GLP-1 medications have revolutionized diabetes management and weight loss treatment, but their effectiveness and safety depend on proper medical surveillance. Understanding which laboratory assessments to complete and when to schedule them helps patients maximize therapeutic benefits while minimizing potential complications. A glp1 monitoring blood test encompasses multiple biomarkers that track medication response, organ function, and metabolic changes throughout your treatment journey.
Understanding GLP-1 Medications and Laboratory Monitoring
GLP-1 receptor agonists work by mimicking the naturally occurring glucagon-like peptide-1 hormone that regulates blood sugar levels, appetite, and digestion. These medications include semaglutide (Ozempic, Wegovy), tirzepatide (Mounjaro, Zepbound), liraglutide (Victoza, Saxenda), and dulaglutide (Trulicity).
When you start these treatments, your healthcare provider needs baseline data to compare against future results. This initial glp1 monitoring blood test establishes your starting point and identifies any pre-existing conditions that might affect treatment decisions.
Why Regular Monitoring Matters
Laboratory surveillance serves multiple critical functions throughout GLP-1 therapy. First, it confirms the medication is working by tracking blood sugar improvements and metabolic changes. Second, it detects potential side effects before they become serious health concerns. Third, it guides dosage adjustments based on your individual response.
The comprehensive monitoring protocols for GLP-1 patients ensure that clinicians can intervene promptly if complications arise. Without consistent laboratory assessments, subtle changes in kidney function, liver enzymes, or lipid profiles might go unnoticed until they cause significant problems.
Core Components of a GLP-1 Monitoring Blood Test
Multiple laboratory panels work together to provide a complete picture of your health while taking GLP-1 medications. Each component serves a specific monitoring purpose and helps identify different potential issues.
Hemoglobin A1C (HbA1C)
This test measures your average blood glucose levels over the past two to three months. For diabetes patients on GLP-1 therapy, A1C monitoring reveals whether the medication is effectively controlling blood sugar.
Testing frequency recommendations:
- Baseline test before starting medication
- Every three months during the first year
- Every six months once blood sugar stabilizes
Target A1C levels typically fall below 7% for most adults with diabetes, though individual goals may vary. Declining A1C values indicate successful treatment response, while stable or rising levels might prompt dosage adjustments or additional interventions.
Comprehensive Metabolic Panel (CMP)
The CMP evaluates kidney function, electrolyte balance, and liver enzymes through a single blood draw. This panel includes creatinine, blood urea nitrogen (BUN), estimated glomerular filtration rate (eGFR), sodium, potassium, chloride, carbon dioxide, glucose, calcium, albumin, total protein, alkaline phosphatase, alanine aminotransferase (ALT), aspartate aminotransferase (AST), and bilirubin.
| Test Component | What It Monitors | Why It Matters for GLP-1 |
|---|---|---|
| Creatinine/eGFR | Kidney filtration rate | GLP-1 medications are processed by kidneys |
| ALT/AST | Liver enzyme levels | Detects liver stress or damage |
| Electrolytes | Sodium, potassium balance | GI side effects can cause imbalances |
| Glucose | Fasting blood sugar | Immediate treatment effectiveness |
According to essential blood tests for GLP-1 medication patients, kidney function monitoring is particularly important because these medications can affect renal performance, especially in patients with pre-existing kidney disease.
Lipid Panel
GLP-1 medications often improve cardiovascular risk factors, making lipid monitoring valuable for tracking these benefits. The lipid panel measures total cholesterol, LDL (low-density lipoprotein), HDL (high-density lipoprotein), and triglycerides.
Many patients experience favorable lipid profile changes within months of starting GLP-1 therapy. Regular testing documents these improvements and helps assess overall cardiovascular health benefits beyond glucose control.
Thyroid Function Tests
Some GLP-1 medications carry warnings about thyroid concerns, particularly medullary thyroid carcinoma. While this risk appears primarily in animal studies, thyroid-stimulating hormone (TSH) testing provides reassurance and early detection capabilities.
Baseline thyroid function testing before starting GLP-1 therapy establishes normal values for comparison. If you develop symptoms like unexplained weight changes (beyond expected medication effects), extreme fatigue, or neck swelling, additional thyroid assessments may be warranted.
Establishing Your Monitoring Schedule
The frequency of glp1 monitoring blood test requirements varies based on individual health status, medication type, dosage, and treatment duration. Understanding when to schedule laboratory work helps you stay compliant with recommended surveillance protocols.
Initial Phase Monitoring
First three months after starting GLP-1 therapy:
- Baseline comprehensive panel before first dose
- Follow-up metabolic panel at 4-6 weeks
- Three-month assessment including A1C, CMP, and lipids
This intensive early monitoring identifies medication intolerance, unexpected metabolic responses, or developing complications quickly. The recommended frequency for laboratory checks when starting GLP-1 therapy emphasizes the importance of this initial surveillance period.
