Understanding your metabolic health requires measuring the right biomarkers at the right time. When it comes to assessing diabetes risk and insulin resistance, two tests frequently come up in conversation: fasting insulin and fasting glucose. While these tests may sound similar and both require an overnight fast, they measure fundamentally different aspects of your metabolism and provide distinct insights into your health. Knowing when to order each test can help you make informed decisions about your wellness journey and catch potential metabolic issues before they progress into serious conditions.
What Fasting Glucose Measures
Fasting glucose is the more commonly known test of the two. This biomarker measures the concentration of sugar in your bloodstream after you've abstained from food and caloric beverages for at least eight hours.
Your body maintains blood sugar levels within a narrow range through a complex regulatory system. When you eat, glucose enters your bloodstream, and your pancreas releases insulin to help cells absorb this sugar for energy or storage. Between meals and during sleep, your liver releases stored glucose to maintain steady blood sugar levels.
A fasting glucose test reveals:
- Current blood sugar control
- How well your body maintains glucose during periods without food
- Potential diabetes or prediabetes based on established diagnostic criteria
- Short-term glucose regulation patterns
The standard reference ranges for fasting glucose include normal (below 100 mg/dL), prediabetes (100-125 mg/dL), and diabetes (126 mg/dL or higher on two separate tests). According to information on impaired fasting glucose, elevated levels indicate your body is struggling to regulate blood sugar effectively.

When Fasting Glucose Becomes Elevated
Blood sugar rises above normal ranges when your cells become less responsive to insulin or when your pancreas cannot produce enough insulin to meet demand. This test has been the gold standard for diabetes screening for decades because elevated fasting glucose directly indicates impaired glucose metabolism.
However, fasting glucose represents just one piece of the metabolic puzzle. Blood sugar can remain normal for years even as underlying insulin resistance develops, which is where fasting insulin testing becomes valuable.
What Fasting Insulin Measures
Fasting insulin measures the amount of insulin hormone circulating in your blood after an overnight fast. Unlike glucose, which represents the fuel in your system, insulin represents your body's effort to manage that fuel.
When cells become resistant to insulin's signals, your pancreas compensates by producing more insulin to achieve the same glucose-lowering effect. This condition, known as hyperinsulinemia, often develops years before blood sugar levels rise into the diabetic range.
Fasting insulin reveals:
- How hard your pancreas is working to maintain normal glucose
- Early-stage insulin resistance before glucose becomes elevated
- Cardiovascular disease risk independent of glucose levels
- Hormonal imbalances related to metabolic syndrome
Normal fasting insulin typically ranges from 2 to 20 μIU/mL, though optimal levels for metabolic health are generally considered to be below 10 μIU/mL. Research published in the Journal of Clinical Endocrinology & Metabolism demonstrates how insulin resistance affects metabolism at the cellular level, including brain glucose utilization.
Key Differences Between Fasting Insulin vs Fasting Glucose
Understanding the distinction between these two tests helps you determine which provides the information you need for your specific health concerns.
| Characteristic | Fasting Glucose | Fasting Insulin |
|---|---|---|
| What it measures | Sugar in bloodstream | Insulin hormone in bloodstream |
| Primary use | Diabetes diagnosis | Insulin resistance detection |
| Detection timing | Later stage metabolic dysfunction | Early stage metabolic dysfunction |
| Standard screening | Yes, widely used | No, more specialized |
| Insurance coverage | Typically covered | Often not covered |
| Interpretation | Well-established ranges | Context-dependent analysis |
The timing difference is particularly important. Studies like this research on young adults show that fasting insulin can predict type 2 diabetes risk years before fasting glucose becomes abnormal, making it a valuable early warning system.
