Understanding hormones and their impact on overall health requires more than surface-level knowledge. Among the most important yet often overlooked hormones is dehydroepiandrosterone sulfate, commonly known as DHEA-S. This steroid hormone serves as a key biomarker for adrenal gland function and offers valuable insights into various health conditions. As the most abundant circulating steroid hormone in the human body, DHEA-S plays multiple roles in maintaining physiological balance, making it an essential component of comprehensive health assessments.
What Makes DHEA-S Your Adrenal Androgen
DHEA-S represents the sulfated form of dehydroepiandrosterone (DHEA), produced primarily by the adrenal cortex. Unlike other hormones that originate from multiple sources, approximately 95% of circulating DHEA-S comes directly from your adrenal glands, earning it the distinction as your adrenal androgen.
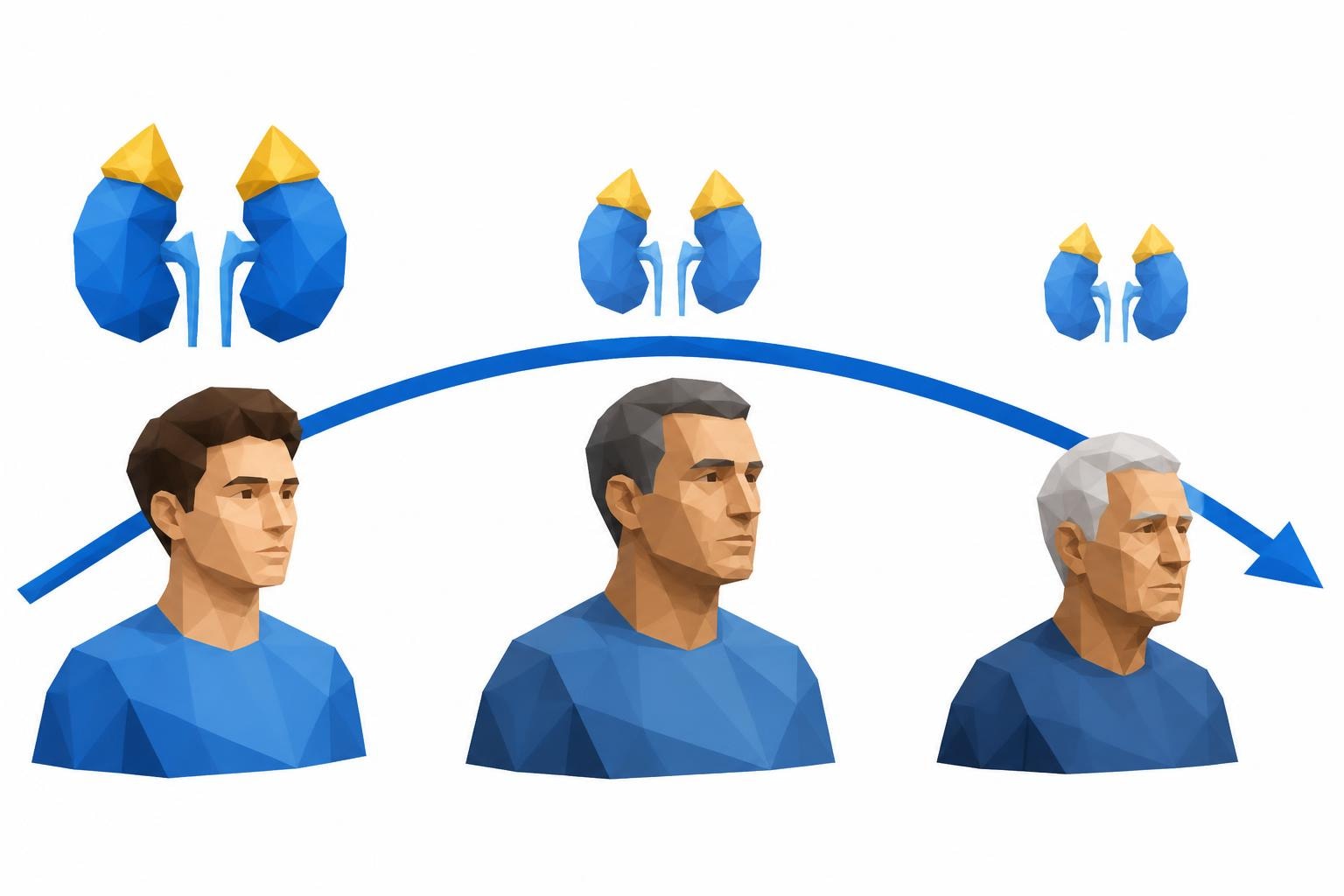
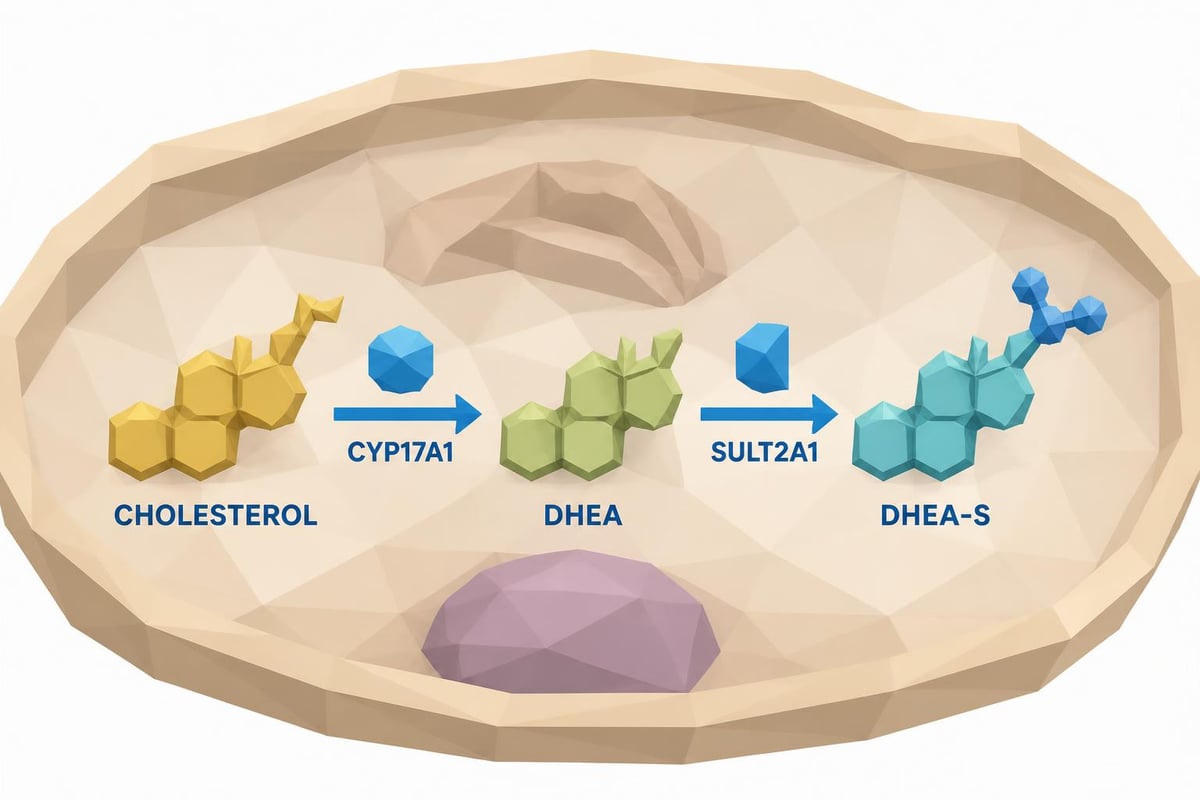
The adrenal glands sit atop each kidney and function as critical endocrine organs. Within the adrenal cortex, specialized cells convert cholesterol into DHEA, which then undergoes sulfation to become DHEA-S. This sulfation process extends the hormone's half-life significantly, making it more stable in the bloodstream and easier to measure accurately through laboratory testing.
The Biochemical Journey
Key characteristics of DHEA-S production:
- Synthesized exclusively in the zona reticularis of the adrenal cortex
- Converted from DHEA through sulfotransferase enzymes
- Maintains a longer half-life (7-10 hours) compared to DHEA (15-30 minutes)
- Exhibits minimal diurnal variation, unlike cortisol
The MedlinePlus DHEA-sulfate test information explains how this stability makes DHEA-S an ideal marker for evaluating adrenal androgen production. Unlike cortisol, which fluctuates throughout the day, DHEA-S levels remain relatively constant, allowing for testing at any time without concerns about circadian rhythm interference.
Understanding Normal DHEA-S Levels Across the Lifespan
DHEA-S your adrenal androgen follows a distinctive pattern throughout human development and aging. Levels change dramatically from birth through old age, reflecting the hormone's role in various life stages.
