Understanding your metabolic health requires more than just checking blood sugar levels. When doctors need to determine how well your pancreas produces insulin or distinguish between different types of diabetes, they turn to c-peptide testing. This diagnostic tool provides critical insights that standard glucose and insulin tests simply cannot deliver, making it an essential component of diabetes management and diagnosis. Whether you're newly diagnosed with diabetes, experiencing unexplained hypoglycemia, or managing an existing condition, understanding c-peptide can empower you to make informed decisions about your health care.
What Is C-Peptide and Why Does It Matter
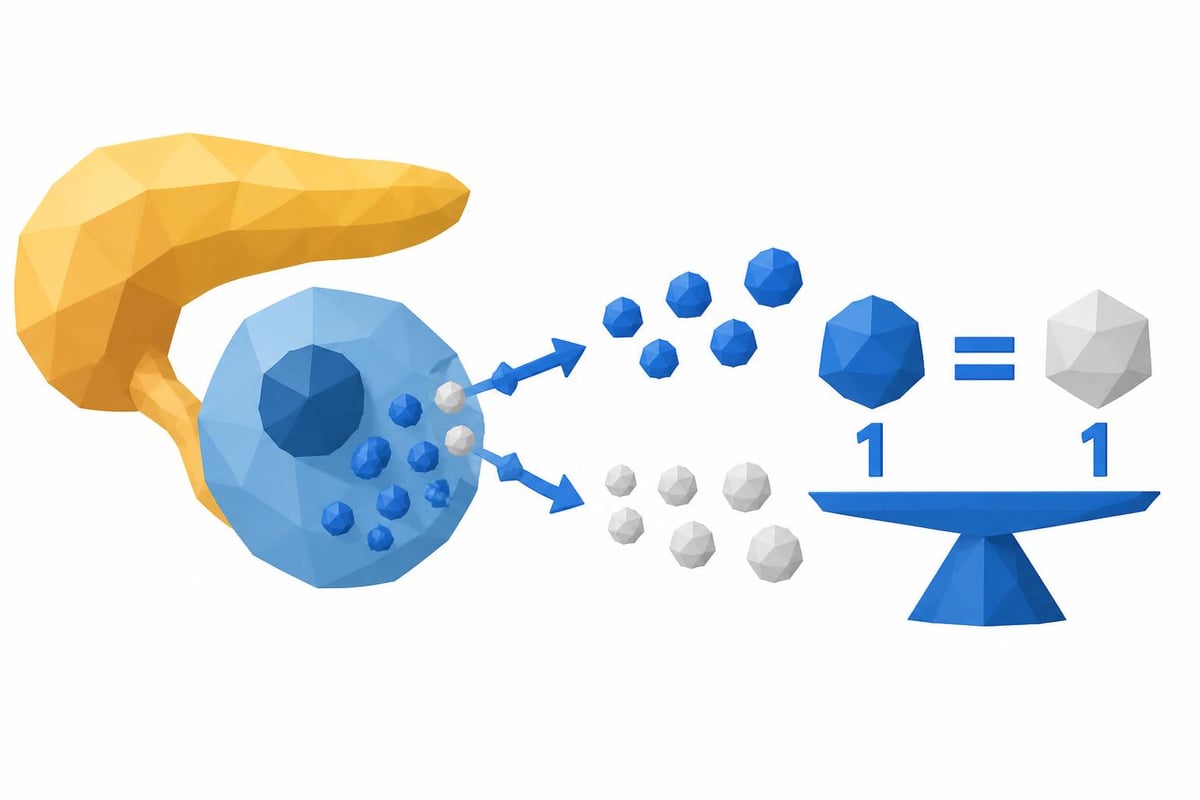
C-peptide, short for "connecting peptide," is a protein fragment produced when your pancreas manufactures insulin. Every time your pancreatic beta cells create an insulin molecule, they produce an equal amount of c-peptide. Think of insulin as a two-part molecule connected by a bridge. That bridge is c-peptide, which gets cleaved off and released into your bloodstream alongside the active insulin hormone.
