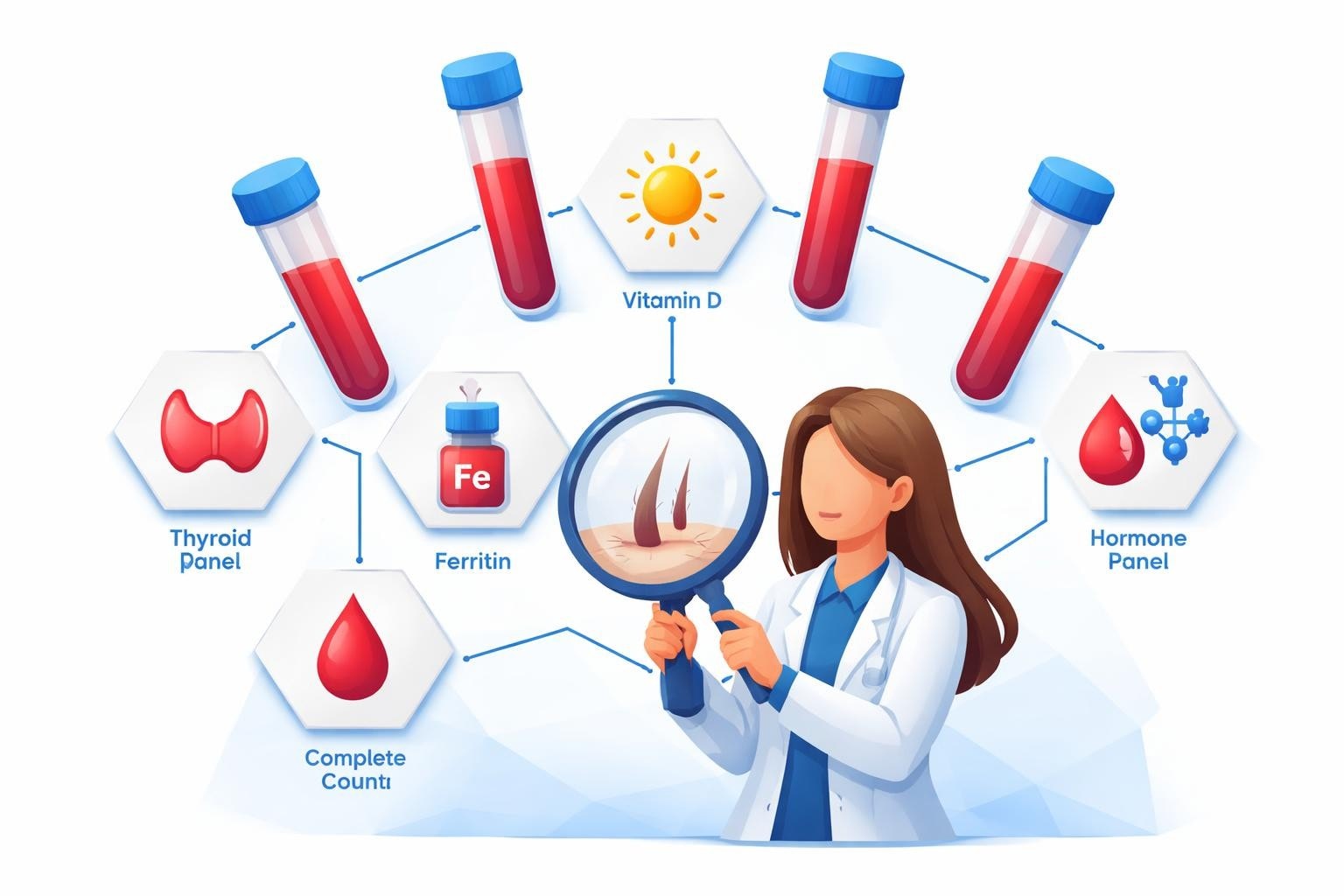
Hair loss affects millions of Americans, creating emotional distress and prompting desperate searches for solutions. While genetics plays a significant role in pattern baldness, many cases of hair thinning stem from treatable medical conditions that only proper diagnostic testing can reveal. Understanding which blood tests for hair loss dermatologists order most frequently empowers you to take control of your hair health and identify reversible causes before permanent damage occurs.