At birth, DHEA-S concentrations are relatively high due to fetal adrenal production. These levels decline rapidly during the first year of life, reaching a nadir in early childhood. The hormone then begins a gradual increase during adrenarche (typically ages 6-8), marking the awakening of adrenal androgen production.
Peak Production and Decline
| Life Stage | Typical DHEA-S Range (μg/dL) | Characteristics |
|---|---|---|
| Newborn | 100-600 | Inherited from fetal production |
| Childhood (1-6 years) | 5-125 | Lowest levels |
| Adolescence | 65-380 | Rapid increase during puberty |
| Young Adult (20-30 years) | 280-640 (men), 65-380 (women) | Peak production |
| Middle Age (40-50 years) | 120-520 (men), 45-270 (women) | Gradual decline begins |
| Older Adult (60+ years) | 20-290 (men), 10-150 (women) | Significantly reduced |
Peak DHEA-S production occurs during the third decade of life. After age 30, levels decline by approximately 2-3% per year, resulting in a 70-80% reduction by age 70. This predictable decline pattern has led researchers to investigate whether DHEA-S supplementation might counteract aging-related changes, though current research on DHEA presents mixed conclusions about its efficacy.
Clinical Significance of DHEA-S Testing
Testing DHEA-S your adrenal androgen provides diagnostic value across multiple clinical scenarios. Healthcare providers order this test to evaluate adrenal function, investigate symptoms of hormone imbalance, and monitor specific medical conditions.
Primary reasons for DHEA-S testing:
- Evaluating adrenal gland tumors or abnormalities
- Diagnosing polycystic ovary syndrome (PCOS) in women
- Assessing causes of excess androgen production
- Investigating delayed or early puberty
- Monitoring adrenal insufficiency treatment
The DHEA-S test overview outlines how this biomarker helps differentiate between adrenal and ovarian sources of androgens. In women with elevated testosterone levels, measuring DHEA-S helps clinicians determine whether the excess androgens originate from the adrenal glands or the ovaries.
Interpreting Abnormal Results
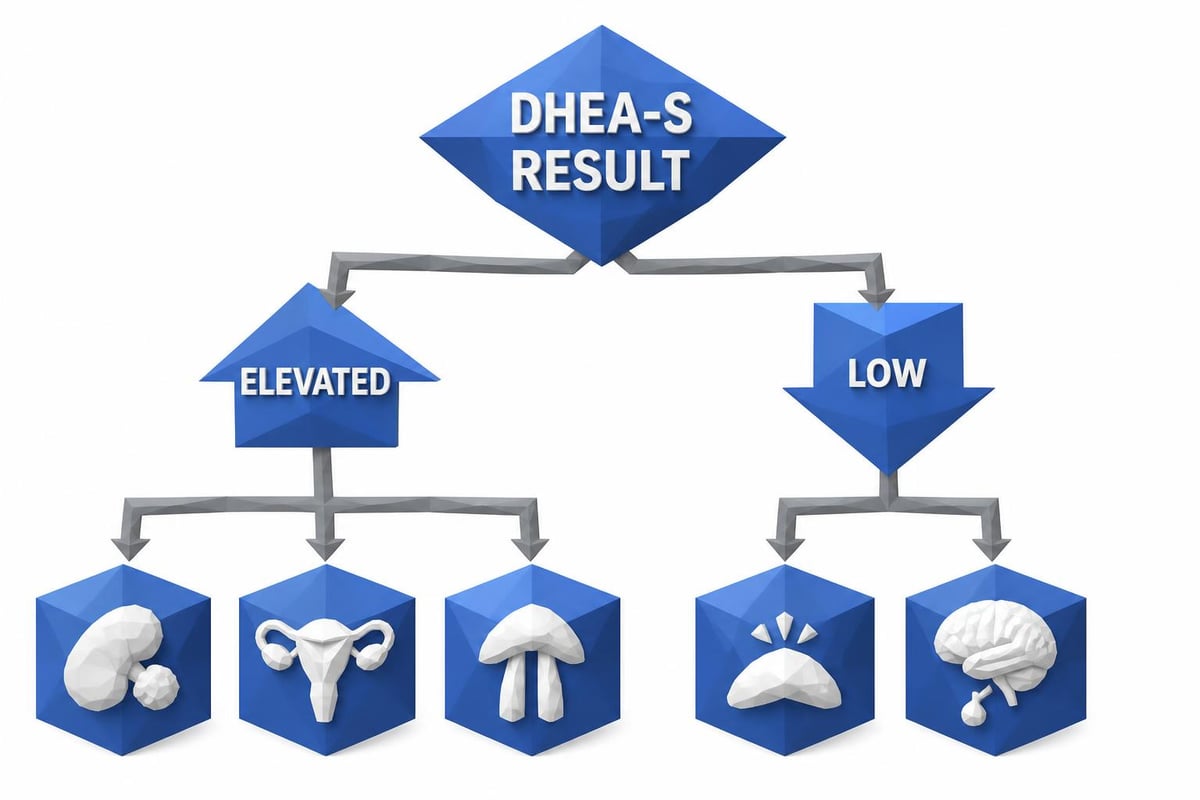
Elevated DHEA-S levels may indicate several conditions. Adrenal tumors, both benign and malignant, can cause overproduction of this hormone. Congenital adrenal hyperplasia, a genetic condition affecting cortisol synthesis, often presents with elevated DHEA-S alongside other hormonal imbalances.
