Persistent bloating affects millions of Americans, yet many suffer for years without discovering the underlying cause. While occasional abdominal distension is common after large meals, chronic bloating that interferes with daily life deserves medical attention. Among the various conditions that can trigger ongoing digestive discomfort, celiac disease stands out as one of the most underdiagnosed culprits. This autoimmune disorder affects approximately 1 in 100 people worldwide, yet studies suggest that up to 80% of cases remain undiagnosed. Understanding the connection between bloating and blood tests specifically designed to detect celiac disease can empower individuals to take control of their digestive health.
Understanding the Link Between Celiac Disease and Bloating
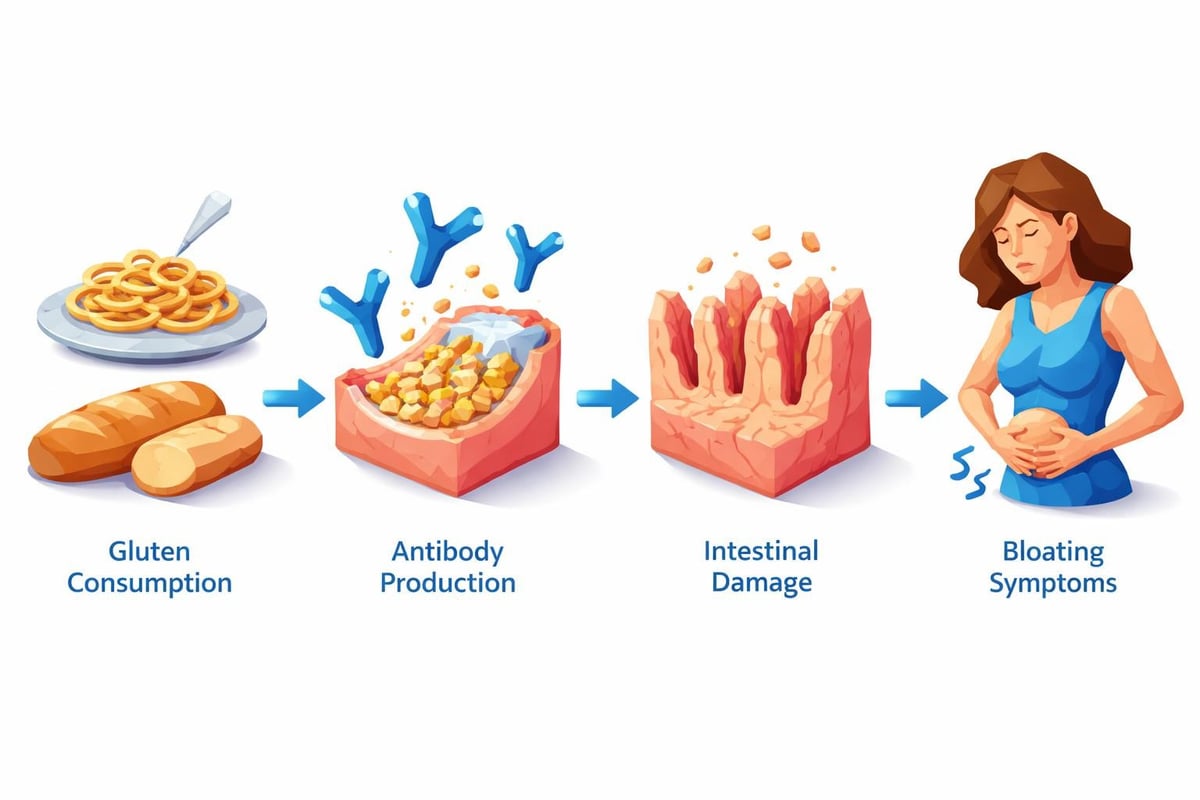
Celiac disease triggers an immune response when gluten proteins from wheat, barley, and rye enter the digestive system. This reaction damages the small intestinal lining, specifically the villi, which are tiny finger-like projections responsible for nutrient absorption. As these structures become inflamed and flattened, the digestive process becomes compromised.