The biochemistry of c-peptide reveals why this molecule serves as such a valuable diagnostic marker. Unlike insulin, which gets rapidly absorbed by the liver during its first pass through the body, c-peptide remains in circulation much longer. This stability makes it a more reliable indicator of how much insulin your body actually produces.
The Science Behind C-Peptide Measurement
When your pancreas creates insulin, it starts with a precursor molecule called proinsulin. This larger protein contains three components: the A-chain and B-chain of insulin, connected by c-peptide. During the final stages of insulin production, enzymes split proinsulin into active insulin and c-peptide in a 1:1 ratio.
Key characteristics of c-peptide include:
- Longer half-life than insulin (approximately 30 minutes versus 5 minutes)
- Minimal liver metabolism during first-pass circulation
- Direct reflection of pancreatic beta-cell function
- Stability that makes testing more reliable across different conditions
This stability matters tremendously in clinical practice. Insulin measurements can be skewed by liver function, insulin resistance, or external insulin injections. C-peptide levels, however, provide an accurate snapshot of your pancreas's actual insulin production capacity regardless of these variables.
When You Need C-Peptide Testing
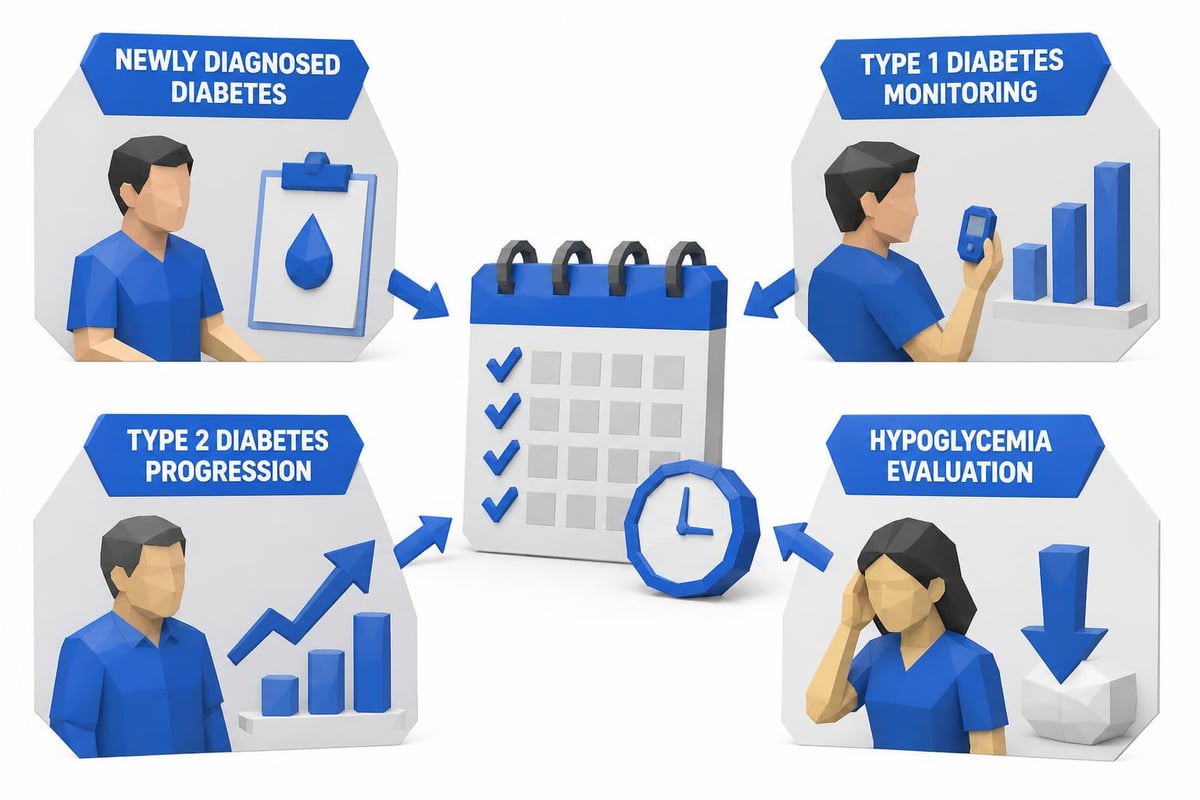
According to clinical guidelines for c-peptide assessment, several scenarios warrant this specialized testing. The most common reason involves determining what type of diabetes a person has, particularly when the diagnosis isn't immediately clear from symptoms alone.