In women, high DHEA-S levels frequently accompany PCOS, contributing to symptoms like irregular periods, excess facial or body hair growth, and difficulty conceiving. The hormone serves as one component of the diagnostic workup, though PCOS diagnosis requires multiple criteria.
Low DHEA-S levels suggest adrenal insufficiency, where the adrenal glands fail to produce adequate amounts of steroid hormones. This condition may result from Addison's disease, hypopituitarism, or chronic corticosteroid use. According to research on DHEA-S as an adrenal function indicator, reduced levels provide valuable diagnostic information when evaluating suspected adrenal dysfunction.
Gender Differences in DHEA-S Production
DHEA-S your adrenal androgen exhibits notable differences between males and females, though both sexes produce this hormone in their adrenal glands. Understanding these variations helps contextualize test results and their clinical implications.
Men typically maintain higher circulating DHEA-S concentrations throughout adulthood compared to women. This difference reflects both production rates and metabolic pathways. While the adrenal glands remain the primary source for both sexes, the downstream conversion of DHEA-S influences overall androgen profiles differently.
Metabolic Pathways by Gender
In men, DHEA-S serves as a minor contributor to total androgen production since the testes generate the majority of testosterone. The adrenal contribution becomes more clinically significant only when testicular function declines or adrenal pathology develops.
For women, DHEA-S plays a more substantial role in overall androgen production. The ovaries produce some androgens, but adrenal androgens, including those derived from DHEA-S, contribute significantly to total circulating testosterone and other androgenic hormones. This makes DHEA-S measurement particularly valuable in evaluating women with symptoms of androgen excess.
Comprehensive reviews of DHEA and DHEA-S demonstrate how age and gender influence concentrations and metabolism. These factors must be considered when interpreting results, as reference ranges differ substantially between demographic groups.
The Role of DHEA-S in Modern Health Assessment
Contemporary medicine increasingly recognizes the importance of measuring DHEA-S your adrenal androgen as part of comprehensive hormone panels. This shift reflects growing understanding of the hormone's multifaceted roles beyond simple androgen precursor functions.
DHEA-S serves as a prohormone, meaning it converts into other active hormones throughout the body. Peripheral tissues can transform DHEA-S into testosterone, estradiol, and other sex steroids through local enzymatic processes. This conversion allows tissues to regulate their own hormonal environment based on specific needs.
Beyond Reproductive Health
Non-reproductive functions influenced by DHEA-S:
- Bone density maintenance and skeletal health
- Immune system modulation and inflammatory responses
- Cardiovascular health and vascular function
- Cognitive function and neuroprotection
- Metabolic regulation and insulin sensitivity
Research documented in Nature Reviews Endocrinology explores how adrenal androgens, including DHEA-S, participate in metabolic processes and disease states. The emerging understanding of 11-oxygenated androgens has revealed additional complexity in adrenal androgen physiology.
Accessing DHEA-S Testing Without Barriers
Traditional healthcare systems often create obstacles to hormone testing. Patients typically need physician referrals, insurance authorization, and multiple appointments before accessing basic laboratory services. These barriers delay diagnosis and increase overall healthcare costs.
Direct-access laboratory testing removes these impediments. Through services that prioritize transparency and convenience, individuals can order comprehensive lab tests without navigating insurance bureaucracy or scheduling multiple doctor visits. This approach proves particularly valuable for monitoring known conditions or investigating symptoms that warrant hormonal evaluation.
The self-pay model offers several advantages. Pricing transparency allows informed decision-making about which tests provide the most value. Eliminating insurance intermediaries often reduces costs while accelerating result delivery. Most direct-access testing services return results within 1-3 days, enabling faster clinical decision-making.