Understanding the Connection Between Blood Work and Hair Health
Hair follicles require specific nutrients, hormones, and optimal bodily conditions to maintain their growth cycle. When deficiencies or imbalances occur, your body prioritizes vital organs over cosmetic functions like hair growth. This biological triage means your scalp becomes one of the first areas to show signs of nutritional inadequacy or hormonal disruption.
Blood testing provides a window into your body's internal environment, revealing hidden deficiencies and imbalances that manifest as hair thinning. Unlike visual scalp examinations or hair pull tests, laboratory analysis offers quantifiable data that guides treatment decisions. Understanding lab results becomes crucial when hair loss is your primary concern, as multiple interconnected factors may contribute simultaneously.
The relationship between blood markers and hair health isn't always straightforward. Some individuals with low-normal ferritin levels experience significant hair loss, while others with similar values maintain full hair density. This variability underscores why comprehensive testing panels provide more valuable insights than single tests.
The Five Essential Blood Tests for Hair Loss
Complete Blood Count with Differential
A complete blood count (CBC) serves as the foundation of hair loss investigation. This comprehensive test evaluates red blood cells, white blood cells, platelets, hemoglobin, and hematocrit levels. Dermatologists order CBCs to screen for anemia, which directly impacts oxygen delivery to hair follicles.
Key markers evaluated in a CBC include:
- Red blood cell count and size
- Hemoglobin concentration
- Hematocrit percentage
- Mean corpuscular volume (MCV)
- Red cell distribution width (RDW)
Low hemoglobin levels indicate anemia, a condition affecting approximately 3 million Americans. When tissues receive insufficient oxygen, non-essential functions like hair production slow down or stop entirely. The various blood tests used to diagnose hair loss often begin with this fundamental screening tool.
Ferritin and Iron Studies
Ferritin testing measures your body's iron storage capacity, which many experts consider the most critical blood test for hair loss. Women experiencing hair thinning frequently have low ferritin levels even when their hemoglobin remains normal. This distinction matters because iron depletion affects hair before causing clinical anemia.
Optimal ferritin levels for hair growth typically exceed 40-50 ng/mL, though laboratory reference ranges often list lower thresholds. Dermatologists specializing in hair disorders commonly recommend ferritin levels above 70 ng/mL for patients experiencing shedding.
| Test Component | Purpose | Optimal Range for Hair Health |
|---|---|---|
| Ferritin | Iron storage assessment | 70-100 ng/mL |
| Serum Iron | Current iron availability | 60-170 mcg/dL |
| TIBC | Iron binding capacity | 250-450 mcg/dL |
| Transferrin Saturation | Iron transport efficiency | 20-50% |
Iron studies provide a complete picture of iron metabolism beyond simple storage measurements. The essential blood tests for hair loss panel always includes comprehensive iron evaluation because supplementation without proper diagnosis can cause dangerous iron overload.
Recommended Test
Ferritin
Ferritin is the best indicator of your body's iron stores. Low ferritin is one of the most common causes of fatigue, especially in women.
Includes 1 biomarkers
$10
Thyroid Function Panel
Thyroid disorders represent one of the most common reversible causes of hair loss. Both hypothyroidism (underactive thyroid) and hyperthyroidism (overactive thyroid) disrupt the hair growth cycle, causing diffuse thinning across the scalp. The thyroid panel examines multiple markers to assess gland function comprehensively.
Standard thyroid testing for hair loss includes:
- Thyroid Stimulating Hormone (TSH) - Primary screening marker
- Free T4 (Thyroxine) - Active thyroid hormone measurement
- Free T3 (Triiodothyronine) - Most potent thyroid hormone
- Thyroid Peroxidase Antibodies (TPO) - Autoimmune marker
- Thyroglobulin Antibodies - Additional autoimmune indicator
TSH levels outside the optimal range of 1.0-2.5 mIU/L may contribute to hair loss even when values remain within standard laboratory ranges. This nuance explains why some patients with "normal" thyroid tests still experience hair improvement after treatment. You can explore thyroid panel costs to understand the investment required for comprehensive thyroid evaluation.
Hashimoto's thyroiditis, an autoimmune condition affecting the thyroid, frequently causes hair loss before other symptoms become apparent. Testing for thyroid antibodies identifies this condition early, allowing intervention before permanent follicle damage occurs.
Recommended Panel
Complete Thyroid Panel
Save $3Our most comprehensive thyroid panel includes all 5 essential markers: TSH, Free T4, Free T3, Reverse T3, and both thyroid antibodies. Get the complete picture of your thyroid health.
