Many people receive a diagnosis of hypothyroidism and assume they understand their condition completely. However, the distinction between hashimoto vs hypothyroidism represents a critical piece of medical information that affects treatment approaches, long-term health outcomes, and daily management strategies. While these terms are often used interchangeably, they describe different aspects of thyroid health that require specific attention and care.
Understanding the Fundamental Difference
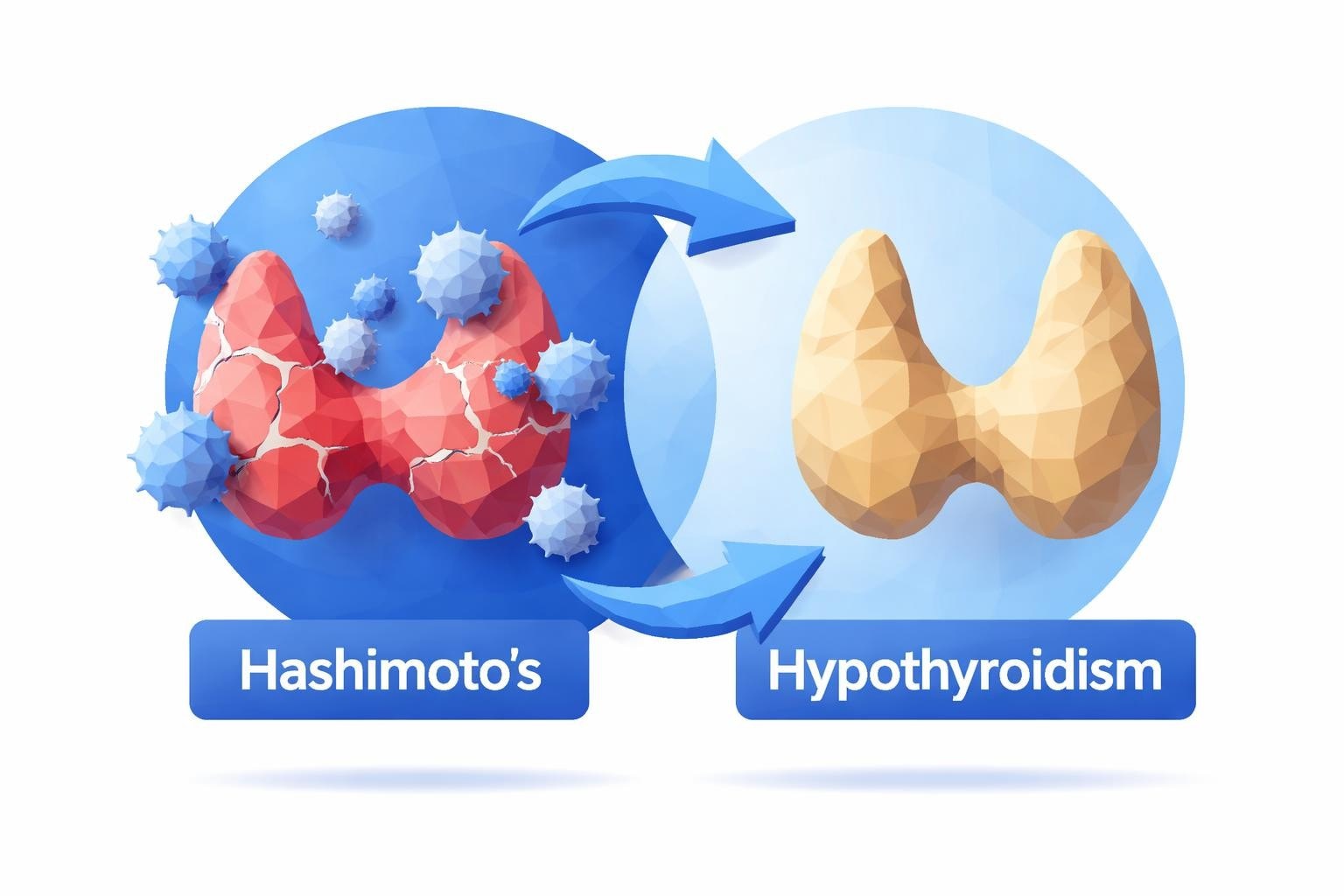
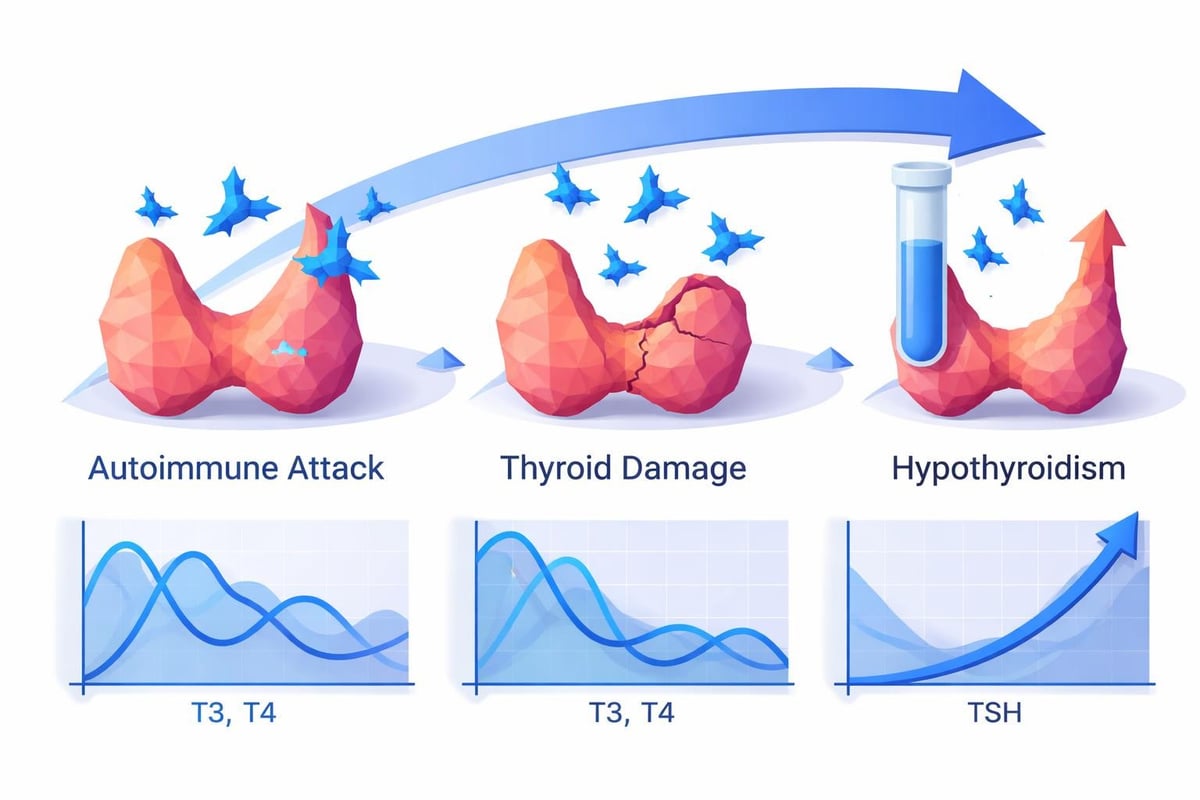
The confusion surrounding hashimoto vs hypothyroidism stems from their interconnected relationship. Hypothyroidism is a condition where your thyroid gland produces insufficient thyroid hormones, leading to a slower metabolism and various systemic effects throughout your body. Hashimoto's thyroiditis, on the other hand, is an autoimmune disease that attacks the thyroid gland and frequently causes hypothyroidism.
Think of it this way: hypothyroidism describes what is happening in your body (low thyroid hormone levels), while Hashimoto's explains why it's happening (autoimmune attack). This distinction matters because Hashimoto's is the most common cause of hypothyroidism in developed countries, but not all cases of hypothyroidism result from Hashimoto's disease.