For those concerned about affordability, exploring labs without insurance demonstrates how direct-pay pricing frequently costs less than insurance copays and deductibles for similar testing. This pricing structure makes regular monitoring more accessible for individuals managing chronic conditions or optimizing their health proactively.
Factors That Influence DHEA-S Levels
Beyond age and gender, multiple variables affect DHEA-S your adrenal androgen concentrations. Understanding these factors helps interpret results accurately and identify when additional investigation may be warranted.
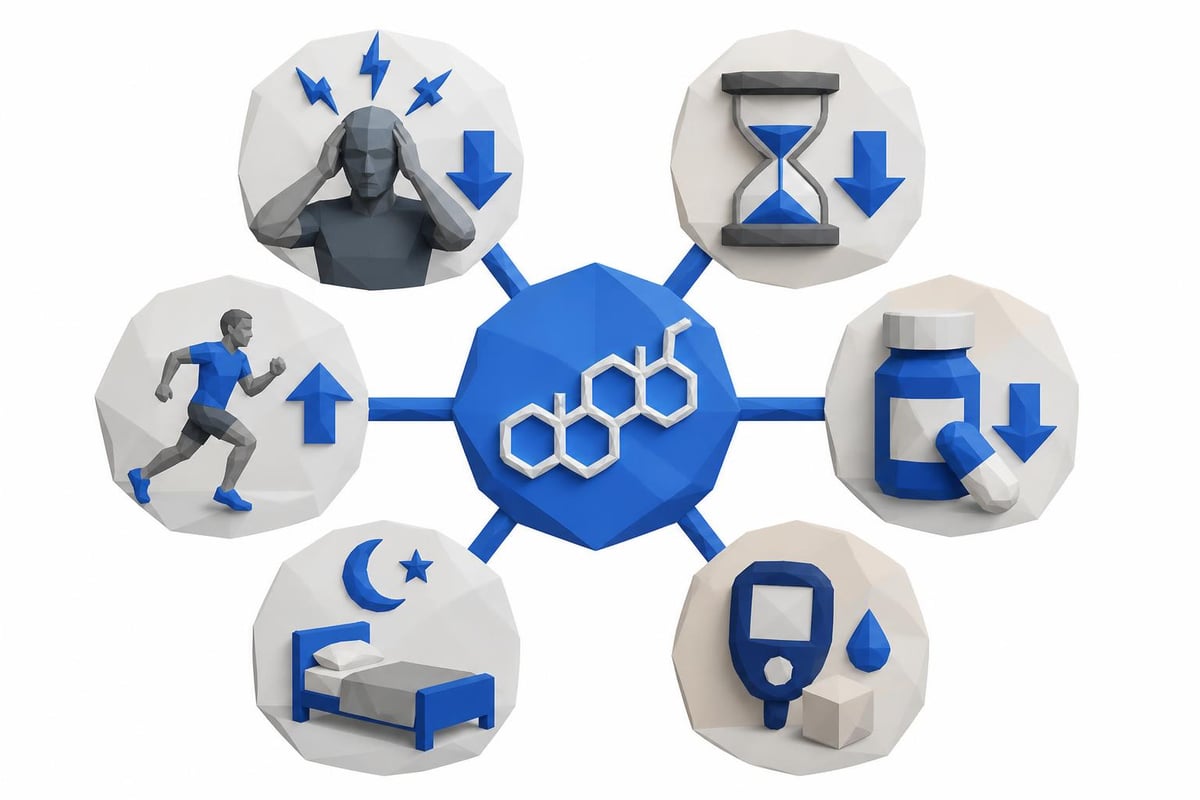
Environmental and lifestyle factors:
- Chronic stress and cortisol dysregulation
- Nutritional status and caloric intake
- Physical activity patterns and exercise intensity
- Sleep quality and circadian rhythm disruption
- Medication use, particularly corticosteroids
Chronic stress presents particular complexity. While acute stress triggers cortisol release, prolonged stress may eventually suppress overall adrenal function, potentially reducing DHEA-S production. The balance between cortisol and DHEA-S provides insights into adrenal reserve and stress adaptation capacity.