Includes 6 biomarkers
$84
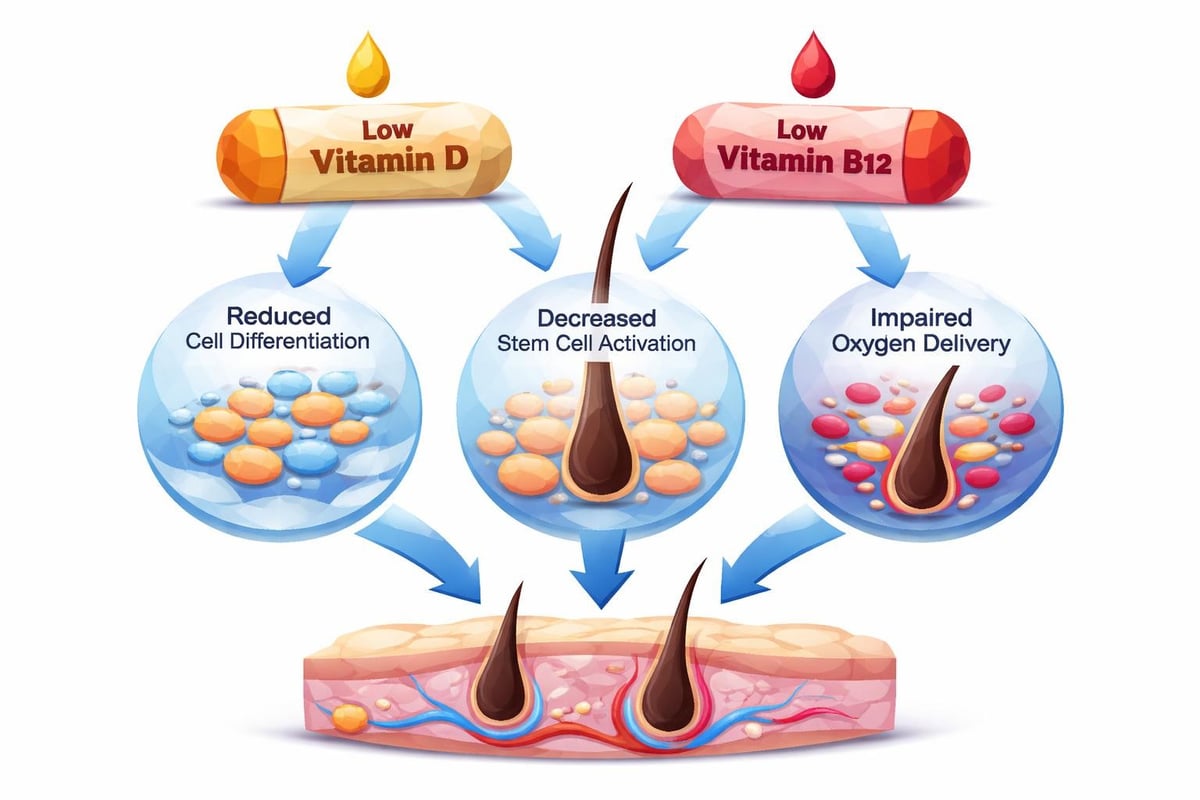
Vitamin D and B12 Levels
Vitamin deficiencies increasingly contribute to hair loss in modern populations spending limited time outdoors and following restrictive diets. Vitamin D receptors exist in hair follicles, and deficiency correlates with various forms of alopecia. Similarly, vitamin B12 supports red blood cell formation and neurological function, both indirectly affecting hair health.
Vitamin D testing measures 25-hydroxyvitamin D levels in your blood. Optimal levels for overall health range between 40-80 ng/mL, though some research suggests higher levels benefit hair growth. Recommended blood tests for diagnosing hair loss frequently emphasize vitamin D assessment given widespread deficiency affecting nearly 42% of American adults.
B12 deficiency warning signs:
- Progressive hair thinning
- Premature graying
- Fatigue and weakness
- Numbness or tingling
- Cognitive difficulties
Vegetarians, vegans, and individuals over 50 face increased B12 deficiency risk. Stomach acid reduction from medications or age-related changes impairs B12 absorption, making supplementation necessary for many people. Testing identifies whether dietary modifications or supplements will effectively address deficiency.
Hormone Panel (Androgens and Sex Hormones)
Hormonal imbalances drive many cases of hair loss, particularly in women experiencing androgen excess. Testing sex hormones and androgens helps identify polycystic ovary syndrome (PCOS), androgen-secreting tumors, and other endocrine disorders manifesting as hair thinning.