Other Causes of Hypothyroidism
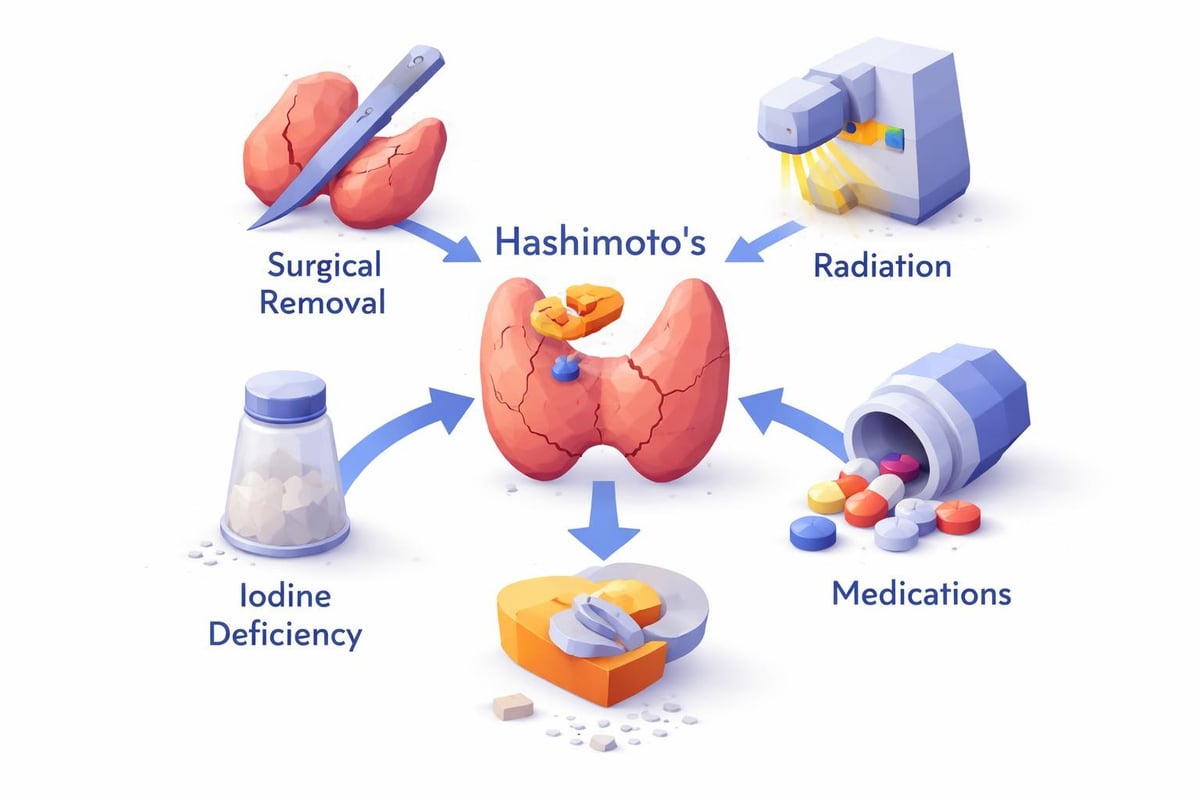
Beyond Hashimoto's, several conditions can lead to hypothyroidism:
- Surgical removal of the thyroid gland
- Radiation treatment for hyperthyroidism or cancer
- Certain medications, including lithium and amiodarone
- Iodine deficiency (rare in developed countries)
- Pituitary gland disorders affecting TSH production
- Congenital thyroid disorders present from birth
Understanding these various causes helps explain why approximately 90% of hypothyroidism cases in the United States result from Hashimoto's thyroiditis, while the remaining 10% have different underlying mechanisms. This statistic underscores the importance of proper diagnostic testing to identify the specific cause.
Symptoms: Where They Overlap and Diverge
When comparing hashimoto vs hypothyroidism symptoms, significant overlap exists because Hashimoto's eventually produces hypothyroidism in most patients. Both conditions share these common manifestations:
Classic hypothyroidism symptoms include:
- Persistent fatigue and low energy levels
- Unexplained weight gain or difficulty losing weight
- Cold intolerance and sensitivity to temperature
- Dry skin and brittle hair
- Constipation and digestive sluggishness
- Muscle weakness and joint pain
- Brain fog and difficulty concentrating
- Depression and mood changes
However, Hashimoto's presents additional considerations. During the early stages, some patients experience periods of hyperthyroidism (excess thyroid hormone) as the autoimmune attack damages thyroid cells and releases stored hormones into the bloodstream. This phenomenon, called "Hashitoxicosis," can cause temporary symptoms opposite to hypothyroidism.