Bloating emerges as one of the hallmark symptoms because damaged intestinal tissue cannot properly process food. According to research on bloating prevalence, abdominal distension affects a significant portion of the global population, with various underlying causes. In celiac disease patients, several mechanisms contribute to this uncomfortable sensation:
- Malabsorption of nutrients leading to bacterial fermentation in the intestines
- Inflammation of the intestinal wall causing fluid retention
- Altered gut motility resulting in gas accumulation
- Disrupted digestive enzyme production preventing proper food breakdown
The bloating associated with celiac disease often worsens after consuming gluten-containing foods, though symptoms may appear hours or even days later. This delayed response makes it challenging for individuals to identify the connection without proper testing.
Why Celiac Disease Remains Underdiagnosed
Despite being relatively common, celiac disease frequently goes undetected for years or even decades. The average time from symptom onset to diagnosis is approximately six to ten years in the United States. Several factors contribute to this diagnostic delay:
Symptom variability presents the primary challenge. While some patients experience severe digestive symptoms including chronic diarrhea, others have minimal gastrointestinal complaints. Some individuals primarily exhibit non-digestive symptoms such as fatigue, joint pain, or skin rashes, making the connection to celiac disease less obvious.
Medical misconceptions also play a role. Healthcare providers may not immediately consider celiac disease when patients present with bloating alone, particularly if other classic symptoms are absent. Many physicians still associate the condition primarily with childhood presentation and severe malnutrition, overlooking adult-onset cases with subtler manifestations.
The accessibility barrier creates another obstacle. Traditional healthcare pathways require scheduling appointments, obtaining referrals, and navigating insurance authorization processes. For individuals seeking answers about persistent bloating, these hurdles can discourage timely testing. Services offering lab tests without insurance provide alternative access points for concerned individuals.
Essential Blood Tests for Celiac Disease Detection
When evaluating bloating and blood tests for celiac disease, several specific antibody markers provide diagnostic information. These tests detect the immune system's abnormal response to gluten proteins, offering a non-invasive screening method before proceeding to more invasive procedures.
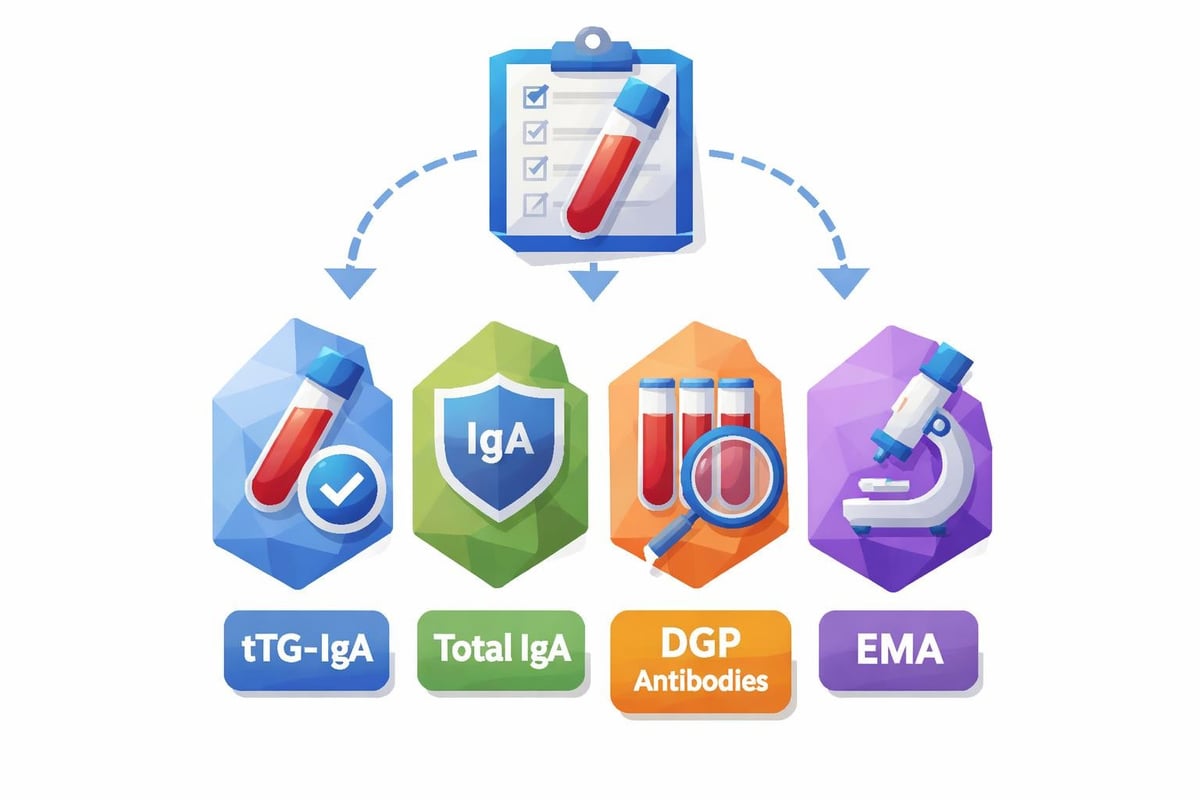
Tissue Transglutaminase Antibody (tTG-IgA)
