin D, and sometimes medications to rebuild bone strength.
Cardiovascular changes may improve gradually but often need continued management. Working with cardiologists or internists ensures appropriate monitoring and treatment of any lasting effects.
Mental health support remains important during recovery. The psychological impact of chronic illness combined with hormonal shifts during treatment can be challenging. Professional counseling or support groups help many people navigate this adjustment period.
The Importance of Self-Advocacy in Healthcare
Distinguishing between stress and medical conditions requires trusting your instincts about your body while seeking appropriate professional guidance.
Don't dismiss persistent symptoms as "just stress" if they don't improve with stress management efforts or if they progressively worsen. Healthcare providers may initially attribute vague symptoms like fatigue or weight gain to lifestyle factors, making self-advocacy essential.
However, misconceptions about cortisol testing and treatment have increased recently due to misinformation on social media. Balance concern about symptoms with reliance on evidence-based testing and professional medical guidance rather than self-diagnosis.
Access to testing shouldn't create barriers to investigation. Services offering labs without insurance requirements at transparent prices remove common obstacles to getting answers about concerning symptoms.
Lifestyle Factors That Influence Cortisol Beyond Stress
While stress management is crucial, other lifestyle factors significantly impact cortisol regulation and overall hormonal health.
Sleep quality and timing affect cortisol rhythms more than most people realize. Irregular sleep schedules, insufficient sleep, or poor sleep quality disrupt normal cortisol patterns even without increased stress.
Shift work and frequent time zone changes particularly challenge cortisol regulation by repeatedly forcing the body to adapt to new schedules. People in these situations benefit from extra attention to sleep hygiene and stress management.
Physical activity influences cortisol in complex ways. Moderate exercise helps regulate healthy cortisol patterns and improves stress response, while excessive high-intensity training without adequate recovery can chronically elevate cortisol.
Social connections and emotional support buffer stress responses and help maintain healthy cortisol levels. Loneliness and social isolation associate with dysregulated cortisol patterns independent of other stressors.
Prevention and Risk Awareness
Understanding risk factors for both stress-related cortisol elevation and medical causes helps you take preventive action and recognize problems early.
Reducing Stress-Related Risk
Building resilience before major stressors occur provides better protection than trying to cope during crisis periods. Regular stress management practices, strong social networks, and healthy lifestyle habits create buffers against cortisol dysregulation.
Recognizing early signs of chronic stress allows intervention before symptoms become severe. Addressing manageable stress through lifestyle changes prevents progression to more serious problems.
Medical Risk Factors
Long-term corticosteroid use for conditions like asthma, autoimmune diseases, or inflammatory conditions represents the most common cause of medication-induced Cushing's syndrome. If you require these medications, work closely with prescribers to use the lowest effective doses.
Family history of endocrine tumors may increase risk for pituitary or adrenal adenomas, though most cases occur sporadically without family connection. Certain genetic syndromes increase risk for multiple endocrine tumors including those affecting cortisol production.
Regular health monitoring catches early changes before they become problematic. Annual checkups with basic metabolic testing identify trends in weight, blood pressure, and blood sugar that may signal developing problems.
Integrating Professional Care with Self-Management
Successfully managing high cortisol symptoms, whether from stress or medical conditions, requires partnership between individual effort and professional healthcare.
For stress-related elevation, healthcare providers can help identify contributing factors you might overlook and suggest targeted interventions. Therapists, nutritionists, and other specialists offer expertise that complements self-care efforts.
Medical conditions absolutely require professional diagnosis and treatment, but patient engagement in care improves outcomes. Understanding your condition, asking questions, and actively participating in treatment decisions leads to better results than passive acceptance of recommendations.
Expert guidance on lowering cortisol emphasizes that sustainable approaches combine multiple strategies rather than relying on single interventions. This integrative approach applies whether you're managing everyday stress or recovering from Cushing's syndrome treatment.
Access to information through reliable healthcare resources supports informed decision-making. However, information should guide discussions with healthcare providers rather than replace professional evaluation and diagnosis.
Recognizing whether your high cortisol symptoms stem from everyday stress or signal serious medical conditions like Cushing's syndrome empowers you to take appropriate action for your health. While temporary stress responses resolve with lifestyle modifications, persistent symptoms warrant medical evaluation and testing. Justlabs provides convenient access to cortisol testing and other hormone panels at transparent prices, with results in 1-3 days, helping you get answers quickly when you're concerned about your health. Taking control of your testing journey means you can address symptoms promptly and work with healthcare providers from an informed position.