Maintenance Phase Monitoring
Once your condition stabilizes and you tolerate the medication well, testing frequency typically decreases. Most patients transition to quarterly or semi-annual monitoring schedules based on their healthcare provider's recommendations and individual risk factors.
Standard maintenance schedule:
- A1C every 3-6 months
- Comprehensive metabolic panel every 6-12 months
- Lipid panel annually
- Thyroid function annually or as symptoms warrant
Patients with pre-existing kidney disease, liver conditions, or other complicating factors may require more frequent assessments. Your individual monitoring plan should reflect your unique health profile and risk factors.
Special Considerations for GLP-1 Blood Testing
Beyond standard monitoring panels, certain situations require additional laboratory assessments or modified testing approaches during GLP-1 therapy.
Pregnancy and Reproductive Health
Women of childbearing age should discuss pregnancy testing and family planning before starting GLP-1 medications. Most GLP-1 receptor agonists are not recommended during pregnancy, making pregnancy test screening important for some patients.
If you're planning pregnancy, your healthcare provider will likely recommend discontinuing GLP-1 therapy and may order beta-hCG blood tests to confirm pregnancy status before making medication adjustments.
Pancreatic Function Monitoring
While uncommon, GLP-1 medications have been associated with pancreatitis in some patients. If you experience severe abdominal pain, nausea, or vomiting, your provider may order additional tests including:
- Lipase levels
- Amylase levels
- Complete blood count (CBC)
These assessments help differentiate between common GI side effects and potentially serious pancreatic inflammation requiring immediate intervention.
Vitamin and Nutrient Status
Significant weight loss and reduced food intake can affect nutrient absorption and vitamin levels. Some practitioners recommend periodic assessment of:
- Vitamin B12
- Vitamin D
- Iron studies
- Folate
Nutritional deficiencies can develop gradually, making preventive monitoring valuable for patients experiencing substantial dietary changes while taking GLP-1 medications.
Accessing Affordable GLP-1 Monitoring Testing
Regular laboratory surveillance represents an ongoing cost throughout GLP-1 therapy. For patients without insurance coverage or those facing high deductibles, finding affordable testing options becomes essential for maintaining proper monitoring compliance.
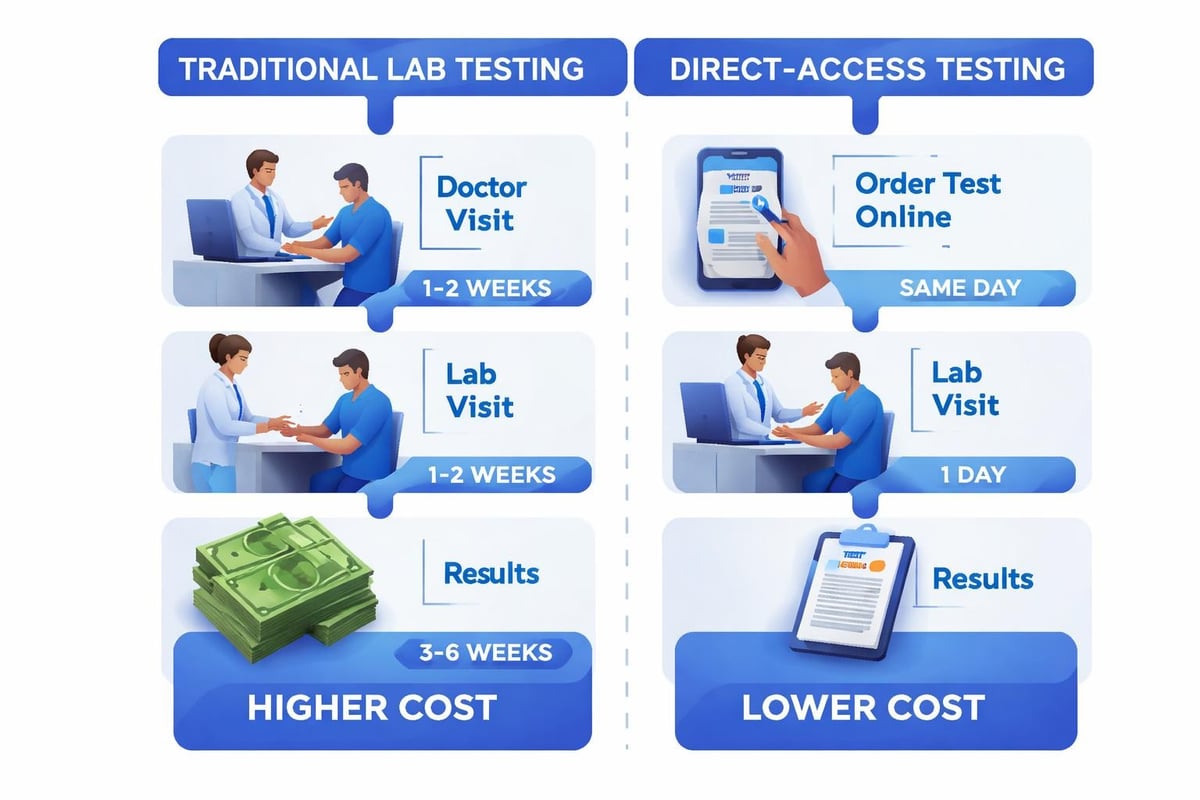
Direct-Access Laboratory Services
Self-pay lab testing services allow patients to order necessary tests directly without requiring a doctor's visit for each laboratory order. This approach reduces overall healthcare costs while maintaining essential medical surveillance.