Hashimoto's-Specific Indicators
| Symptom Category | Hypothyroidism Only | Hashimoto's Disease |
|---|---|---|
| Thyroid enlargement | Rare | Common (goiter) |
| Fluctuating symptoms | Stable progression | Variable, may cycle |
| Autoimmune markers | Absent | Present in blood |
| Other autoimmune conditions | Unrelated | Often coexist |
| Response to treatment | Predictable | May need adjustment |
People with Hashimoto's frequently develop other autoimmune conditions, including celiac disease, rheumatoid arthritis, Type 1 diabetes, and vitiligo. This clustering of autoimmune disorders rarely occurs with non-autoimmune hypothyroidism, making it a distinguishing characteristic worth monitoring.
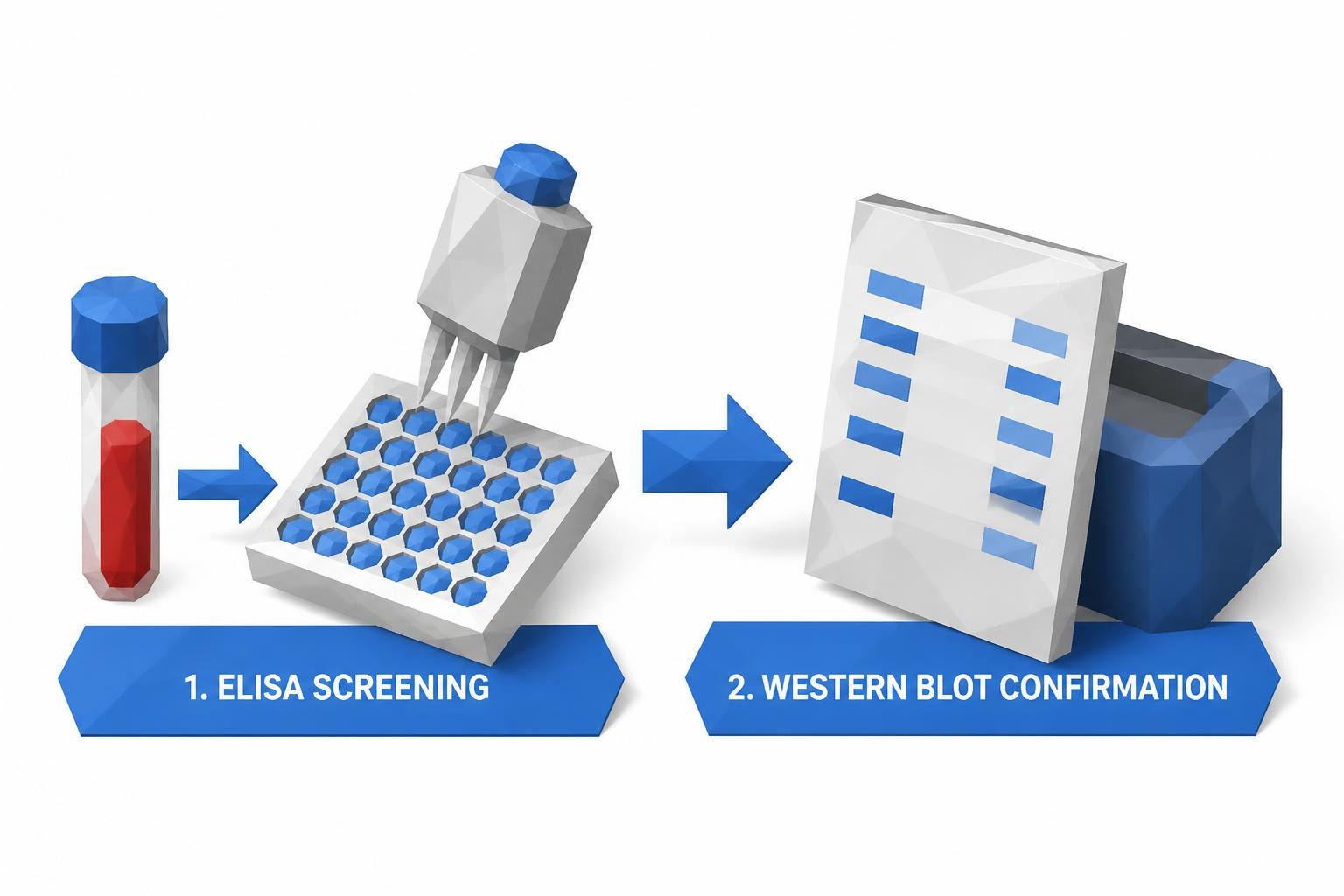
Diagnostic Testing: Identifying the Root Cause
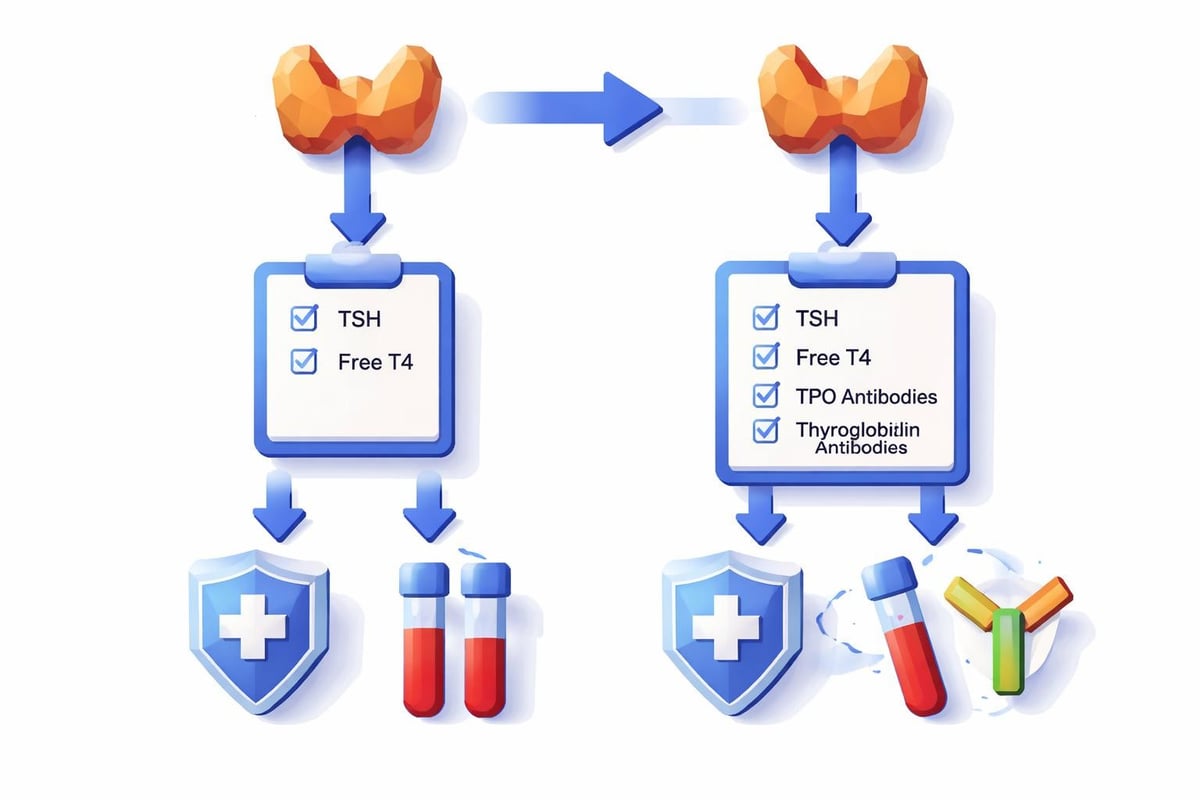
The laboratory testing approach definitively answers the hashimoto vs hypothyroidism question. While both conditions show elevated TSH (thyroid-stimulating hormone) and low free T4 levels, Hashimoto's requires additional antibody testing for confirmation.