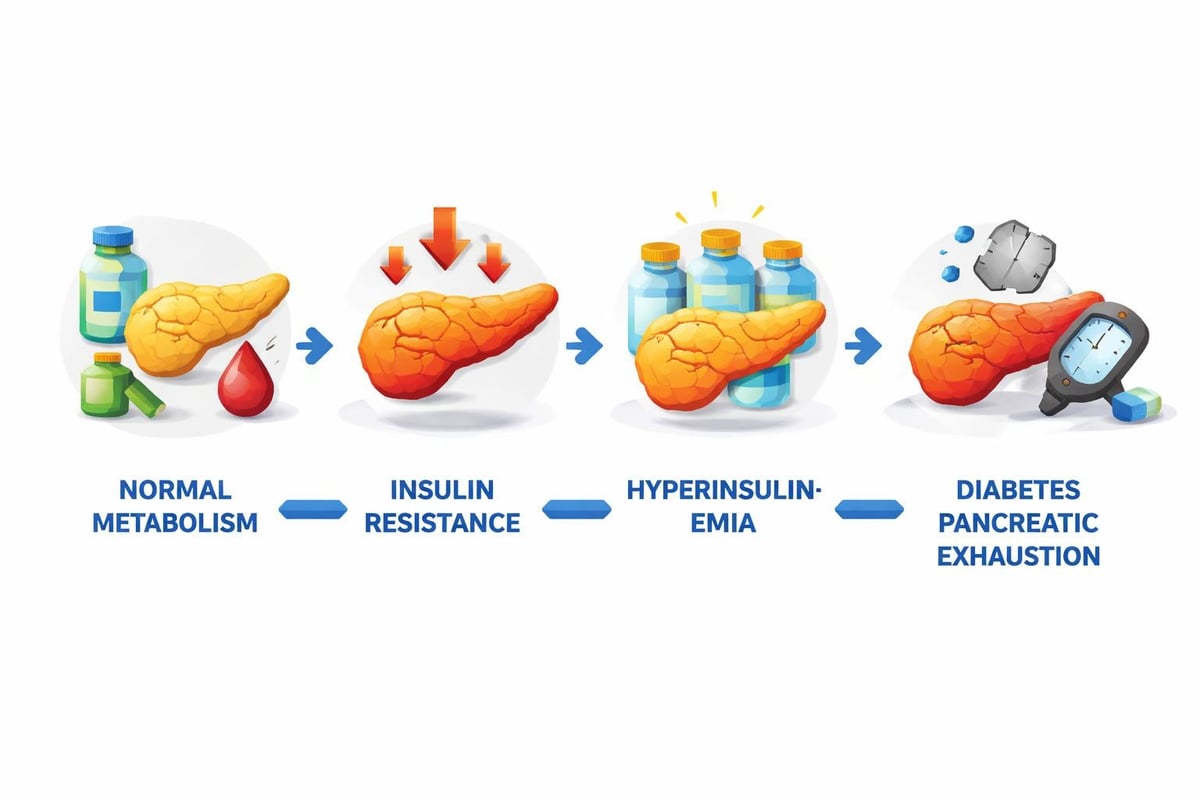
The Cascade of Metabolic Dysfunction
Metabolic disease typically follows a predictable progression. First, cells become less sensitive to insulin signals. Second, the pancreas increases insulin output to compensate. Third, despite higher insulin levels, glucose begins to rise. Fourth, the pancreas eventually cannot keep up with demand.
Fasting insulin catches problems at stage two. Your glucose might still look perfect at 85 mg/dL, but if your insulin is 25 μIU/mL, your body is working overtime to maintain that normal glucose. Fasting glucose catches problems at stage three or four when the damage is more advanced and harder to reverse.
Recommended Panel
Insulin Resitance Panel
Save $1.5A focused panel to detect early insulin resistance and metabolic dysfunction before blood sugar levels become abnormal.
Includes 21 biomarkers
$45
Fasting required
Using Glucose-to-Insulin Ratios
Many practitioners don't evaluate fasting insulin or glucose in isolation. Instead, they calculate ratios that provide additional context about insulin sensitivity and metabolic health.