This test represents the primary screening tool for celiac disease. It measures IgA antibodies against tissue transglutaminase, an enzyme that becomes a target in the autoimmune response triggered by gluten. The tTG-IgA test demonstrates high sensitivity and specificity, making it the most reliable single blood test for celiac disease detection.
| Test Component | Purpose | Accuracy Level |
|---|---|---|
| tTG-IgA | Primary screening antibody | 90-95% sensitivity |
| Total IgA | Confirms IgA production capability | Identifies IgA deficiency |
| DGP-IgG | Alternative for IgA-deficient patients | 85-90% sensitivity |
| EMA-IgA | Confirmatory testing | 95-98% specificity |
Total Serum IgA
This companion test ensures that the body produces adequate IgA antibodies. Approximately 2-3% of celiac disease patients have selective IgA deficiency, which would produce false-negative results on IgA-based tests. Testing total serum IgA levels helps identify these individuals, prompting healthcare providers to use alternative IgG-based tests instead.
Deamidated Gliadin Peptide Antibodies (DGP-IgA and DGP-IgG)
These tests detect antibodies against gliadin, a component of gluten. The deamidated form shows improved accuracy compared to older gliadin antibody tests. DGP-IgG becomes particularly valuable for patients with IgA deficiency, offering an alternative screening pathway. Some laboratories include both IgA and IgG versions in comprehensive celiac panels.
Endomysial Antibody (EMA-IgA)
This highly specific test detects antibodies against endomysium, the connective tissue surrounding muscle fibers. While extremely accurate when positive, the EMA-IgA test costs more and requires specialized laboratory techniques. Healthcare providers typically use it as a confirmatory test rather than initial screening.
Preparing for Celiac Disease Blood Tests
Proper preparation significantly impacts the accuracy of bloating and blood tests for celiac disease. Unlike some laboratory tests that require overnight fasting, celiac antibody tests have a critical dietary requirement that surprises many patients.
Continue eating gluten before testing. This counterintuitive instruction is essential because celiac antibody levels decrease rapidly once gluten is removed from the diet. Patients who have already started a gluten-free diet may need to undergo a "gluten challenge," consuming gluten-containing foods for several weeks before testing to ensure accurate results.
Healthcare providers generally recommend:
- Maintain normal gluten intake for at least six to eight weeks before testing
- Consume gluten daily equivalent to 2-4 slices of wheat bread
- Avoid starting elimination diets before completing testing
- Document symptoms to help correlate test results with clinical presentation
For individuals exploring self-directed testing options, understanding how to order labs without a doctor can streamline the process while maintaining testing accuracy.