Medical Conditions and DHEA-S
| Condition | Typical DHEA-S Pattern | Clinical Relevance |
|---|---|---|
| Adrenal tumors | Significantly elevated | Helps localize source of excess androgens |
| PCOS | Mildly to moderately elevated | Contributes to diagnostic criteria |
| Addison's disease | Markedly reduced | Indicates adrenal insufficiency |
| Cushing's syndrome | Variable, often elevated | Part of comprehensive adrenal workup |
| Premature adrenarche | Elevated for age | Indicates early adrenal activation |
Medications significantly impact DHEA-S measurements. Oral contraceptives, hormone replacement therapy, and glucocorticoids all alter adrenal androgen production or metabolism. Patients should inform testing facilities about all medications to ensure proper result interpretation.
DHEA-S Measurement and Laboratory Considerations
Accurate DHEA-S your adrenal androgen measurement requires appropriate laboratory methodology and quality assurance. Several analytical techniques exist, each with specific advantages and limitations.
Immunoassay methods represent the most common approach for clinical DHEA-S testing. These techniques use antibodies specific to the DHEA-S molecule, providing rapid results suitable for routine clinical use. Modern automated immunoassay platforms deliver excellent precision and accuracy for most clinical applications.
Liquid chromatography-mass spectrometry (LC-MS/MS) offers superior specificity and sensitivity compared to immunoassays. This methodology directly measures DHEA-S molecules rather than relying on antibody binding, reducing potential interference from similar compounds. Reference laboratories increasingly employ LC-MS/MS for hormone testing, particularly when precise quantification proves critical.
Preparing for Testing
DHEA-S testing requires minimal patient preparation. Unlike cortisol or testosterone, which fluctuate throughout the day, DHEA-S levels remain relatively stable. This stability means:
- Testing can occur at any time of day
- Fasting is generally not required
- A single measurement provides reliable information
- Repeat testing can occur at consistent intervals without timing concerns
According to Medscape's DHEA overview, this convenience makes DHEA-S measurement more practical than other adrenal hormones that require timed collection or multiple samples.
Monitoring DHEA-S Over Time
Serial DHEA-S your adrenal androgen measurements provide more information than isolated results. Tracking changes over time helps assess disease progression, treatment response, and age-related patterns.
Individuals with adrenal tumors require regular monitoring after diagnosis and treatment. DHEA-S serves as a tumor marker in cases where adrenal adenomas or carcinomas produce excess androgens. Declining levels after surgical removal confirm successful treatment, while rising levels may indicate recurrence.
Women managing PCOS often benefit from periodic DHEA-S testing alongside other hormonal markers. While treatment focuses primarily on metabolic and reproductive symptoms, monitoring androgen levels helps assess therapeutic effectiveness and guide medication adjustments.
Recommended testing frequency varies by indication:
- Adrenal tumor surveillance: Every 3-6 months initially, then annually if stable
- PCOS management: Every 6-12 months or when symptoms change
- Adrenal insufficiency treatment: Annually or as clinically indicated
- General health optimization: Every 1-2 years for baseline tracking
The detailed review from University of Minnesota experts emphasizes how longitudinal data provides context that single measurements cannot offer. Individual variation means that what constitutes normal for one person may differ from population averages, making personal trends particularly informative.
The Future of DHEA-S Research and Clinical Application
Scientific understanding of DHEA-S your adrenal androgen continues evolving. Current research investigates potential therapeutic applications, refines reference ranges for specific populations, and explores relationships between DHEA-S and various disease states.
Researchers are particularly interested in the age-related decline of DHEA-S and whether this reduction contributes to aging-associated health changes. Some studies suggest associations between higher DHEA-S levels and better cognitive function, bone density, and immune response in older adults, though causation remains unproven.
The relationship between DHEA-S and cardiovascular health represents another active research area. Some evidence suggests protective effects against atherosclerosis and cardiovascular events, while other studies find no significant association. These conflicting results highlight the complexity of hormone-disease relationships and the need for continued investigation.
Metabolic syndrome and insulin resistance show interesting correlations with DHEA-S levels. Lower concentrations associate with increased metabolic risk in some populations, raising questions about whether DHEA-S plays a protective metabolic role or simply reflects overall health status.
Understanding how to access reliable testing becomes increasingly important as research expands. Learning how testing works helps individuals make informed decisions about when hormone evaluation might provide valuable health insights.
DHEA-S your adrenal androgen serves as a critical biomarker for adrenal function, hormone balance, and various health conditions. Understanding this hormone's patterns across age, gender, and disease states empowers better health decisions and more targeted medical investigations. When you need convenient, affordable access to hormone testing without the complexity of insurance authorization and physician referrals, Justlabs provides direct-to-consumer laboratory services with transparent pricing and rapid results delivery. Take control of your health monitoring by ordering the tests you need when you need them.