The fasting glucose-to-insulin ratio offers insights into how efficiently your body manages blood sugar. Studies on prepubertal girls with premature adrenarche and research on glucose tolerance prediction demonstrate the clinical utility of these ratios in assessing insulin resistance.
Calculating and Interpreting the Ratio
To calculate this ratio, divide your fasting glucose (in mg/dL) by your fasting insulin (in μIU/mL). Some practitioners multiply the result by a conversion factor for standardization.
- Ratio above 7: Generally indicates good insulin sensitivity
- Ratio between 4.5-7: Suggests early insulin resistance
- Ratio below 4.5: Indicates significant insulin resistance
A person with fasting glucose of 90 mg/dL and fasting insulin of 5 μIU/mL would have a ratio of 18, suggesting excellent insulin sensitivity. Conversely, someone with glucose of 95 mg/dL and insulin of 20 μIU/mL would have a ratio of 4.75, indicating insulin resistance despite normal glucose.
Who Should Test Fasting Insulin vs Fasting Glucose
The question isn't necessarily which test is better, but rather which test answers your specific health questions. Different situations call for different testing strategies.
Candidates for Fasting Glucose Testing
Everyone should monitor fasting glucose periodically as part of routine health maintenance. This test serves as a fundamental screening tool for diabetes and prediabetes.
Priority groups include:
- Adults over 45 years old
- People with BMI over 25 with additional risk factors
- Individuals with family history of diabetes
- Women with history of gestational diabetes
- People with diagnosed prediabetes requiring monitoring
Most routine annual physicals include fasting glucose, and guidelines recommend regular screening starting in middle age. If you're ordering labs without insurance, fasting glucose is typically affordable and provides essential baseline information.
Candidates for Fasting Insulin Testing
Fasting insulin testing targets people seeking early detection of metabolic problems before glucose becomes abnormal. This proactive approach can identify issues when lifestyle interventions are most effective.
According to guidance on who should undergo fasting insulin testing, priority candidates include:
- People with stubborn weight gain despite reasonable diet and exercise
- Individuals with family history of diabetes or metabolic syndrome
- Women with PCOS or other hormonal imbalances
- Anyone with cardiovascular risk factors like high triglycerides or low HDL
- People with normal glucose but metabolic symptoms like fatigue or brain fog
Fasting insulin often requires specific ordering since it's not included in standard panels. When you order labs without a doctor, you can select this specialized test based on your individual risk profile and health goals.
Interpreting Results in Context
Neither fasting insulin nor fasting glucose exists in a vacuum. Proper interpretation requires considering both markers alongside other health data.

Four Common Metabolic Scenarios
| Fasting Glucose | Fasting Insulin | Interpretation | Action Needed |
|---|---|---|---|
| Normal | Normal | Healthy metabolism | Maintain current habits |
| Normal | Elevated | Early insulin resistance | Lifestyle intervention crucial |
| Elevated | Elevated | Advanced insulin resistance | Aggressive intervention needed |
| Elevated | Normal/Low | Pancreatic exhaustion | Medical management likely required |
The second scenario-normal glucose with elevated insulin-represents the sweet spot for preventive intervention. Your body is still compensating successfully, but the warning signs are clear. This stage responds particularly well to dietary changes, exercise, and stress management.
Recommended Panel
Comprehensive Diabetes Panel
This panel detects diabetes and prediabetes at every stage. Includes lipids because diabetes dramatically increases heart disease risk.
Includes 9 biomarkers
$35
Fasting required
Additional Markers to Consider
Comprehensive metabolic assessment often includes:
- Hemoglobin A1c: Three-month average glucose levels
- Lipid panel: Triglycerides and HDL cholesterol patterns
- Liver enzymes: Indicators of fatty liver disease
- C-peptide: Measure of insulin production capacity
- HOMA-IR score: Calculated insulin resistance index
Resources like this comparison of fasting glucose versus insulin provide additional context for understanding how these biomarkers work together to paint a complete picture of metabolic health.
Practical Considerations for Testing
Both tests require proper preparation to ensure accurate results. The quality of your data depends on following pre-test protocols carefully.