The
Recommended Panel
GLP1 Monitoring Panel
Save $2.55 essential blood tests to monitor your health on GLP-1 medications like Ozempic, Wegovy, Mounjaro, and Zepbound. Covers liver function, blood sugar, cholesterol, thyroid, and blood counts — everything your provider wants to see.
Includes 38 biomarkers
$37
Fasting required
provides comprehensive monitoring specifically designed for patients taking GLP-1 medications, bundling essential tests at transparent pricing.
Understanding Test Costs
Traditional healthcare settings often don't disclose laboratory pricing until after tests are completed. This lack of transparency makes budgeting for ongoing monitoring difficult. Understanding lab test pricing before ordering helps patients plan for this recurring healthcare expense.
Typical glp1 monitoring blood test costs without insurance:
| Test Type | Traditional Lab Pricing | Direct-Access Pricing |
|---|---|---|
| Hemoglobin A1C | $85-150 | $25-45 |
| Comprehensive Metabolic Panel | $120-200 | $35-65 |
| Lipid Panel | $75-125 | $25-50 |
| TSH (Thyroid) | $80-140 | $30-55 |
Direct-access laboratory services typically offer significantly lower prices compared to hospital-based or traditional reference laboratories, making consistent monitoring more financially sustainable for self-pay patients.
Insurance Alternatives and Payment Options
Many patients don't realize that FSA and HSA funds are eligible for laboratory testing, providing a tax-advantaged way to pay for ongoing GLP-1 monitoring. These health savings accounts can significantly reduce the actual cost of maintaining proper medical surveillance throughout treatment.
For patients who need to bypass insurance entirely, understanding where to get lab tests without insurance involvement streamlines the process and often results in lower out-of-pocket costs than filing insurance claims with high deductibles.
Interpreting Your GLP-1 Monitoring Results
Understanding what your laboratory values mean helps you actively participate in treatment decisions and recognize when follow-up is necessary. While your healthcare provider provides official interpretation, knowing the basics empowers informed health management.
Normal Ranges and Treatment Goals
Reference ranges vary slightly between laboratories, but general targets for patients on GLP-1 therapy include:
Glycemic control markers:
- Fasting glucose: 70-100 mg/dL (optimal)
- Hemoglobin A1C: Below 7% for most diabetes patients
- Postprandial glucose: Below 140 mg/dL two hours after meals
Kidney function markers:
- Creatinine: 0.7-1.3 mg/dL (varies by sex and muscle mass)
- eGFR: Above 60 mL/min/1.73m² (normal function)
- BUN: 7-20 mg/dL
Liver function markers:
- ALT: 7-56 units/L
- AST: 10-40 units/L
- Alkaline phosphatase: 44-147 units/L
Research on GLP-1 medication effects on monitoring systems confirms that these therapies don't interfere with blood glucose monitoring accuracy, ensuring reliable test results throughout treatment.
When Results Indicate Concerns
Certain laboratory findings warrant prompt follow-up or treatment modifications. Contact your healthcare provider if monitoring reveals:
- Rising creatinine or declining eGFR (kidney function decline)
- Significantly elevated liver enzymes (more than twice normal range)
- Persistent hyperglycemia despite medication adherence
- Dramatic lipase or amylase elevation (potential pancreatitis)
- Abnormal thyroid function with concerning symptoms
Early intervention based on laboratory trends prevents minor issues from becoming serious complications. Don't wait for scheduled appointments if results show concerning changes.
Tracking Progress Over Time
Maintaining personal records of your laboratory results helps you visualize treatment effectiveness and identify patterns. Many patients create simple spreadsheets or use health apps to track key values across multiple testing dates.
Longitudinal data reveals whether improvements are sustained, plateauing, or declining. This information supports productive discussions with your healthcare provider about continuing current treatment, adjusting dosages, or considering supplementary interventions.