The comprehensive hormone evaluation includes:
- Total testosterone
- Free testosterone
- DHEA-S (dehydroepiandrosterone sulfate)
- Sex hormone binding globulin (SHBG)
- Prolactin
- LH and FSH (in women)
Elevated androgens trigger miniaturization of hair follicles in genetically susceptible individuals, the same process underlying male pattern baldness. Women with PCOS often show elevated DHEA-S and testosterone levels alongside irregular periods and unwanted facial hair growth.
Free testosterone provides more clinically relevant information than total testosterone because it represents the biologically active hormone fraction. SHBG levels influence how much testosterone remains free versus bound, affecting tissue exposure to androgens throughout your body.
Recommended Panel
Female Hormone Panel
Save $10This comprehensive panel measures all major female hormones: estrogen, progesterone, reproductive hormones (FSH/LH), and androgens (testosterone/DHEA-S) - essential for understanding hormonal balance.
Includes 7 biomarkers
$89
Who Should Get Blood Tests for Hair Loss
Not everyone experiencing hair shedding requires extensive laboratory testing. Certain patterns and presentations make blood work essential while others respond to observation and conservative management.
You should prioritize blood tests for hair loss if you experience:
- Sudden onset hair thinning without family history
- Diffuse shedding across the entire scalp
- Hair loss accompanied by fatigue or weakness
- Changes in menstrual patterns alongside thinning
- Previous diagnosis of thyroid or autoimmune conditions
- Restrictive diets or malabsorption disorders
Age influences testing decisions significantly. Women experiencing hair loss before menopause benefit more from comprehensive testing than those developing thinning in their 60s or 70s, when age-related changes explain most cases. Similarly, men under 30 with rapid onset hair loss warrant investigation beyond typical male pattern baldness.
The complete diagnostic panel for hair loss becomes particularly valuable when multiple family members experience unexplained hair thinning, suggesting hereditary conditions affecting iron metabolism or autoimmune tendencies.
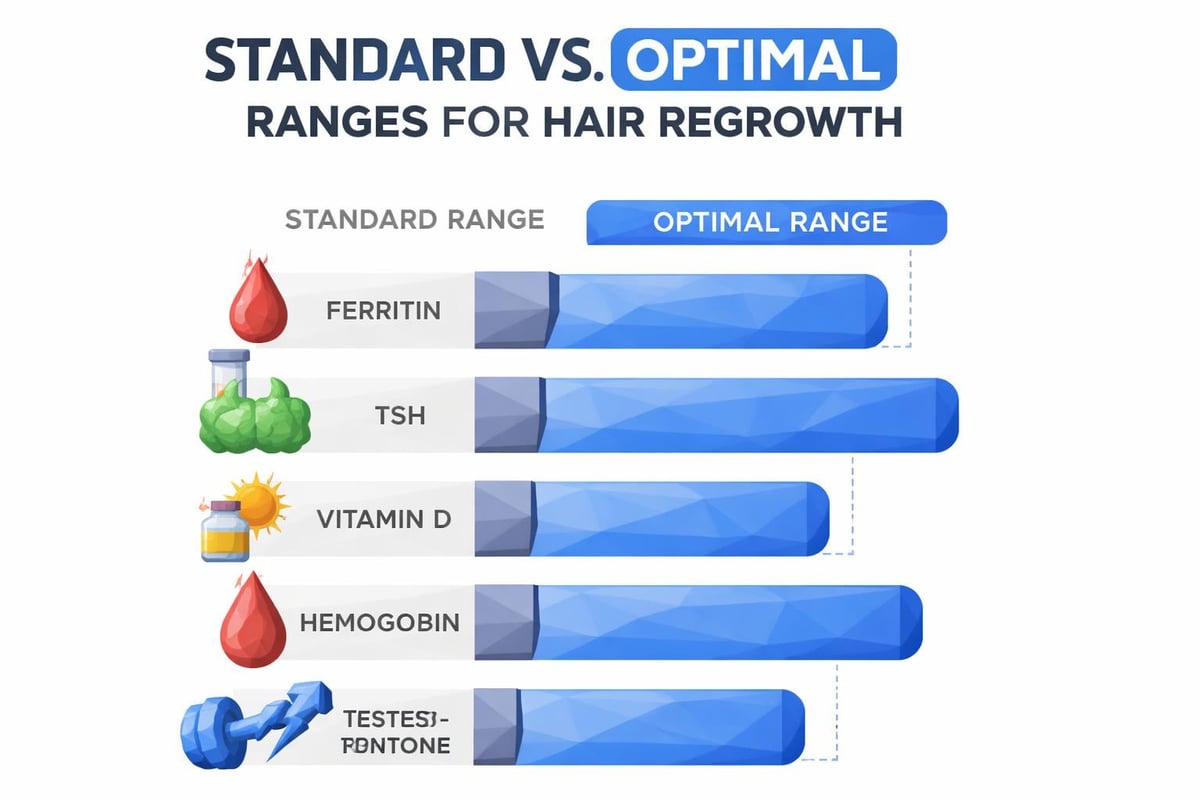
Interpreting Your Blood Test Results
Understanding what your numbers mean empowers better conversations with healthcare providers and more informed treatment decisions. Laboratory reference ranges represent the middle 95% of tested populations, meaning "normal" doesn't always equal "optimal" for hair growth.