Differentiating Diabetes Types
The primary application of c-peptide testing centers on distinguishing Type 1 from Type 2 diabetes. In Type 1 diabetes, your immune system attacks and destroys the insulin-producing beta cells in your pancreas. This results in little to no c-peptide production. Conversely, Type 2 diabetes typically involves insulin resistance rather than complete loss of insulin production, meaning c-peptide levels remain normal or even elevated as your pancreas works harder to overcome that resistance.
Testing scenarios include:
- Adults diagnosed with diabetes who don't fit typical patterns
- Children or young adults where diabetes type isn't clear
- People with diabetes who don't respond as expected to treatment
- Patients who might have latent autoimmune diabetes in adults (LADA)
- Monitoring beta-cell function over time in diabetes patients
The c-peptide test becomes especially valuable when someone presents with diabetes but doesn't fit the typical profile for either type. For instance, an overweight adult might be assumed to have Type 2 diabetes, but low c-peptide levels would reveal Type 1 diabetes requiring immediate insulin therapy.
Investigating Hypoglycemia
Beyond diabetes classification, c-peptide testing plays a crucial role in evaluating unexplained low blood sugar episodes. If you experience hypoglycemia without a clear cause, measuring c-peptide during a low blood sugar episode can reveal whether your pancreas is inappropriately producing too much insulin.
| Condition | C-Peptide Level | Insulin Level | Clinical Significance |
|---|---|---|---|
| Insulinoma | High | High | Tumor producing excess insulin |
| External insulin use | Low | High | Synthetic insulin administration |
| Type 1 diabetes | Low | Low | Insufficient beta-cell function |
| Type 2 diabetes (early) | Normal to High | High | Insulin resistance present |
Understanding Your C-Peptide Test Results
When you receive c-peptide test results, the numbers need context. Normal fasting c-peptide levels typically range from 0.5 to 2.0 ng/mL, though reference ranges may vary slightly between laboratories. More important than the absolute number is what it reveals about your pancreatic function.
Interpreting Low C-Peptide Levels
Low c-peptide indicates reduced insulin production by your pancreas. This finding strongly suggests Type 1 diabetes, advanced Type 2 diabetes with beta-cell failure, or pancreatic damage from other causes. If you're taking insulin and have low c-peptide levels, it confirms your pancreas isn't producing adequate insulin on its own.
As explained by WebMD's c-peptide overview, low levels typically mean your body cannot produce enough insulin naturally, necessitating insulin therapy rather than oral medications alone. This distinction fundamentally changes treatment approaches and long-term management strategies.
Interpreting High C-Peptide Levels
Elevated c-peptide suggests your pancreas is working overtime to produce insulin. This pattern commonly appears in early Type 2 diabetes when insulin resistance forces your pancreas to compensate by producing more insulin. High levels might also indicate an insulinoma, a rare tumor that produces excess insulin.
Factors affecting c-peptide levels:
- Recent food intake (levels rise after meals)
- Kidney function (reduced clearance increases levels)
- Medications affecting insulin secretion
- Stress and illness
- Time of day (diurnal variation exists)

The C-Peptide Testing Process
Getting a c-peptide test through services like Justlabs involves a straightforward blood draw, but timing and preparation matter significantly. Most healthcare providers order c-peptide testing as a fasting test, meaning you shouldn't eat or drink anything except water for eight to twelve hours before your blood draw.