Essential Thyroid Tests
Standard hypothyroidism screening begins with TSH testing, which measures the pituitary hormone that regulates thyroid function. Elevated TSH indicates your pituitary is working overtime to stimulate an underactive thyroid gland. Many healthcare providers stop here, but this approach misses the autoimmune component entirely.
A comprehensive evaluation includes:
- TSH (Thyroid-Stimulating Hormone) - Screening test showing thyroid function status
- Free T4 (Thyroxine) - Measures actual thyroid hormone available to tissues
- Free T3 (Triiodothyronine) - Active form of thyroid hormone
- Thyroid Peroxidase Antibodies (TPO) - Elevated in 90% of Hashimoto's cases
- Thyroglobulin Antibodies (TgAb) - Present in 80% of Hashimoto's patients
When considering affordable thyroid testing options, accessing comprehensive panels that include antibody testing becomes crucial. Many patients discover their Hashimoto's diagnosis only after requesting antibody tests themselves, as standard protocols don't always include them.
Recommended Panel
Hashimoto's Panel
Save $3The definitive panel for diagnosing Hashimoto's thyroiditis - the #1 cause of hypothyroidism. Tests both major thyroid antibodies that indicate autoimmune thyroid disease.
Includes 5 biomarkers
$58
Why Antibody Testing Matters
Identifying Hashimoto's through positive antibody results changes the clinical approach significantly. Patients with confirmed autoimmune thyroid disease benefit from monitoring other autoimmune conditions, addressing inflammatory triggers, and potentially implementing dietary interventions that standard hypothyroidism patients don't require.
The ability to order lab tests without a doctor empowers patients to seek comprehensive thyroid panels when their healthcare providers might only order basic screening. This accessibility proves particularly valuable when advocating for thorough testing.
Recommended Test
TPO & TG Antibodies
This panel tests for both major thyroid antibodies that indicate autoimmune thyroid disease, the most common cause of thyroid problems.
Includes 2 biomarkers
$27
Treatment Approaches and Management Strategies
Understanding hashimoto vs hypothyroidism directly impacts treatment decisions. Both conditions typically require thyroid hormone replacement therapy, most commonly levothyroxine (synthetic T4). However, Hashimoto's management extends beyond simple hormone replacement.
Standard Thyroid Hormone Replacement
The primary treatment for both conditions involves daily thyroid hormone medication to normalize TSH levels and relieve symptoms. Dosing requires regular monitoring through blood tests, typically every 6-12 weeks initially, then annually once stable.
Treatment monitoring requires:
- Regular TSH testing to assess medication effectiveness
- Free T4 measurements to verify hormone levels
- Symptom tracking to ensure clinical improvement
- Dose adjustments based on lab results and symptoms
- Timing considerations for medication absorption
Some patients with Hashimoto's report better results with combination therapy (T4 plus T3) or natural desiccated thyroid, though research evidence remains mixed regarding superiority over levothyroxine alone.
Additional Hashimoto's Management
Beyond hormone replacement, Hashimoto's patients may benefit from addressing the autoimmune component directly. While no treatment currently reverses the autoimmune process, several strategies may help reduce inflammation and antibody levels.
Many practitioners recommend:
- Selenium supplementation (200 mcg daily) to potentially reduce TPO antibodies
- Vitamin D optimization through testing and supplementation if deficient
- Gluten elimination for patients with concurrent celiac disease or sensitivity
- Stress management techniques to reduce inflammatory triggers
- Regular antibody monitoring to track disease progression
Research into dietary modifications for Hashimoto's suggests that some patients experience symptom improvement and antibody reduction through nutritional interventions, though individual responses vary considerably.
The Autoimmune Factor: Long-Term Implications
The autoimmune nature of Hashimoto's creates unique considerations absent in other forms of hypothyroidism. Autoimmune diseases don't exist in isolation; having one increases your risk for developing others. This interconnection requires broader health monitoring beyond thyroid function alone.