Ferritin Interpretation Nuances
Standard ferritin reference ranges often span from 12-150 ng/mL for women and 12-300 ng/mL for men. However, hair loss specialists recognize that values below 40 ng/mL frequently contribute to shedding, and optimal levels for regrowth exceed 70 ng/mL.
If your ferritin measures 25 ng/mL, you're technically within normal range but likely experiencing iron-related hair loss. This discrepancy between laboratory norms and clinical optimization causes confusion when doctors declare results "normal" despite ongoing symptoms.
| Ferritin Level | Laboratory Interpretation | Hair Loss Perspective |
|---|---|---|
| Below 12 ng/mL | Deficient | Severe hair loss likely |
| 12-40 ng/mL | Low-normal | Probable contributor |
| 40-70 ng/mL | Normal | May still affect hair |
| Above 70 ng/mL | Normal | Optimal for regrowth |
Thyroid Function Optimization
TSH represents the pituitary gland's signal to your thyroid requesting hormone production. Higher TSH values indicate your pituitary works harder to stimulate adequate thyroid hormone release, suggesting subclinical hypothyroidism even with normal T4 and T3 levels.
Dermatologists treating hair loss often target TSH levels between 1.0-2.5 mIU/L rather than accepting the broader 0.4-4.5 mIU/L reference range. This tighter control optimizes thyroid function for hair regrowth while maintaining overall health.
Free T3 levels deserve particular attention because T3 represents the most metabolically active thyroid hormone. Some individuals convert T4 to T3 poorly, experiencing symptoms despite adequate T4 levels. Comprehensive thyroid panels revealing this conversion problem guide treatment adjustments.
Getting Tested Without Insurance Barriers
Traditional medical pathways for blood tests for hair loss involve scheduling appointments, obtaining referrals, and navigating insurance pre-authorization. These barriers delay diagnosis and treatment, allowing hair loss to progress while you wait for approval.
Direct-access laboratory testing eliminates these obstacles. Ordering labs without a doctor becomes increasingly popular among individuals seeking timely answers about their health concerns. The self-pay model provides transparent pricing and rapid results without insurance complexity.
Advantages of direct-access testing include:
- Same-day ordering and next-day appointments
- No referral requirements or waiting periods
- Transparent, affordable pricing known upfront
- Results delivered within 1-3 days
- Privacy without insurance records
Cost concerns often prevent people from seeking comprehensive testing through traditional channels. Insurance copays, deductibles, and coinsurance create unpredictable expenses. Lab testing without insurance via self-pay services actually costs less than insured testing for many individuals, particularly those with high-deductible plans.
The ability to view available tests online and select specific panels empowers you to control your healthcare spending. Rather than paying for unnecessary tests bundled into expensive panels, you choose precisely which markers matter for your situation.
Timing and Frequency of Testing
When you schedule blood tests for hair loss significantly impacts result accuracy and clinical utility. Certain markers fluctuate with menstrual cycles, dietary intake, and supplement use, requiring strategic timing for meaningful data.
Optimal Testing Timeline
Schedule your initial comprehensive panel at least 3-6 months after noticing increased shedding. Hair loss often lags behind the triggering event by several months due to the hair growth cycle. Testing too early may miss the causative factor if it resolved before symptoms appeared.