Interpreting Your Celiac Disease Blood Test Results
Understanding test results requires consideration of reference ranges, antibody levels, and clinical context. Laboratory reports typically indicate whether results fall within normal ranges, but interpretation extends beyond simple positive or negative designations.
Positive Results
Elevated antibody levels suggest active celiac disease, but confirmation typically requires endoscopic biopsy of the small intestine. Blood tests demonstrate high accuracy, yet intestinal biopsy remains the diagnostic gold standard. The diagnostic process for digestive conditions often involves multiple testing modalities to establish definitive diagnoses.
Strong positive results (antibody levels significantly above reference ranges) correlate with higher likelihood of villous atrophy on biopsy. Patients with markedly elevated tTG-IgA levels often show extensive intestinal damage requiring immediate dietary intervention.
Negative Results
Normal antibody levels generally indicate celiac disease is unlikely, particularly when total IgA levels are adequate. However, negative results do not completely exclude the diagnosis in all circumstances:
- Patients with IgA deficiency require IgG-based testing
- Individuals already following gluten-free diets may show falsely negative results
- Early-stage disease occasionally presents with normal antibody levels despite intestinal changes
Borderline Results
Antibody levels near the upper limit of normal ranges create interpretive challenges. These borderline results may indicate early celiac disease, potential celiac disease susceptibility, or testing variability. Repeat testing after several months of continued gluten consumption often clarifies ambiguous initial results.
Beyond Celiac Disease: Other Conditions Requiring Blood Test Evaluation
While celiac disease represents a significant cause of chronic bloating, other conditions detected through blood testing may contribute to persistent abdominal symptoms. Comprehensive evaluation of bloating and blood tests should consider these alternative diagnoses.
Thyroid Disorders
Both hypothyroidism and hyperthyroidism can alter digestive motility, leading to bloating and constipation or diarrhea. A thyroid panel measuring TSH, T3, and T4 levels helps identify thyroid dysfunction. Hypothyroidism slows intestinal transit time, allowing increased bacterial fermentation and gas production.
Small Intestinal Bacterial Overgrowth (SIBO)
While primarily diagnosed through breath testing, certain blood markers can suggest conditions predisposing to SIBO. Research on gas retention and bloating mechanisms demonstrates how bacterial overgrowth contributes to symptom generation. Blood glucose levels, diabetes screening, and inflammatory markers provide context for SIBO risk assessment.
Food Intolerances and Allergies
Lactose intolerance rarely requires blood testing, but some individuals benefit from genetic testing that identifies lactase persistence or non-persistence. True food allergies produce IgE antibodies detectable through blood tests, though these typically cause more acute reactions than chronic bloating.
| Condition | Relevant Blood Tests | Associated Bloating Pattern |
|---|---|---|
| Celiac Disease | tTG-IgA, DGP, EMA | Worsens with gluten intake |
| Hypothyroidism | TSH, Free T4 | Persistent, with constipation |
| Inflammatory Bowel Disease | CRP, ESR, fecal calprotectin | Variable, with pain |
| Ovarian Issues | CA-125, hormone panels | Cyclical or progressive |
The Role of Direct-Access Laboratory Testing
Traditional healthcare pathways create barriers for individuals experiencing persistent bloating who want answers quickly. Extended wait times for specialist appointments, insurance requirements, and referral processes delay diagnosis and treatment initiation. Understanding evaluation approaches for gas and bloating emphasizes the importance of timely diagnostic testing.
Direct-access laboratory services transform this landscape by offering immediate testing availability without physician referrals. Individuals concerned about bloating and blood tests for celiac disease can initiate screening independently, receiving results within days rather than weeks or months.
Cost transparency represents another significant advantage. Traditional laboratory billing through insurance often involves surprise charges, confusing explanation of benefits statements, and unexpected out-of-pocket expenses. Self-pay laboratory services provide upfront pricing, allowing informed decision-making about testing investments.
Comprehensive test selection empowers patients to choose appropriate panels based on their symptoms and concerns. Rather than limiting tests to insurance-approved options, individuals can select comprehensive panels that address multiple potential causes simultaneously.