Fasting Versus Stimulated Testing
Standard c-peptide tests measure fasting levels, providing a baseline assessment of insulin production. However, some situations call for stimulated c-peptide testing, where you consume a standardized meal or receive a glucagon injection before measurement. This approach reveals how well your pancreas responds to insulin demands.
The stimulated test offers advantages when fasting levels fall into borderline ranges or when providers need to assess remaining beta-cell reserve in people with diabetes. A robust c-peptide response to stimulation suggests meaningful insulin production capacity, while a minimal response indicates advanced beta-cell loss.
What to Expect During Testing
The actual blood draw takes just a few minutes. A healthcare professional will collect a small blood sample from a vein in your arm, typically similar to any standard blood test. The sample gets sent to a laboratory for analysis, with results usually available within one to three days.
Preparation steps:
- Fast for 8-12 hours before your appointment
- Continue taking prescribed medications unless instructed otherwise
- Inform the testing facility about all medications and supplements
- Avoid strenuous exercise before the test
- Stay well-hydrated with water
Similar to other metabolic markers like IGF-1 testing, c-peptide results become most meaningful when interpreted alongside your complete clinical picture, including symptoms, other lab values, and medical history.
C-Peptide and Diabetes Management
Once diagnosed with diabetes, c-peptide monitoring can guide treatment decisions over time. For people with Type 1 diabetes, periodic c-peptide testing helps assess whether any residual beta-cell function remains. This matters because preserving even minimal insulin production can improve glucose control and reduce complications.
Treatment Implications
Your c-peptide level directly influences treatment choices. Low or absent c-peptide indicates absolute insulin requirement, meaning oral diabetes medications alone won't suffice. Conversely, preserved c-peptide production suggests your pancreas retains function that oral medications or lifestyle interventions might support.
The clinical applications of c-peptide measurement extend to predicting diabetes progression and complications risk. People with higher residual c-peptide levels typically experience better glucose control and fewer severe hypoglycemic episodes, even when taking insulin.
Monitoring Disease Progression
Regular c-peptide testing tracks how diabetes evolves over time. In Type 2 diabetes, declining c-peptide levels signal worsening beta-cell function, indicating that treatment intensification may be necessary. This proactive monitoring allows for timely adjustments before glucose control deteriorates significantly.
| Testing Frequency | Clinical Scenario | Purpose |
|---|---|---|
| At diagnosis | New diabetes diagnosis | Classify diabetes type accurately |
| Annually | Type 1 diabetes | Monitor residual beta-cell function |
| Every 2-3 years | Stable Type 2 diabetes | Assess disease progression |
| As needed | Treatment changes | Evaluate therapy effectiveness |
| During hypoglycemia | Unexplained low blood sugar | Identify cause of hypoglycemia |
Special Considerations and Limitations
While c-peptide testing provides valuable information, several factors can affect results or limit interpretation. Understanding these nuances helps you and your healthcare provider make informed decisions based on test outcomes.
Impact of Kidney Function
Kidney disease significantly affects c-peptide levels because your kidneys normally clear this peptide from circulation. Reduced kidney function leads to c-peptide accumulation, potentially creating falsely elevated levels that don't accurately reflect insulin production. If you have chronic kidney disease, your provider must interpret c-peptide results cautiously, often correlating them with other markers.
Medication Interactions
Certain medications influence c-peptide levels by affecting insulin secretion or clearance. Drugs that stimulate insulin release, such as sulfonylureas, can increase c-peptide production. Conversely, medications that suppress beta-cell function might lower levels. Always disclose all medications when undergoing c-peptide testing to ensure accurate interpretation.