Pre-testing preparation recommendations:
- Stop biotin supplements 3-7 days before testing (interferes with assays)
- Fast 8-12 hours for lipid and glucose accuracy
- Schedule morning appointments for hormone stability
- Avoid iron supplements 24 hours prior
- Maintain normal diet and hydration
Women should ideally test during days 3-5 of their menstrual cycle for hormone accuracy, though other tests remain valid throughout the month. Thyroid and vitamin testing doesn't require specific cycle timing.
Follow-Up Testing Strategy
Retest 3-4 months after starting treatment to assess response and guide adjustments. Ferritin levels improve slowly, often requiring 6-12 months of supplementation to reach optimal ranges. Hair regrowth lags even further behind laboratory improvements, with visible changes appearing 4-6 months after correcting deficiencies.
Monitor thyroid function every 6-8 weeks when initiating or adjusting medication. Once stable, annual testing suffices unless symptoms change. Vitamin D and B12 require less frequent monitoring, typically every 6-12 months depending on supplementation needs.
Treatment Implications of Abnormal Results
Identifying specific deficiencies through blood tests for hair loss enables targeted treatment rather than trial-and-error supplementation. Precision matters because incorrect supplementation causes side effects without addressing the actual problem.
Iron Supplementation Protocols
Low ferritin requires elemental iron supplementation, typically 65-100 mg daily taken with vitamin C for enhanced absorption. Ferrous sulfate, ferrous fumarate, and ferrous gluconate represent common formulations with varying elemental iron content.
Gastrointestinal side effects including constipation, nausea, and dark stools affect many people taking oral iron. Taking supplements with food reduces absorption but improves tolerance. Alternative dosing schedules like every-other-day administration maintain efficacy while minimizing side effects.
Intravenous iron infusions bypass absorption issues, rapidly replenishing stores in patients with malabsorption or severe deficiency. This route particularly benefits individuals with inflammatory bowel disease, celiac disease, or previous gastric surgery affecting nutrient uptake.
Thyroid Hormone Replacement
Hypothyroidism requires thyroid hormone replacement, typically levothyroxine (synthetic T4). Starting doses depend on age, weight, and severity of deficiency, with gradual titration based on follow-up testing. Most patients require 1.6 mcg per kilogram of body weight for full replacement.
Some individuals benefit from combination T4/T3 therapy or natural desiccated thyroid despite T4 monotherapy representing standard treatment. Hair regrowth response varies, with some patients noting improvement within months while others require extended treatment.
Vitamin Supplementation Strategies
Vitamin D deficiency responds to supplementation ranging from 1,000-5,000 IU daily depending on baseline levels and body weight. Larger individuals and those with severe deficiency require higher doses. Vitamin D3 (cholecalciferol) demonstrates superior efficacy compared to D2 (ergocalciferol).
B12 supplementation route depends on deficiency cause. Dietary inadequacy responds to oral supplementation at 1,000 mcg daily, while malabsorption requires sublingual, nasal, or intramuscular administration. Methylcobalamin and cyanocobalamin both effectively raise B12 levels.
Costs and Accessibility Considerations
Understanding testing costs helps you budget for comprehensive hair loss evaluation. Prices vary dramatically between providers, with hospital-based laboratories charging significantly more than independent facilities.
Transparent lab test pricing eliminates billing surprises common in traditional healthcare settings. Knowing exact costs before testing allows informed financial planning and prevents unexpected charges months later.
Individual test costs typically range as follows:
- Complete Blood Count: $15-30
- Ferritin: $20-40
- Comprehensive Thyroid Panel: $50-150
- Vitamin D: $25-50
- Hormone Panel: $75-200
Bundled panels offering multiple related tests often provide better value than ordering individually. A comprehensive hair loss panel including all five essential test categories might cost $200-400 through direct-access services versus $800-1,500 through traditional medical channels.
Many people don't realize FSA and HSA funds cover eligible tests, making self-pay testing more affordable. These tax-advantaged accounts reimburse laboratory expenses without requiring insurance claims or provider authorization.
Blood tests for hair loss provide essential diagnostic information that separates treatable medical conditions from genetic balding requiring different management approaches. By identifying specific deficiencies and imbalances through comprehensive testing, you can pursue targeted treatment with confidence rather than guessing at causes. When you're ready to take control of your hair health through accessible, affordable testing, Justlabs offers the comprehensive panels discussed in this article with transparent pricing, convenient online ordering, and results delivered within 1-3 days-no doctor's appointment or insurance required.