Associated Autoimmune Conditions
| Condition | Prevalence in Hashimoto's | Screening Considerations |
|---|---|---|
| Celiac Disease | 4-6% (vs. 1% general population) | TTG antibodies, intestinal biopsy |
| Type 1 Diabetes | 3-4x higher risk | Fasting glucose, A1C testing |
| Rheumatoid Arthritis | 2-3x higher risk | RF antibodies, joint symptoms |
| Vitiligo | 7% of patients | Visual skin examination |
| Pernicious Anemia | Higher prevalence | B12 levels, intrinsic factor antibodies |
Understanding the differences between thyroid conditions helps patients recognize when new symptoms might signal an additional autoimmune disorder requiring evaluation. This awareness facilitates earlier diagnosis and intervention.
Pregnancy Considerations
Women with either condition face increased risks during pregnancy, but Hashimoto's presents additional challenges. The autoimmune attack may intensify or diminish during pregnancy, requiring careful monitoring and medication adjustments.
Pregnant women with Hashimoto's need:
- Pre-conception TSH optimization (ideally below 2.5 mIU/L)
- First-trimester medication increases (typically 30-50%)
- Monthly thyroid testing throughout pregnancy
- Postpartum monitoring for thyroid fluctuations
- Assessment for postpartum thyroiditis
The distinction in hashimoto vs hypothyroidism becomes particularly relevant during family planning, as antibody-positive women require more intensive monitoring regardless of current TSH levels.
When to Retest and Monitor Progress
Both hypothyroidism and Hashimoto's require ongoing laboratory monitoring, but the frequency and scope differ based on several factors. Stable patients on consistent medication dosing may only need annual testing, while those experiencing symptoms or medication changes require more frequent evaluation.
Recommended Testing Schedules
For newly diagnosed patients:
- Baseline comprehensive panel including TSH, Free T4, Free T3, and antibodies
- Follow-up testing 6-8 weeks after starting medication
- Continued monitoring every 6-8 weeks until TSH stabilizes
- Transition to every 6 months once stable
- Annual testing for well-controlled cases
Hashimoto's patients should periodically recheck antibody levels (annually or when symptoms change) to assess disease activity, while this testing provides no benefit for non-autoimmune hypothyroidism. The convenience of direct-access testing allows patients to monitor their condition proactively without waiting for annual physical examinations.
Reasons to Test Sooner
Certain situations warrant immediate retesting:
- New or worsening symptoms suggesting inadequate treatment
- Significant weight changes affecting medication requirements
- Starting medications that interfere with thyroid hormone absorption
- Pregnancy or postpartum period
- Changes in dietary patterns, especially regarding iodine intake
- Development of symptoms suggesting other autoimmune conditions
The ability to access affordable lab testing without insurance barriers enables responsive monitoring when circumstances change, rather than adhering to arbitrary annual schedules that may not align with individual needs.
Making Informed Decisions About Your Thyroid Health
Distinguishing between hashimoto vs hypothyroidism empowers patients to advocate effectively for comprehensive care. Many people live for years on thyroid medication without knowing whether autoimmune disease drives their condition. This knowledge gap prevents optimization of treatment approaches and misses opportunities for preventive care regarding associated conditions.
Key takeaways for patients:
- Request antibody testing (TPO and TgAb) if you've only had TSH checked
- Track symptoms systematically to identify patterns and treatment response
- Consider comprehensive thyroid panels rather than TSH-only testing
- Monitor for signs of other autoimmune conditions if Hashimoto's is confirmed
- Maintain regular testing schedules appropriate to your disease stability
- Explore evidence-based complementary approaches for autoimmune management
The medical landscape continues evolving regarding understanding the relationship between these conditions, with growing recognition that one-size-fits-all approaches don't serve all patients equally well. Personalized medicine requires accurate diagnosis as its foundation.
Taking Control of Your Testing
Many patients find that obtaining comprehensive testing through traditional healthcare channels proves challenging due to cost concerns, insurance limitations, or provider reluctance to order extensive panels. The healthcare system often operates on minimum necessary testing protocols, which may not capture the complete picture.
Direct-access laboratory services address these barriers by providing transparent pricing and comprehensive test options without requiring insurance pre-authorization or physician orders. This accessibility proves particularly valuable when seeking answers about autoimmune involvement or monitoring treatment effectiveness between scheduled appointments.