The convenience factor cannot be overstated. With thousands of collection sites nationwide, patients can complete blood draws at locations and times that fit their schedules. Results typically become available through secure online portals within one to three business days, expediting the path from symptoms to answers.

When to Pursue Blood Testing for Bloating
Not every instance of bloating warrants immediate laboratory investigation. Understanding when symptoms cross the threshold from normal digestive variation to potential medical concern helps individuals make informed testing decisions.
Red Flag Symptoms Requiring Evaluation
Several warning signs suggest bloating stems from underlying medical conditions rather than dietary indiscretion or stress:
- Persistent symptoms lasting more than two weeks despite dietary modifications
- Progressive worsening of abdominal distension over weeks or months
- Unintentional weight loss accompanying digestive symptoms
- Blood in stool or black, tarry stools
- Severe pain that disrupts daily activities
- Family history of celiac disease, inflammatory bowel disease, or colon cancer
Research on intestinal pseudo-obstruction diagnosis highlights how severe bloating may indicate serious motility disorders requiring comprehensive medical evaluation.
Chronic But Stable Symptoms
Many individuals experience chronic bloating without alarming features. These cases still merit investigation, particularly when symptoms affect quality of life, work productivity, or social activities. The threshold for testing should balance symptom impact against individual preferences for diagnostic certainty.
Pattern recognition helps identify potential celiac disease. Bloating that consistently worsens after consuming bread, pasta, pizza, or baked goods suggests gluten sensitivity or celiac disease. Keeping a detailed food and symptom diary for two weeks often reveals these patterns.
What Happens After Positive Celiac Disease Blood Tests
Receiving positive results on bloating and blood tests for celiac disease initiates a multi-step diagnostic and treatment process. While elevated antibodies strongly suggest the condition, additional testing typically precedes definitive diagnosis and treatment initiation.
Confirmatory Testing Through Endoscopy
Gastroenterologists perform upper endoscopy with small intestinal biopsy to visualize and sample tissue from the duodenum. This procedure confirms villous atrophy and identifies the extent of intestinal damage. Multiple tissue samples from different intestinal locations provide comprehensive assessment of disease severity.
The biopsy results are graded using the Marsh classification system, ranging from normal tissue (Marsh 0) to complete villous atrophy (Marsh 3c). Higher grades indicate more extensive damage and often correlate with more severe symptoms and nutritional deficiencies.
Nutritional Assessment
Years of undiagnosed celiac disease often result in vitamin and mineral deficiencies due to malabsorption. Comprehensive blood work typically includes:
- Iron studies to assess for anemia
- Vitamin D levels frequently depleted in celiac patients
- Vitamin B12 and folate to evaluate absorption capacity
- Bone density screening for patients with long-standing disease
- Liver function tests as some patients develop elevated liver enzymes
Genetic Testing Considerations
While not required for diagnosis, genetic testing for HLA-DQ2 and HLA-DQ8 provides additional information. Approximately 95% of celiac disease patients carry one or both of these genetic markers. Negative genetic testing essentially rules out celiac disease, making it useful in ambiguous cases.
Dietary Management and Symptom Resolution
The cornerstone of celiac disease treatment involves strict, lifelong adherence to a gluten-free diet. This dietary modification eliminates the antigenic trigger, allowing intestinal healing and symptom resolution. Most patients notice significant improvement in bloating within weeks of gluten elimination.
Label reading becomes essential as gluten hides in unexpected products including sauces, processed meats, and medications. Many manufacturers now clearly label gluten-free products, simplifying grocery shopping. However, cross-contamination during food preparation requires ongoing vigilance.
Nutritional adequacy presents challenges during the transition to gluten-free eating. Many gluten-free products lack fortification with B vitamins and iron commonly added to wheat-based foods. Working with registered dietitians specializing in celiac disease helps ensure balanced nutrition while maintaining strict gluten avoidance.