Preparation Requirements
For both fasting insulin and fasting glucose:
- Fast for 8-12 hours before blood draw (water is allowed)
- Avoid strenuous exercise the night before
- Maintain consistent medication schedule unless directed otherwise
- Get adequate sleep the night before testing
- Schedule morning appointments when possible
Timing matters because insulin and glucose levels fluctuate throughout the day in response to circadian rhythms, meals, and physical activity. Morning fasting tests provide the most standardized and comparable results.
Cost and Accessibility Differences
Fasting glucose is typically inexpensive and widely available. Most insurance plans cover this test as preventive care, and self-pay pricing through services offering transparent lab test pricing remains affordable.
Fasting insulin costs more and may not be covered by insurance, particularly when ordered for screening rather than diagnosis. However, the investment in early detection can prevent far greater healthcare costs down the road. When you access comprehensive testing through platforms where you can browse available tests, you can compare costs and make informed decisions about which biomarkers provide the most value for your situation.
Frequency of Testing
How often you should test fasting insulin vs fasting glucose depends on your current metabolic health status and risk factors.
Fasting glucose screening recommendations:
- Every 3 years for adults with normal results and no risk factors
- Annually for people with prediabetes
- Every 3-6 months during active intervention or treatment
- As directed by healthcare providers for diabetes management
Fasting insulin monitoring guidelines:
- Baseline test for people with metabolic risk factors
- Retest every 6-12 months during lifestyle intervention
- More frequent testing if results are significantly abnormal
- Periodic rechecks even after normalization to detect recurrence
People actively working to reverse insulin resistance through diet, exercise, or medication benefit from seeing objective improvements in their fasting insulin levels, which often drop before other markers show change.
Making the Testing Decision
The choice between fasting insulin and fasting glucose isn't always either/or. Many people benefit from testing both markers to get comprehensive metabolic insights.
Order both tests when:
- You're concerned about metabolic health but have no formal diagnosis
- You want the most complete picture of your glucose metabolism
- You're tracking progress during lifestyle changes
- You have conflicting symptoms and lab results
Order fasting glucose alone when:
- You're doing routine annual screening
- You've been diagnosed with diabetes and monitor regularly
- You have limited budget and need basic information
- Your doctor specifically ordered only glucose testing
Order fasting insulin alone when:
- Your glucose is consistently normal but you have metabolic symptoms
- You're seeking early detection of insulin resistance
- You've already established your glucose patterns
- You're specifically targeting insulin-related interventions
Understanding how lab testing works helps you navigate the process efficiently, whether you're ordering one test or creating a comprehensive metabolic panel.
The Bigger Picture of Metabolic Health
While fasting insulin vs fasting glucose represents an important distinction, neither test tells the complete story of your metabolic health. These biomarkers function as pieces of a larger puzzle that includes body composition, inflammatory markers, hormone balance, cardiovascular health, and lifestyle factors.
The real power comes from tracking trends over time rather than obsessing over single data points. A fasting insulin of 15 μIU/mL might seem concerning in isolation, but if it was 25 μIU/mL six months ago, you're moving in the right direction. Similarly, fasting glucose at the high end of normal deserves attention, but context from other markers determines urgency and intervention strategy.
Modern approaches to metabolic health emphasize prevention through early detection and intervention. By the time fasting glucose reaches diabetic levels, you've already lost significant beta cell function and developed widespread insulin resistance. Testing fasting insulin earlier in the disease process opens a window for intervention when simple lifestyle modifications can make dramatic differences.
Both fasting insulin and fasting glucose provide valuable information about metabolic health, but they measure different aspects of how your body processes energy. Understanding which test answers your specific health questions empowers you to make informed decisions about your wellness journey. Whether you need basic glucose screening or comprehensive metabolic assessment including insulin testing, Justlabs provides affordable, accessible lab testing without insurance hassles or doctor visits, delivering results in 1-3 days so you can take action on your health goals.