Understanding Your Test Results
Receiving thyroid test results represents only the first step; interpreting them correctly determines their value. Reference ranges vary between laboratories, and optimal levels for symptom resolution may differ from standard reference ranges.
| Test | Standard Range | Optimal Range (Symptoms) | Hashimoto's Consideration |
|---|---|---|---|
| TSH | 0.4-4.0 mIU/L | 0.5-2.0 mIU/L | May need lower target |
| Free T4 | 0.8-1.8 ng/dL | Upper half of range | Monitor conversion to T3 |
| Free T3 | 2.3-4.2 pg/mL | Upper half of range | May need supplementation |
| TPO Antibodies | <35 IU/mL | <35 IU/mL | Track trend over time |
| TgAb | <20 IU/mL | <20 IU/mL | Complement TPO testing |
Resources for understanding lab results help patients contextualize their numbers within both clinical ranges and symptom experience. Some people feel best with TSH near 1.0, while others require different levels for optimal function.
The Importance of Trend Analysis
Single test results provide limited information compared to tracking changes over time. Hashimoto's often progresses gradually, with increasing antibody levels preceding TSH elevation by months or years. Establishing baseline values and monitoring trends reveals disease trajectory better than isolated measurements.
Comparing hashimoto vs hypothyroidism through laboratory trends shows distinct patterns. Non-autoimmune hypothyroidism typically demonstrates stable TSH elevation responsive to consistent medication dosing. Hashimoto's may show fluctuating values as thyroid destruction progresses, requiring periodic medication adjustments even when previously stable.
The Role of Lifestyle and Environmental Factors
While medication forms the cornerstone of treatment for both conditions, lifestyle modifications may influence outcomes, particularly for Hashimoto's patients seeking to moderate autoimmune activity. Environmental triggers potentially exacerbate autoimmune responses in susceptible individuals.
Evidence-based lifestyle considerations include:
- Stress reduction through meditation, yoga, or other relaxation techniques
- Sleep optimization maintaining 7-9 hours of quality sleep nightly
- Regular exercise appropriate to energy levels and physical capacity
- Toxin avoidance minimizing exposure to endocrine disruptors
- Nutrient-dense diet emphasizing whole foods and adequate micronutrients
The distinction between hyperthyroidism and hypothyroidism helps patients understand that while some thyroid conditions respond dramatically to dietary changes alone, hypothyroidism (whether from Hashimoto's or other causes) consistently requires thyroid hormone replacement medication.
Nutritional Considerations
Certain nutrients directly impact thyroid function and immune regulation. Deficiencies in selenium, zinc, iron, vitamin D, and vitamin B12 commonly occur in Hashimoto's patients and may worsen symptoms or interfere with medication effectiveness.
Testing for nutritional deficiencies makes sense when:
- Symptoms persist despite normalized TSH
- Fatigue remains disproportionate to thyroid levels
- Hair loss or skin problems continue with treatment
- Immune function appears compromised
- Diet quality has been suboptimal
Comprehensive metabolic panels and specific nutrient testing identify correctable deficiencies that complement thyroid hormone replacement. The availability of diverse testing options enables targeted investigation of potential contributing factors beyond basic thyroid function.
Recommended Panel
Complete Thyroid Panel
Save $3Our most comprehensive thyroid panel includes all 5 essential markers: TSH, Free T4, Free T3, Reverse T3, and both thyroid antibodies. Get the complete picture of your thyroid health.
Includes 6 biomarkers
$84
Understanding the distinction between hashimoto vs hypothyroidism fundamentally changes how you approach your thyroid health, from initial diagnosis through long-term management. While both conditions affect thyroid hormone levels, knowing whether autoimmune disease drives your hypothyroidism enables targeted treatment strategies and preventive monitoring for associated conditions. Comprehensive testing that includes antibody markers provides the diagnostic clarity necessary for personalized care. Justlabs makes accessing complete thyroid panels simple and affordable, with results available in 1-3 days so you can take informed action quickly. Whether you're seeking initial diagnosis or monitoring treatment effectiveness, direct laboratory access puts you in control of your thyroid health journey.