Social and practical considerations affect adherence. Dining out, traveling, and social gatherings require planning and communication about dietary needs. Support groups and celiac disease organizations provide resources, recipes, and community connections that ease the transition.
Monitoring Disease Activity Through Follow-Up Testing
After diagnosis and dietary intervention, periodic blood testing monitors treatment effectiveness and dietary compliance. Follow-up celiac antibody testing typically occurs three to six months after initiating a gluten-free diet, then annually thereafter.
Expected Antibody Decline
Antibody levels should decrease progressively on a strict gluten-free diet. The tTG-IgA typically normalizes within 6-12 months, though individual timelines vary based on initial antibody levels and disease severity. Persistent elevation suggests ongoing gluten exposure, either intentional or from hidden sources.
Some patients achieve clinical remission with symptom resolution but maintain mildly elevated antibodies. These cases require careful evaluation to identify potential gluten contamination sources and assess the need for repeat endoscopy.
Long-Term Health Monitoring
Beyond antibody testing, patients with celiac disease require periodic assessment of:
- Nutritional status including vitamin and mineral levels
- Bone density screening every 1-2 years initially
- Thyroid function as autoimmune conditions often cluster
- Liver enzymes to detect persistent inflammation
Research examining dietary fat types and bloating associations demonstrates how various dietary factors beyond gluten can influence digestive symptoms, emphasizing the need for comprehensive nutritional management.
Accessing Affordable Testing Options
Cost concerns prevent many individuals from pursuing needed diagnostic testing. Understanding pricing structures and payment options removes financial barriers to health information. Traditional hospital-based laboratory services often charge significantly more than independent testing facilities, with prices varying dramatically based on location and billing practices.
Transparent pricing models allow budget planning and informed decision-making. When individuals know exact costs upfront, they can prioritize testing based on symptom severity and financial resources. Many comprehensive celiac panels cost less than anticipated, particularly through self-pay laboratory services that eliminate insurance markup and administrative fees.
HSA and FSA eligibility makes laboratory testing more affordable for individuals with health savings accounts or flexible spending arrangements. Understanding FSA and HSA eligible tests helps maximize tax-advantaged healthcare dollars for diagnostic purposes.
Price comparison between providers reveals substantial cost differences for identical tests. A celiac panel through hospital outpatient laboratory services might cost $400-800 or more, while the same tests through direct-access services often run $100-200. These savings become particularly significant for individuals without insurance coverage or those with high-deductible health plans.
Taking Control of Your Digestive Health
Persistent bloating deserves investigation rather than resignation. While occasional digestive discomfort represents normal physiologic variation, chronic symptoms that interfere with daily life warrant medical attention. The connection between bloating and blood tests, particularly for celiac disease screening, offers a pathway to answers and relief.
Modern laboratory access removes traditional barriers to diagnostic testing. Individuals no longer need to wait weeks for appointments or navigate complex insurance authorizations before seeking answers about their symptoms. Self-directed testing empowers patients to initiate evaluation processes, bringing results and concerns to healthcare providers for collaborative treatment planning.
Understanding which tests to order, how to interpret results, and what follow-up steps to take transforms passive symptom tolerance into active health management. Whether ultimately diagnosed with celiac disease, other digestive conditions, or finding reassurance through negative results, laboratory testing provides valuable information for decision-making.
The underdiagnosis of celiac disease represents a significant public health concern, leaving millions suffering unnecessarily with preventable symptoms and complications. Increased awareness of the connection between chronic bloating and this treatable condition, combined with accessible testing options, can identify previously unrecognized cases and improve quality of life for affected individuals.
Understanding the relationship between bloating and blood tests opens pathways to diagnosis and relief for conditions like celiac disease that might otherwise remain undetected for years. If you're experiencing persistent abdominal discomfort and want answers without the hassle of insurance authorization or lengthy appointment scheduling, Justlabs offers convenient access to comprehensive celiac panels and other diagnostic tests with transparent pricing and results available in just 1-3 days. Take control of your digestive health today by ordering the tests you need to identify the root cause of your symptoms.