Medications affecting c-peptide:
- Sulfonylureas (increase levels)
- Corticosteroids (may alter levels)
- Beta-blockers (can affect secretion)
- Diuretics (may impact clearance)
- Insulin (doesn't affect c-peptide but affects interpretation context)
Accessing C-Peptide Testing
Traditionally, c-peptide testing required a doctor's order and insurance navigation, creating barriers for people seeking answers about their metabolic health. Modern lab testing services now offer more direct access, allowing you to order tests based on your needs and health concerns.
For those exploring testing options, understanding costs and processes helps make informed decisions. Many people appreciate transparent pricing and straightforward ordering, especially when managing chronic conditions like diabetes that require ongoing monitoring.
Questions about test preparation, result interpretation, or choosing appropriate panels are common. Comprehensive FAQ resources can address many concerns about the testing process, turnaround times, and understanding results, making healthcare more accessible and less intimidating.
When to Consider Testing
Consider c-peptide testing if you experience symptoms of diabetes but don't know what type you might have, struggle with unexplained low blood sugar episodes, or want to assess how well your diabetes treatment preserves pancreatic function. The test provides objective data that guides treatment decisions and helps you understand your body's insulin production capacity.
Early and accurate diabetes classification prevents years of potentially inappropriate treatment. Someone with Type 1 diabetes misdiagnosed as Type 2 might spend months or years on oral medications that cannot adequately control blood sugar, leading to preventable complications. Conversely, someone with Type 2 diabetes unnecessarily placed on insulin might experience difficult hypoglycemia and weight gain.
Beyond Diabetes: Other Clinical Applications
While diabetes diagnosis and management represent the primary uses for c-peptide testing, this marker serves additional clinical purposes. Researchers continue discovering new applications as our understanding of insulin metabolism and pancreatic function deepens.
Pancreatic Disease Assessment
C-peptide testing helps evaluate pancreatic function in conditions beyond diabetes. Chronic pancreatitis, pancreatic cancer, and other pancreatic disorders can impair insulin production. Measuring c-peptide provides objective evidence of beta-cell capacity in these contexts, helping guide treatment and monitor disease progression.
Evaluating Insulin Therapy
For people taking insulin, c-peptide testing distinguishes between endogenous (body-produced) and exogenous (injected) insulin. This becomes crucial when investigating hypoglycemia, as high insulin with low c-peptide indicates external insulin administration, while high levels of both suggest endogenous overproduction like an insulinoma.
Clinical scenarios requiring this distinction:
- Unexplained hypoglycemia in people taking insulin
- Suspected factitious hypoglycemia (intentional insulin overdose)
- Determining whether to discontinue insulin therapy
- Assessing beta-cell recovery after acute illness
- Evaluating pancreas or islet cell transplant function
Making Informed Health Decisions
Understanding c-peptide empowers you to participate actively in your healthcare. When you comprehend what tests measure and what results mean, you can ask informed questions, advocate for appropriate testing, and make educated decisions about treatment options.
Knowledge about c-peptide testing proves particularly valuable if you face diagnostic uncertainty, experience treatment challenges, or want to understand your diabetes better. This biomarker provides insights that other tests cannot, filling critical gaps in metabolic assessment that guide personalized care strategies.
The ability to access testing directly, understand results comprehensively, and integrate findings into your health management represents a fundamental shift in healthcare accessibility. Rather than passively receiving diagnoses and prescriptions, you can actively investigate symptoms, monitor conditions, and collaborate meaningfully with healthcare providers based on concrete data.
C-peptide testing offers critical insights for diabetes classification, treatment selection, and ongoing management by accurately measuring your pancreas's insulin production capacity. This simple blood test can distinguish Type 1 from Type 2 diabetes, evaluate unexplained hypoglycemia, and guide personalized treatment strategies that improve outcomes. Whether you're seeking initial diagnosis clarification or monitoring disease progression, Justlabs provides convenient access to c-peptide testing with transparent pricing, no insurance hassles, and results delivered in one to three days, putting essential health information directly in your hands.