Preparing for Your GLP-1 Monitoring Blood Test
Proper test preparation ensures accurate results that truly reflect your health status. Following preparation guidelines prevents the need for repeat testing and provides reliable data for treatment decisions.
Fasting Requirements
Most glp1 monitoring blood test panels require fasting for 8-12 hours before the blood draw. This means:
- No food after midnight if testing in the morning
- Only water is permitted during the fasting period
- Continue taking GLP-1 medication as prescribed unless specifically instructed otherwise
- Avoid exercise immediately before testing
Fasting provides standardized conditions for glucose and lipid measurements, eliminating dietary influences that might skew results. If you're unsure about fasting requirements for your specific test panel, detailed testing information clarifies preparation needs.
Medication Timing Considerations
Generally, you should continue your GLP-1 medication on schedule before laboratory testing. However, specific timing questions should be directed to your healthcare provider. Some considerations include:
- Weekly GLP-1 injections: Testing can occur on any day
- Daily GLP-1 medications: Maintain consistent dosing schedule
- Other diabetes medications: Follow provider instructions for test day
The monitoring requirements for patients on GLP-1 treatment recommend maintaining medication consistency to assess real-world treatment effectiveness rather than artificially altered conditions.
Hydration and Timing
Adequate hydration improves blood draw success and may affect certain test results. Drink plenty of water the day before and morning of your test (water doesn't break your fast). Well-hydrated veins are easier to access, reducing discomfort and failed draw attempts.
Schedule your glp1 monitoring blood test early in the morning when possible. This minimizes fasting duration discomfort and ensures you can eat soon after the blood draw. Many laboratory locations offer early morning hours specifically to accommodate fasting patients.
Long-Term Monitoring and Medication Adjustments
As you continue GLP-1 therapy long-term, your monitoring needs may evolve based on treatment response, changing health conditions, and developing risk factors.
Dose Titration and Laboratory Response
Most GLP-1 medications follow gradual dose escalation protocols, starting at lower doses and increasing over weeks or months. Laboratory monitoring during titration helps determine optimal dosing for your individual needs.
If A1C improvements plateau before reaching therapeutic goals, providers may recommend dose increases. Conversely, if you experience significant side effects with normal laboratory values, dose reductions might be appropriate despite adequate glucose control.
Monitoring Medication Efficacy Over Time
Some patients experience diminished medication response after extended use, requiring laboratory surveillance to detect this phenomenon. If glucose control deteriorates despite medication adherence, comprehensive testing helps identify whether:
- The medication is losing effectiveness
- Other health changes are interfering with treatment
- Additional interventions are needed
- Alternative medications should be considered
Regular glp1 monitoring blood test completion provides the objective data necessary for these important treatment decisions.
Transitioning or Discontinuing Therapy
If you eventually discontinue GLP-1 medication, additional monitoring becomes important. Blood sugar levels may rise after stopping therapy, requiring close surveillance during the transition period. Some patients need:
- More frequent glucose monitoring for 1-3 months
- Assessment for alternative diabetes management strategies
- Lipid panel follow-up to track metabolic changes
- Weight and metabolic parameter surveillance
Your healthcare provider will recommend an appropriate post-discontinuation monitoring schedule based on your individual circumstances and reasons for stopping therapy.
Combining GLP-1 Monitoring with Comprehensive Health Assessments
While focused GLP-1 surveillance is essential, integrating these tests with broader health maintenance creates a more complete wellness picture. Consider coordinating your glp1 monitoring blood test with other recommended screenings.
Annual Wellness Integration
Many adults benefit from annual comprehensive health assessments that include:
- Complete blood count (CBC)
- Comprehensive metabolic panel
- Lipid panel
- A1C (for diabetes patients)
- Thyroid function
- Vitamin D levels
- Urinalysis
Bundling GLP-1 monitoring with these routine assessments reduces the total number of laboratory visits required annually. The comprehensive test menu available through direct-access services allows patients to customize panels based on individual needs.
Cardiovascular Risk Assessment
GLP-1 medications provide cardiovascular benefits beyond glucose control. Enhanced cardiovascular monitoring might include:
- High-sensitivity C-reactive protein (hs-CRP)
- Lipoprotein(a)
- Homocysteine
- Advanced lipid particles
These additional markers provide deeper insight into cardiovascular health and help quantify risk reduction achieved through GLP-1 therapy combined with lifestyle modifications.
Regular glp1 monitoring blood test completion ensures safe, effective treatment while catching potential complications early. Understanding which tests you need, when to schedule them, and how to interpret results empowers active participation in your healthcare journey. Justlabs makes essential GLP-1 monitoring accessible and affordable by offering transparent pricing, convenient online ordering, and rapid result delivery-typically within 1-3 days-without requiring insurance or doctor visits for each test order.